Trenton clinics abandon long-term schedule to try to reduce wait times
Listen-

-

-

-

-

-
-
-
-

-

-
-

-

-

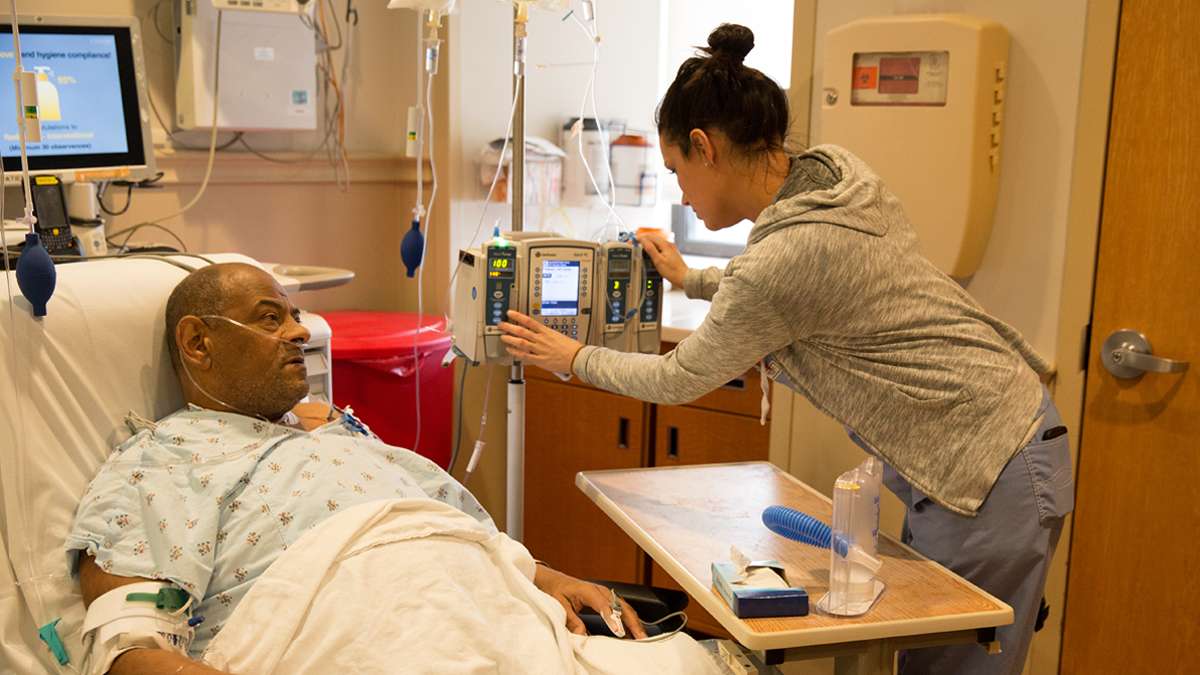
