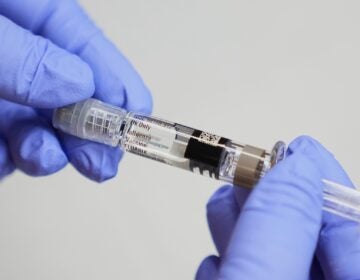
Flu count continues to rise in Pa., N.J., and Del.
This past week, Pennsylvania counted almost 9,000 cases of the flu. That’s up from the week prior, when 8,000 people were tallied.
Listen 1:38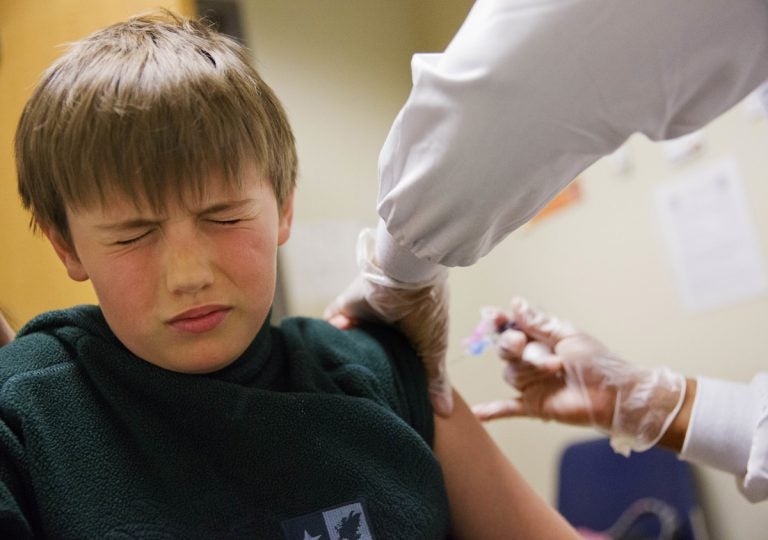
Reed Olson, 8, gets a flu shot, Monday, Feb. 5, 2018. The U.S. government's latest flu report released on Friday, Feb. 2, 2018, showed flu season continued to intensify the previous week, with high volumes of flu-related patient traffic in 42 states, up from 39 the week before. (David Goldman/AP Photo)
This past week, Pennsylvania counted almost 9,000 cases of the flu. That’s up from the week prior, when 8,000 people were tallied. There were also 26 flu related deaths. In part, that’s because this year’s vaccine may not have been as effective as in years past. But scientists and doctors are still recommending it because even though the vaccine may not work to prevent people from getting the flu, it can prevent it from becoming fatal.
Each year, the World Health Organization collects and uses data to predict which strain of the flu will be the most popular and develop a vaccine that prevents it. Scott Hensley studies what influences flu vaccine effectiveness at Penn’s Perelman School of Medicine. He says, sometimes they guess wrong.
“A lot can happen between when these recommendations are made and when the flu season actually occurs,” Hensley said. But, based on his research, that’s not exactly what happened this year. It’s true that the vaccine designed to immunize against the H3N2 virus, the most prevalent strain, looks different from the virus itself. But that’s not so much because they made the wrong forecast.
“We think that this year, the vaccine — the H3N2 vaccine — might have less than ideal effectiveness because the vaccine strain changed in the manufacturing process,” said Hensley.
It’s industry standard to cultivate flu vaccines in chicken eggs. But Hensley says that the most common flu strain is bad at binding to the cells of chicken eggs — to do so, the culture has to adapt and mutate. By the time the vaccine is cultivated, it looks really different from the virus that’s floating around among people — different enough that it might not serve as an effective vaccine. Hensley noted that around 10 percent of flu vaccines are cultivated using methods other than chicken eggs, and although it would require research funding, that is the direction he believes we need to head if we want to avoid the problem in the future.
“If we have H3 viruses next year, it’s going to be a major problem next year, too,” he said.
Getting vaccinated may not protect people from getting the flu, but it could prevent the flu from becoming fatal, says Hensley. The Centers for Disease Control and Prevention only counts flu deaths among children. It reports that in years past, 80 percent of children who died from the flu were not vaccinated. The CDC estimates roughly 36,000 people die from the flu each year.
So far this year, there have been 91 flu related deaths in Pennsylvania. Delaware’s department of health reports four deaths so far, and New Jersey, which also only counts pediatric deaths from the flu, reports one fatality.
Pennsylvania does not separate its reported deaths by those who had been vaccinated and those who hadn’t. It does classify “flu-associated deaths” without distinguishing between those who died as a direct result of the virus, and those who died as a result of a secondary infection like bacterial pneumonia, which commonly takes root in a compromised immune system.
Kevin Alby, director of Clinical Microbiology at the University of Pennsylvania, says that makes it very difficult to know how many people are actually dying from the flu each year. The CDC does not require states to report deaths, so data is inconsistent, and it’s easy for someone who may die from a respiratory disorder that they already had and which was exacerbated by the flu, to go overlooked in the flu-related death tally.
Alby says there is a relationship between a mismatched vaccine and more flu-associated deaths.
“You definitely see more deaths in more severe seasons, so you would tend to see more severe seasons in years where the vaccine isn’t as efficacious,” he said.
As for how people are actually dying from the flu, some are from those secondary infections or existing conditions. But in some cases, the body just responds to the virus almost too well.
“The body is seeing lots of virus it’s trying to fight,” Alby explained. “It’s doing everything it can to fight off the virus to the detriment of the rest of the body — the chemicals and the things that the body uses to attack the virus or the infected cells can also damage healthy cells.”
So what causes one person’s body to react so aggressively to the virus that it damages its healthy tissue, while another person has a more balanced response?
“We don’t have great predictors as to, OK this person is at high risk for developing significant, almost over-reactive immune dysfunction,” said Alby. “We don’t really know.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.