How one doctor’s risky experiment paved the way for modern intensive care
Some anesthesiologists and intensive care physicians mark August 27 as Bjørn Ibsen Day — honoring the lives he saved during a polio outbreak 70 years ago.
Listen 19:54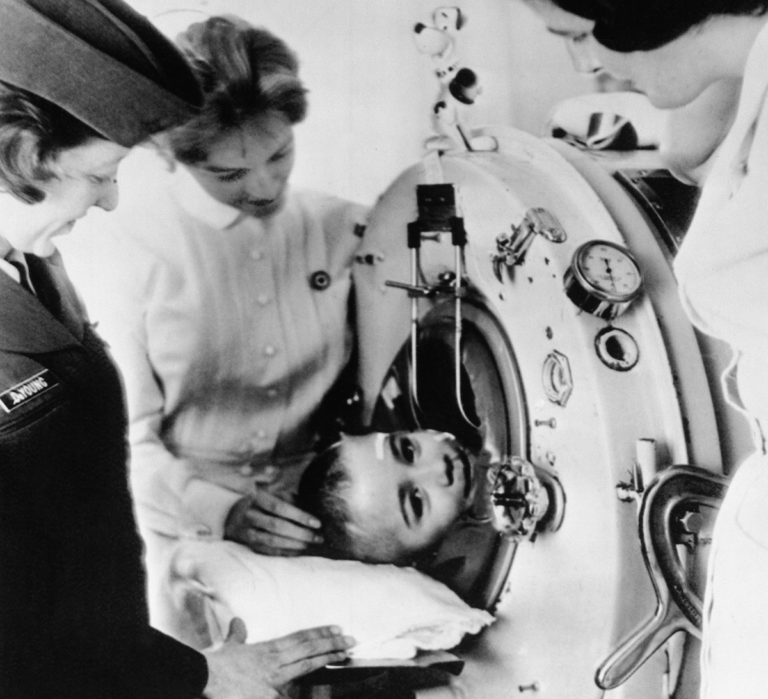
Johnny Whetzel says goodbye to his two University of Virginia Hospital nurses, Beverly Archer, center, and Peggy Moore, right, who cared for him during five months of treatment for polio in Charlottesville, Virginia (AP Photo)
This story is from The Pulse, a weekly health and science podcast.
Find it on Apple Podcasts, Spotify, or wherever you get your podcasts.
In the summer of 1952, Vivi Ebert who just 12 years old, was taken to Blegdam Hospital in Copenhagen, Denmark, where she was suffering from a severe case of polio.
People described Vivi as a sweet, vivacious girl. Polio had caused partial paralysis in both of her arms and legs. She had mucus in her lung, and she could barely swallow.
“By the time she got to the hospital, she was struggling to breathe,” said Hanna Wunsch, a critical care physician, who is currently writing a book about the polio epidemic in Denmark. “And at this point they looked at her and basically they knew there was nothing more that they could really do for her, that she was very likely to die.”
Polio was raging in many places that summer and Denmark was going through a particularly serious outbreak.
“There were a lot of cases elsewhere in the world. There were some spots in the United States that were truly terrible. Wunsch said. “But in Denmark, they had this kind of hospital that was the focus for the entire country for care of these patients. And at one point they had 50 patients a day coming into their hospital, and they were completely overwhelmed.”
They were seeing many bulbar polio cases, Wunsch said.
Polio is an infectious disease, caused by a virus, which can affect a person’s central nervous system. Any part of the body can become paralyzed, but with bulbar polio cases the virus attacks the bulbar part of the brain stem “where it’s difficult to breathe, difficult to swallow, and the mortality rate was very, very high,” Wunsch said. “They had never seen anything like it. And so, they knew if they didn’t do something, they were going to see catastrophic numbers of deaths.”
Polio was known to strike in the warmer weather, especially in summer, and it affected people of all ages. A vaccine was being developed, but it wouldn’t be widely available for another three or four years. Until then, treatment options were limited. For people with breathing problems, the main option was the iron lung, which was invented in 1928.