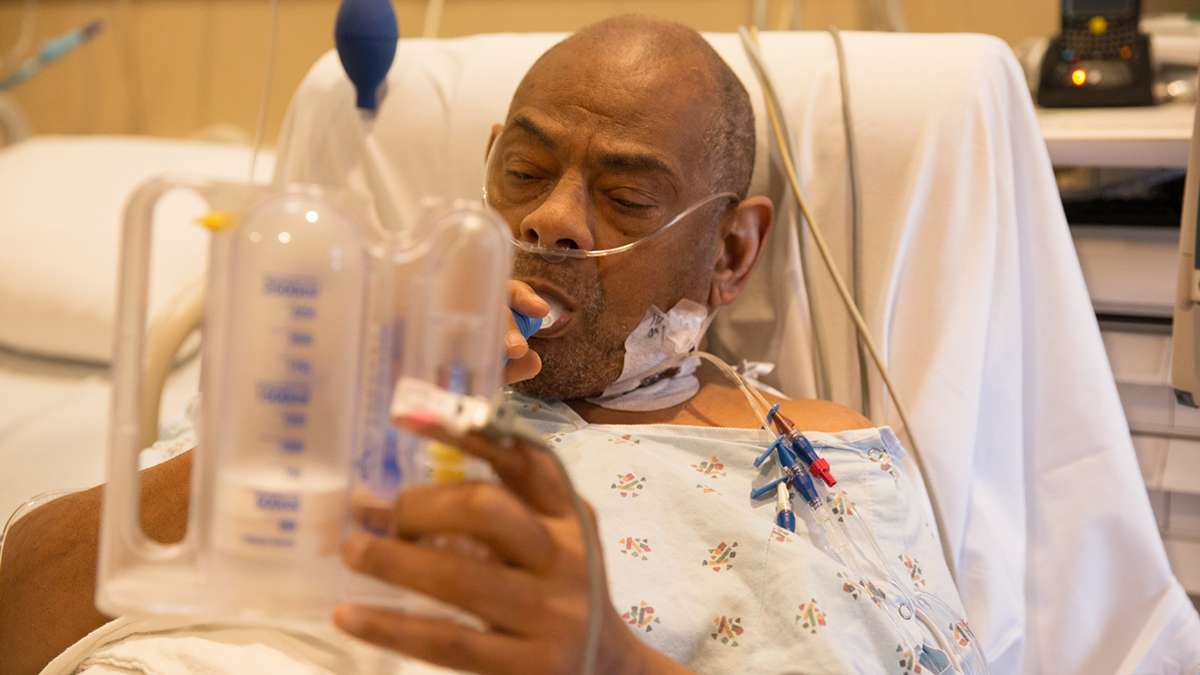
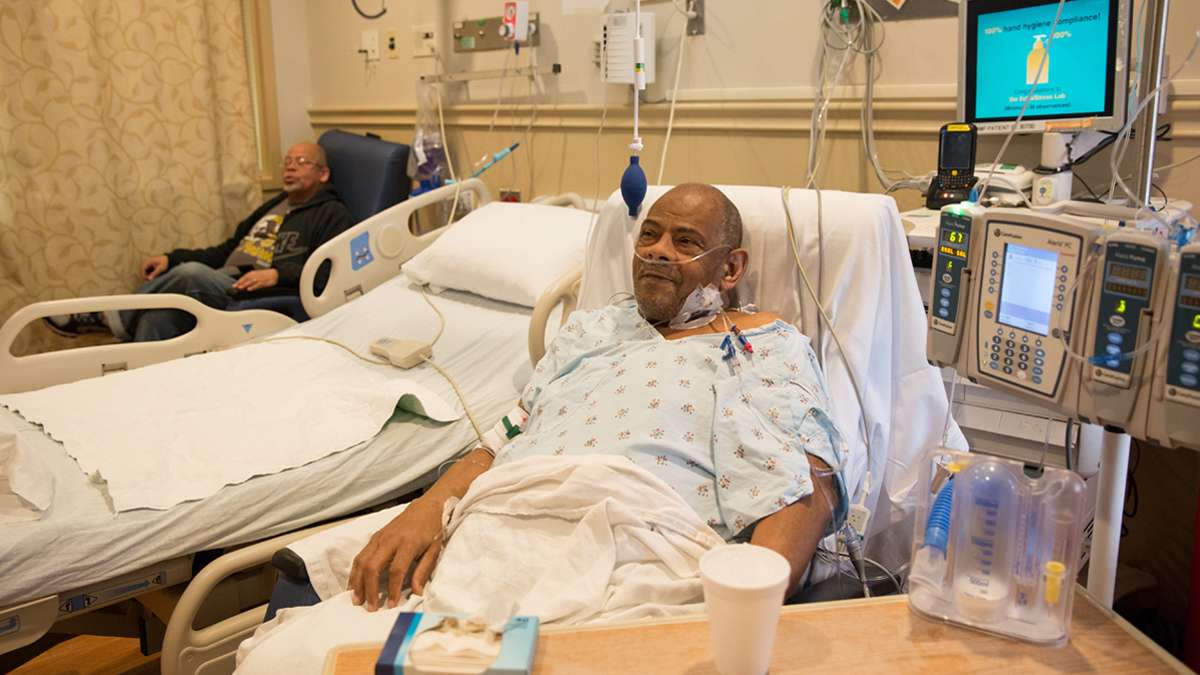
(Lindsay Lazarski/for The Pulse
-

