A look at how antibodies from a COVID-19 infection and vaccination wane over time
Penn Med researchers found that memory T and B cells play a significant role in fighting COVID-19 even 6 months after vaccination.
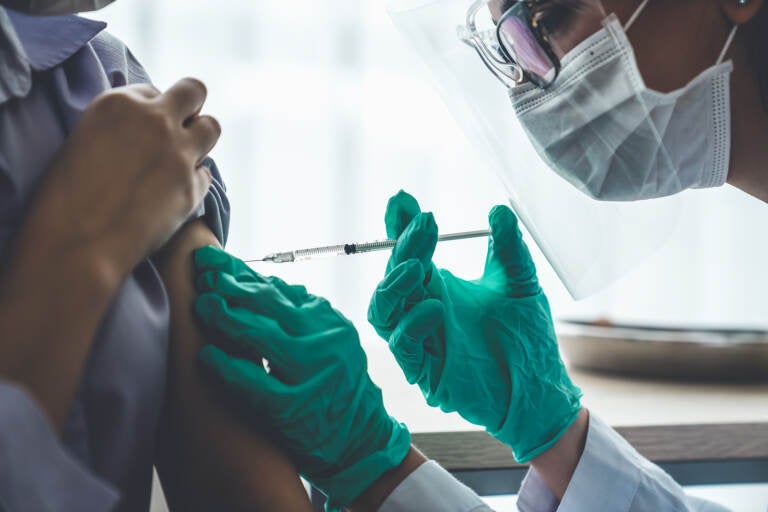
COVID-19 vaccine clinic. (World Image / BigStock)
Since the COVID-19 vaccines have rolled out, there’s been a lot of talk about the production of antibodies and how it correlates to the effectiveness of the shot — as well as how it protects people who had actual coronavirus infections.
Though antibody responses are important to prevent viruses from invading the body, memory B and T cells play a significant role when fighting infection, according to researchers at the University of Pennsylvania. They followed people fully vaccinated with mRNA vaccines (Pfizer or Moderna) — some of whom never had COVID-19 and others who had previously had the virus — to measure their immune responses.
As expected, antibodies waned over time, but memory B and T cells persisted for at least six months, which might suggest steady and durable protection from severe disease and hospitalization as a result of the virus, according to the Penn Medicine study published in Science.
Waning immunity has been a hot topic in recent months as breakthrough COVID infections, though rare, have been reported, and as boosters have been recommended for certain groups of people whose immune responses become less robust over time.
“One of the things that we’re hoping for is to shine a spotlight on things beyond antibody … we want to make sure that we’re not forgetting that there are other components of the immune system that work in concert with antibodies, and it will be important to measure those in different populations and to incorporate them in how we’re thinking about the need for boosters, the need for vaccines in different populations, and how we go forward in thinking about other kinds of vaccines, even after SARS-CoV-2,” said Dr. John Wherry, director of the Penn Institute of Immunology, who helped lead the study.
“We want to try to make sure that we and others can perform these kinds of assays over a longer time frame — a year or two years — to understand this durability, and how that might be important in understanding the transition from SARS-CoV-2 as a pandemic virus to something that we likely will be living with for a long time; SARS-CoV-2 as an endemic or a seasonal virus.”
Antibodies are proteins made by the immune system that circulate in the blood, nasal passages, lungs and areas of entry for viruses, and they act as a shield to prevent viruses from invading the body. Though they are an important component of infection prevention, antibodies usually decline over time, and sometimes they don’t work as well when viruses change or mutate.
The effectiveness of the COVID-19 vaccine often is correlated with the production of antibodies. But there are other parts of the immune system that can help fight the virus.
The vaccine can also boost memory B cells, which are cells that can make antibodies. They circulate in the blood and are ready to help people fight infections. If a person does get infected, or receives a booster vaccine, those memory B cells quickly become activated, and within a couple days they make a new set of high-quality antibodies to help eliminate the virus and prevent it from spreading around the body.
The immune system also generates memory T cells that detect and tackle viruses once inside the body.
Memory B cells and memory T cells can’t function like a shield the way antibodies do. But once a virus invades the body, these cells prevent the virus from spreading and from getting deep in the lungs, which could cause pneumonia and severe respiratory symptoms.
“The immune system divides and conquers the things that are important for giving us optimal protection,” Wherry said.
“We often think about antibodies as being what protects us, and even talk about antibodies as the correlate of protection … But that correlate doesn’t mean that other parts of the immune system aren’t also important in limiting infection. When you have high levels of antibodies, you tend to also have good memory B cells and good T-cells. So all parts of the immune system can play a really important role in coordinating that optimal protection,” he said.
The Penn team wanted to study memory B and T cells because there’s very little data examining their long-term (in this case, six months) responses following vaccination. There’s a lot of data about antibodies, though, and many studies show antibody levels decline over time.
Among the study participants who had never had COVID-19, vaccines initially induced very robust antibody and memory B and T cell responses.
Following the first dose, these participants developed an initial T-cell response, and after the second dose, their T-cells helped their B cells to produce a robust response. Study participants achieved high levels of antibodies very soon after getting the shot.
Over time, T cells and B cells meet in the lymph nodes and form what immunologists call a “germinal center;” that’s where memory B cells improve over time, including the quality of the antibodies they make. That reaction can take eight to 15 weeks.