Subscribe to The Pulse
“It was really the first way to try to use machinery, to help support someone who was having trouble breathing,” Wunsch said. “It basically looks like a giant tin can that someone’s head sticks out of.”
The concept behind the iron lung was to apply negative pressure around a person’s chest, by sucking the air out of the large metal cylinder.
“The idea was that it would make a seal around someone’s neck, and then it would literally create a vacuum in the iron lung that would force the lungs to expand in that vacuum. And therefore, someone would be forced to take a breath in,” Wunsch said.
But there was a problem – the iron lung wasn’t very effective. Wunsch says polio still had an 80% mortality rate even with the use of the iron lung.
Iron lungs were also large, difficult to operate and very expensive. At Blegdam Hospital, they only had one iron lung in the entire hospital. Something else needed to be done. And the person to do it was a somewhat unorthodox anesthesiologist.
A risky experiment
Bjørn Ibsen was born in Denmark in 1915. He was studying medicine at the University of Copenhagen. By 1940, he decided to become a surgeon.
Louise Reisner-Senelar is an anesthesiologist from Copenhagen whose postgraduate research focused on Ibsen’s work. She says that Ibsen soon realized that it would be hard for him to rise the hierarchy of the department of surgery at the University Hospital.
“He then looked around him and saw that his career opportunities were rather dim. He could see that it would take him many, many years before he would be able to advance within the system,” she said.
Instead, he chose to focus on a field that was still relatively new in those days — anesthesiology. It wasn’t a specialty in Denmark at the time, so to learn about the discipline, he moved to the U.S., and trained and worked at Mass General Hospital in Boston.The skills that Ibsen learned there would prove invaluable in 1952. He had returned to Denmark and was working as an anesthesiologist at various hospitals, but he was asked to come in to Blegdam Hospital, to see if he could put his new skills to use with their polio patients.
“He was just a very observant man and had a lot of expertise in… looking at how people breathe and understanding what was going on with them in the operating room when they were breathing under anesthetic,” Wunsch said. “It was this training and background and this kind of unique combination of having seen what was going on in the United States and clearly being an inquisitive person, reading widely that led him to propose something that was considered quite radical.”
Ibsen was going to attempt a risky experiment.
It was something that just wasn’t being done in those days. In fact, it was the opposite of what was done. Instead of using negative pressure on a patient, like in the iron lung, he wanted to apply positive pressure, “essentially pushing air into the lungs with a bag of air and oxygen and breathing for them,” Wunsch said.
To do this, he first had to do a procedure called a tracheostomy, “putting a hole into the neck and a tube into the lungs to help someone to breathe,” Wunsch said.
This seemed like a counterintuitive way to do things. After all, we breathe naturally through negative pressure. We contract our diaphragm, expanding the space in our chest and drawing air into our lungs. Using positive pressure seemed odd or even dangerous.
“People were actually kind of afraid that if you pushed air into the lungs, that you might cause damage,” Wunsch said.
The very first patient chosen for this experimental procedure was Vivi Ebert, the young girl, who was struggling to breathe.
Ibsen prepared to do the tracheostomy. But things did not start off very well.
“One must just try to imagine being 12 years old, not able to breathe, not able to swallow. And then somebody comes and makes an incision in your throat … it was not easy, neither for the doctor nor for Vivi,” Reisner-Senelar said.
Vivi resisted. She gasped for breath and turned blue.
“She goes into what’s called bronchospasm, meaning her kind of lungs constrict, and they can’t actually ventilate her,” Wunsch said.
Ibsen had no option but to give her more anesthetic and put her under.
“Everybody kind of gets nervous that he’s not going to be successful and walks out of the room to go to lunch,” Wunsch said.
Reisner-Senelar interviewed Bjørn Ibsen as part of her research in 2006, when he was 90 years old.