-

-

-

-

-

-

-

The concept is called advanced access, and it encourages providers to get rid of the backlog by doing away with long-term scheduling books.
For years, residents in Trenton, N.J. typically had to wait more than a month for an appointment at the main health clinic, which stressed staff, patients and the broader health system. Then, health leaders tried something that, to them, seemed counterintuitive: they did away with long-term scheduling for the most part. The approach, known as open or advanced access, has gained a lot of traction in recent years, mainly in primary care. Now, nearly three years in, the system has been tried by many providers in Trenton, who say after some initial legwork, they’re able to see more patients at times when the patients want to be seen.
Inside the scheduling hub
Manuel Soto says the flood of calls hits like clockwork on Mondays at 8 a.m. He’s ready for it, he says, headset on and stationed at a computer cubby.
“How may I help you?” he asks, picking up a call mid-ring, as the morning rush begins. Soto swiftly punches patient information into an electronic scheduling system displayed across two screens. “Ok, I do have 1, 1:30 2:30 and 3:00 would be the latest.”
This is the part of a health clinic you may never see. And why would you? It’s the call center, where Soto and a handful of other operators, including one nurse, manage a flow of people seeking appointments at the Henry J. Austin Health Center in Trenton.
“Time goes by quick,” Soto says. “It’s pretty exciting. Busy, though.”
This call center can easily book 100 appointments in a day, according to Soto. Most, however, are for slots that same day, the next day or within a week, give or take. It’s methodical. Returning patients get matched with the same doctor.
But Soto and others say it wasn’t always this way. Up until a revamped call center and scheduling overhaul in April 2011, appointments came through a patchwork of direct patient calls to on floor nurses, Soto and others for appointment requests on a schedule that was usually booked for weeks out.
‘Frustration and stress’
Henry J. Austin’s four locations are main points of entry for health care in a city where at least a third of people live below the poverty level. The clinic alone handles some 50,000 patient visits a year, according to medical director, Dr. Kemi Alli.
Dr. Alli has been leading the charge here, and throughout all of Trenton, to reduce wait times for getting in to see a doctor. Alli started as a resident at Henry J. Austin over a decade ago. Sitting in that same office, but now as medical director, and in between pediatric patient visits, she says she loves her work, but it used to be a lot more frustrating and hectic, taking on average, 37 days for people, mainly adults, to get in for an appointment.
“The theme that you would hear was frustration or stress in the patients trying to get in and be seen, and then that snowballs and can lead to many different things,” says Alli. “It leads to higher ER visits, and if you don’t go to the ER and don’t get the services you need, then you end up in the hospital, so just the snowball effect of all the things we know we don’t want from health care.”
Alli says staff had trouble keeping up, and yet the clinic’s packed schedule included no shows 40 percent of the time.
“I thought, there has to be a better way to do this, all of this,” she recalls.
Experimenting with ‘advanced access’
Enter Mark Murray.
He’s is a consultant and a former assistant medical director at the massive health system, Kaiser Permanente, in Northern Ca. Murray is obsessed with minimizing delays and improving the flow of patient care. Alli called him for help. Murray says her concerns were “common complaints of a system that’s out of control.”
Murray preaches a concept called advanced access or open access. He says its modeled off of lean thinking and industrial engineering concepts that companies like Starbucks and Amazon rely on to reduce waiting.
So, he says, why not apply that to health care?
“The basic premise is that we want to build and design a system so that there’s no delay,” he says. “Where we understand what the capacity of that system is, what the supply of that system is. We understand correspondingly what the demand is, we balance those two, and then once they’re balanced, we put them together and then eliminate the waiting time in between the two of them.”
Getting rid of the wait
Murray challenged Dr. Alli to better understand her own clinic’s supply and demand. How many doctors work there? How many patients can each handle on his/her panel, and in turn, how many new patient appointments each week could be they take?
While it requires constant data crunching, Murray says even at places like Henry J. Austin, those answers may be more predictable than you think. For example, if there’s a constant, fixed delay of three months, then that means “you have enough capacity to keep up, but you’ve chosen a system that won’t keep up. Why do you make everyone wait three months?”
Get rid of the wait, the thinking goes. Instead, reduce that constant backlog through some additional legwork so that when those same people call, the clinic can take them that day.
Dr. Alli was on board, but convincing staff to let go of the old system wasn’t an easy sell, especially because it meant six months of working longer days and seeing additional patients to get rid of that pent up backlog.
Kimberly Allen, a longtime nurse, recalls the transition.
“One thing that really helped – we started in the morning with huddle meetings, so we had this 15 minutes where we encouraged one another,” she says.
Dr. Alli, meanwhile, reined in other area health groups, including Capitol Health and St. Francis Hospital to adopt the approach. They’d formed a health care coalition, Trenton Health Team, aimed at improving health care in the city. The effort was funded by the same group, the Nicholson Foundation, spearheading a citywide coalition in Camden.
Doing today’s work today
Primary care doctors beyond Trenton appear to be incorporating same-day scheduling into their practices. A 2012 survey of 986 practices nationwide by the American Academy of Family Physicians found that 72 percent of respondents had adopted some form of open access or same day scheduling, compared to 62 percent in 2009.
It’s been about two years since the Henry J. Austin Center threw out the old, scattered scheduling system. Today, Dr. Alli says the goal is getting patients in within two days, sometimes it’s less, sometimes more. Returning patients see the same doctor. That’s key, she says, pointing to the fact that that alone can improve a patient’s health.
The new appointment system has also cut down on those no shows because patients are getting in sooner. While Ethel McCray waits with a friend in the patient area, she explains she also made an appointment for herself, as her leg has been bothering her.
“They’re gonna see me Wednesday,” she says. “I think that’s good.”
Charles Carter first came to the clinic a few weeks ago.
“It took no time at all, no time at all,” he says.
Others say it’s still a challenge getting in to see their regular doctor. Alonya Tootle is in for a checkup after calling the week before. She says it’s hard getting through the call center during that morning rush. Slots fill fast.
“Then they say, ‘Well, we don’t have anything for this month, but you have to call by back next Monday at 8 a.m. and see if we have something,” she says. “That’s the problem.”
Dr. Alli says the system isn’t perfect, but they’re keeping tabs daily.
“I would say we’re about three quarters where I’d like us to be, where need to be, and part of that is improving the flow within the practice, I think there’s still work to be done there.”
She says making a more responsive call center and scheduling system is important, but one continuing challenge is they don’t have enough staff or space to respond to the many residents needing care in Trenton. The clinic is also losing one doctor, who’s retiring, and they’re having trouble finding a replacement. All of this, explains Dr. Alli, means the clinic doesn’t have supply to meet the overall demand, and addressing that involves a broader strategy, one that extends beyond the clinic doors.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