The Penn researchers found that though initial antibodies waned over time, memory B cells actually got better as time went on, and produced antibodies with improved quality than before.
Wherry said that finding might suggest why some people have mild breakthrough infections — the waning antibodies mean people are more vulnerable to catching COVID-19 in the first place, but the improved memory B cells prevent that person from getting severe illness.
“We’ve seen some waning of immunity over time, that’s pretty clear, but the glass is still half-full here. The amount of immunological memory we have is still quite robust,” Wherry said.
“It does look like the vaccines are doing what we all would have initially hoped,” he said. “They’re preventing people from getting severely sick and dying. They’re keeping our health system functioning, because we aren’t sending a lot of vaccinated people to the hospital. They’re providing an opportunity, we think, to limit transmission in vaccinated people, so vaccinated people aren’t spreading, so even those people who are vulnerable, who can’t be fully vaccinated, are being protected because the vaccines are preventing severe infection and preventing prolonged infection in most people and very likely dramatically limiting the spread.”
The study also found that memory B cells boosted after vaccination responded to variants of the coronavirus.
Its findings suggest that booster shots will reactivate memory B cells, sparking an effective new immune response, Wherry said.
What the study’s findings could mean for booster recommendations still is up in the air, Wherry said. And there are strong arguments for and against boosters. People over 65, people with certain health conditions, and people who work or live in settings that put them at risk for catching COVID-19 currently are eligible for boosters at least six months after getting the second dose of the Pfizer vaccine. Centers for Disease Control and Prevention approval for Moderna and Johnson & Johnson boosters is likely to come soon.
“There’s no question that what we need to do is vaccinate people who are unvaccinated, or vaccinate people who don’t have immunity from infection,” Wherry said. “That’s how we’re going to stop transmission. That’s how we’re going to end the pandemic. And it’s very likely that vaccinated people or people who previously had COVID are not spreading the virus very much … So at the public health level, boosters are not going to change the trajectory of the pandemic very much.”
On the other hand, boosters might benefit people who don’t want to be taken out of work or school for a few days or to be quarantined, he said.
Wherry thinks that boosters for healthy adults should be optional. But immunocompromised people, older people, and other vulnerable populations could prevent severe illness by getting booster shots, he said. For many immunocompromised people, particularly those who don’t produce sufficient antibodies following two doses of the vaccine, boosters are important.
What Penn’s recently published study means for immunocompromised people is that antibodies aren’t the be all and end all — that memory B and memory T cells play a key role.
Still, it’s important to note that not all immunocompromising conditions are the same, Wherry said. The aspect of the immune system that is compromised, and to what degree, differs from person to person. Wherry said many immunocompromised individuals should get boosters, but should talk to their doctors first.
“I think the idea that it’s one size fits all probably isn’t quite right … Many of our immunocompromised populations may still have T cell responses. Maybe some of them have memory B cell responses as well, but just suboptimal antibodies,” he said.
Studying the immune responses of people with immune-compromising conditions could lead to the production of post-exposure medications that help prevent infection, Wherry said. He added it’s crucial that the public consider getting vaccinated to protect immunocompromised people who could still get severely ill from COVID-19 even after vaccination.
Responses in those who’d already had COVID-19
In evaluating immune responses to the vaccine among people who had previous COVID-19 infections, the Penn researchers found that getting vaccinated boosted their antibody responses, but that the vaccine had only a modest impact on the boosting of memory B and T cells.
Immunity from natural infection is quite good, but the data on that is mixed. A study from Israel suggests that immunity from infection might be slightly better than after vaccination, while other studies conclude that protection from natural infection is equivalent to or even slightly lower than protection from vaccines.
“The immunity following infection is much more variable than it is following vaccination. And so there’s a lot of data that the level of antibodies generated following infection, especially mild infection, can be lower than you would get following vaccination … So the recommendation is still that people who were previously infected should get vaccinated,” Wherry said.
An earlier Penn study suggests that just one dose of an mRNA vaccine might provide sufficient protection for people who previously had COVID-19. That’s not the official recommendation yet, however.
“I think the other question is: How do you know that you have good enough immunity following infection? And that’s very difficult to do. There aren’t really good tests to know how immune you are. We don’t know how long immunity following infection lasts. We are starting to get an idea how long immunity following vaccination lasts. So there are more variables with immunity following infection than there are with immunity following vaccination,” Wherry said.
“Some will say that immunity from infection might be better because you make immune responses to other parts of the virus. You do indeed make immune responses to other parts of the virus that are not contained in the vaccine. But the only antibody responses that will prevent infection are the antibodies to spike that you generate following vaccination or infection. The immune responses generated following infection to other parts of the virus may limit severe disease, but they’re not going to prevent these initial infection events,” he said.
“The bottom line is that most of the data looking at protection from infection or protection from disease say that the protection afforded by infection is close to what you get following vaccination. But questions about variability and durability remain.”
There were some limitations in Penn’s new study. There only were 61 participants, and they were largely young or middle-aged — more research among older people needs to be conducted. It’s also important to note that measuring immune responses is not the same as determining how many people get infected following vaccination.
Penn researchers also want to study the immune response beyond six months.
“The immune response is clearly dynamic and undergoes changes over a relatively long-time scale. So we expect that there will be continued evolution of the immune response even after six months,” Wherry said.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)