“Ibsen told me that at that moment, many of his colleagues, who did not realize what was happening, they thought Vivi was about to die. They thought she had stopped struggling because she was dying. So, they left the room, and said, ‘Well, it didn’t work,’” Reisner-Senelar said.
It was at this point, with everyone out of the room, that Ibsen started putting to work all the knowledge he had gained as an anesthesiologist in the operating theater.
He knew that it would be difficult to provide treatment to a patient who was thrashing around, in clear pain and distress, so the only way he could try out his new method was to have Vivi properly sedated.
“That gave Ibsen the time to now suck out all the fluids that had collected in the lungs,” Reisner-Senelar said.
This was a very simple but crucial part of the treatment. Ibsen realized it was not only about pumping oxygen into Vivi’s lungs, but also about removing all the byproducts that had accumulated in her system, like mucus and carbon dioxide.
“Vivi was quiet, she was relaxed. Now he could start ventilating her,” Reisner-Senelar said.
Ibsen sat by Vivi’s side, with a rubber bag connected to a tube, manually blowing air into her lungs, one breath at a time. And gradually, as Vivi regained consciousness, there was a noticeable change with her.
“She goes from looking blue and gasping for breath to sort of being awake and pink and smiling,” Wunsch said.
Ibsen’s colleagues, who had left thinking there was no hope for Vivi, started to return.
“And they’re amazed. They can’t believe that she’s doing so well. And so that was enough to convince them,” Wunsch said.
From that point on, the hospital leaders believed in Ibsen and his new method. And they decided to apply it throughout the hospital. It would be cheaper and simpler and wouldn’t require any complicated machinery like the iron lung.
“This was something that every nurse or every doctor could sit down and do with very, very little training,” Reisner-Senelar said.
Within days, the mortality rate for polio patients plummeted, from as high as 90% with the iron lung to around 20%.
One-to-one care
The problem now was that the hospital had so many polio patients coming in that there weren’t enough doctors and nurses available for the new treatment. They began recruiting anyone they could find — retired nurses, medical trainees, even dental students. They would each be in charge of one patient.
“They would literally sit next to the patient and their bed, and they had a rubber bag and they had to compress this rubber bag somewhere between 20 and 30 times a minute to breathe for the patient,” Wunsch said.
They would do this in 6 to 8 hour shifts every day. It was exhausting work.
“Sometimes someone wouldn’t show up to relieve them and you couldn’t walk away. So, then you would just have to stay and keep going for another six to eight hours,” Wunsch said.
Anne Holten Jensen was just 20 years old during the polio outbreak, and in her second year of medical school. She had a friend who worked in the pediatric department of the hospital.
“She was shaken because of the work she had to do. It was like a war, she said, the ambulances were coming so often, so it was just a lot of children coming in … very ill children. They were gasping and … they were blue to look at,” Jensen said. “It was awful.”
Jensen went to the hospital one evening to see if she could help. “There were two elder students who … told me that I was very welcome to start immediately,” Jensen said. “And so, I did, and they told me in a few minutes what to do.”
Jensen was trained in a matter of minutes.
“And then I was put to [take care of] a patient who died the same evening, and it was awful,” she said.
The other students eventually came to relieve Jensen and pleaded for her to come back the following morning. After the experience of the first evening, she wasn’t sure if she could go back.
“It was rather hard. But then I came the next morning, and they asked if I would like to have a patient to ventilate who was a little boy. And I accepted. And it was much better than the evening before,” Jensen said.
The boy’s name was Paul. He was 5 years old and had paralysis in his arms. Jensen remembers him as very alert and precocious.
“It is fantastic, how children can just accept what is going on,” she said. “He was a little, clever boy.”
Jensen stayed with Paul, day in and day out, sitting next to his bed and compressing that little rubber bag between 20 and 30 times a minute. She read him stories— Winnie the Pooh was his favorite. She supported him during very painful sessions of physiotherapy, and she even broke some hospital rules with him.
“He tried to make some agreement with me,” Jensen said.
Because a patient who’d had a tracheostomy couldn’t speak, they had to communicate in other ways, like by blinking their eyes or pointing or using special boards. But Paul and Jensen discovered a way around it. They found that if they released a little pressure near the tube going into his neck, “a small amount of air could pass … and it passed through his vocal cords, and then he could speak and say something to me,” she said. “He really loved when we did this experiment, we only did it when there was no one else in the room.”
Then, after three months of sitting by Paul’s side, compressing the little bag for hours at a time, Jensen suddenly felt resistance in the balloon.
“And I said to him, ‘What are you doing, Paul? Are you trying to breathe?’ And he was smiling,” she said.
Jensen started letting Paul try to breathe by himself, not compressing the bag for some time.
“I started not giving him some air for half a minute, one minute, two minutes, three minutes. And he started to breathe. And after a short while he could breathe himself completely,” Jensen said.
Eventually Paul was able to leave the ward and move to the pediatric department, where he began his rehabilitation. Jensen lost contact with him.
She never saw Paul again, and even if she’d wanted to keep in touch with him, she was too busy by then. She was put in charge of another polio patient, a 3-month-old baby.
Soon after, though, she had to return to her studies. At the time, none of what she was doing seemed particularly out of the ordinary to her.
“We didn’t feel that we had been doing something special,” Jensen said. “I thought … now you’re going to become a doctor. So, this is your life, maybe in the future. I didn’t know better.”
Because of all the work she had put in at the hospital, Jensen failed her exams that semester. But she did pass later and became a doctor.
And even if it didn’t feel special to her at the time, her work in 1952 and the method that Bjørn Ibsen pioneered gave rise to modern Intensive Care Units.
“So, Ibsen’s idea was to … create a ward where people with respiratory insufficiency no matter for what reason, can come and be treated,” Reisner-Senelar said. “A year later … he opened the first Intensive Care in December 1953. He opened the first Intensive Care Unit of the world.”
Soon, this idea of positive pressure ventilation would gain recognition and come to be replicated around the world.
“They published widely in highly respected journals, The Lancet, the British medical journal. Within a few years, they had people visiting to see their approach,” Wunsch said. “And so, it really was influential in convincing people that this was an approach that could be used for care, not only of polio patients, but then of other patients who had respiratory failure for other causes.”
In time, the ventilation was done with mechanical ventilators like the ones we might see in a hospital today, but the principles were still the same. Ibsen, however, was not given recognition for his innovations at the time.
“He did not get the credit that he deserved,” Reisner-Senelar said.
The Director of Blegdam Hospital, Dr. Henry Lassen, told Ibsen not to forget that it was the generals who won the wars, not the soldiers.
“Lassen considered himself as the general and Ibsen as a soldier,” Reisner-Senelar said. “And when I spoke to Ibsen … he was still bitter about that. You could still hear it in his voice.”
Eventually, Ibsen did gain the recognition he deserved, at least within his medical specialty.
These days, some anesthesiologists and intensive care physicians mark August 27, the anniversary of Vivi Ebert’s procedure, as Bjørn Ibsen Day in his honor. Vivi survived her treatment and was able to live for many years afterwards.
“Unfortunately … she was one of the few patients who never recovered enough to be completely independent from the ventilator and lived the rest of her life, needing the support of a mechanical ventilator on and off,” Wunsch said.
She did, however, eventually leave the hospital. As did Paul and hundreds of other patients. Patients who may not have been so lucky if it hadn’t been for one doctor who decided to take a risk on an experimental procedure, and for countless volunteers who followed his lead.
Editor’s note: Since reporting this story Anne Holten Jensen, the medical student who volunteered at Blegdam Hospital during the polio crisis and later became an anesthesiologist, has died.
This story was adapted for web by Sarah Kerson.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.






