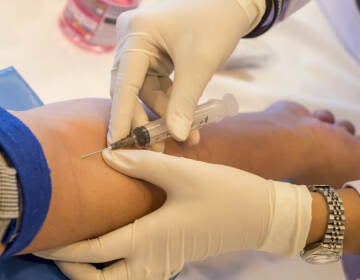
Getting on PrEP is harder than you think
In Louisiana, even an informed patient got lost in barriers and stigma while trying to get a prescription for PrEP.
Listen 10:22
In Louisiana, even informed patient Xander Adams got lost in barriers and stigma while trying to get a prescription for PrEP. (Image by Hira-Maja Dupas)
I started hearing “Ask your doctor about PrEP?” on TV and YouTube sometime in spring 2016. I was a university student having my fair share of queer fun, so PrEP was definitely a topic of conversation. But when I Googled it, a big $1,200-per-month price tag came up, which made me terrified to ask my parents about it — and they pay for my health insurance.
Then, a long list of confusing side effects filled my computer screen, from nausea to diarrhea, dizziness to depression.
Here’s the deal: I don’t like condoms — the feel, the idea, the whole thing. At the same time, I was truly lucky to receive a comprehensive sexual-health education. I couldn’t rationalize having the sex I wanted to have and not protecting myself from a threat I well knew was there.
Alone in my bedroom, just coming off the last of a series of HIV scares, I was determined: I was going to get on PrEP and stop this anxiety, this self-hatred of my sex life. So, come hell or high water, I picked up the phone, called my family doctor, and made an appointment.
I gave my pitch to the doctor:
“Hey, so I am high risk, and I know that. Um … I had 82 partners last year. I’m using but hating condoms. And uh, I know there’s another way to do this. Could we look at Truvada for PrEP?”
He pulled his laptop in front of him. Did some click-clack-clacking away. And then came the words, “This is not covered by your insurance.”
I panicked inside. I could not do this without insurance. I went home searching for another option.
Googling furiously, I found out what my doctor said wasn’t true. Not only did my insurance cover it, Gilead, the manufacturer, had a copay program that makes the pills free regardless of where you get them or if you have insurance.
So I went back to my doctor and demanded an explanation.
As he came in, I blurted out that I need PrEP. That I promised that I will show up for blood work and honestly report side effects. “I need this medication … please.”
What he said next still messes with me today:
“I will not prescribe a slut drug. I don’t want to talk about this again.”
That should never have happened. But I only know that now.
In 2016, PrEP was easily accessible in so many gay capitals across the U.S. with payment help, free lab costs, and community engagement. But San Francisco is San Francisco. Southeast Louisiana is something else.
Recently, I talked it out with a friend of mine, Austin Matthews. He’s a social worker, who specializes in patients with HIV, here in Louisiana.
He said it’s rare that clients are so forthright about saying, “’I know that I have some behavior that puts me in a higher category for this outcome. Please help me,’”
“If I could hear that from every client that I’ve ever seen as a social worker, my life would be so much easier,” Matthews said. “You gave the doctor a win.”
But that didn’t really answer my question. So I talked to someone else who helps people get on this medication every day. I shared the same story again, this time with nurse practitioner Dionne Bell.
“It’s unfortunate, but that happens a lot,” Bell said. “You know, down here in, in the South, it’s a little different. All over the country, people are evolving and trying to eliminate HIV, and this is just one of the steps in that goal. I understand discomfort with something that you don’t know. I totally get that. I do feel that he could have at least helped you to find a resource to get on PrEP.”
But he didn’t! I’m 19, trying to stay safe, staring at say-nothing billboards with no real resources on them, just “Did you know that there’s a pill that can prevent HIV?”
Yeah, I do, but that doesn’t mean I know how to get it.
“I’ve seen the commercials. I’ve seen the billboards. I’ve seen the signs, but there’s still, you know, more we need to do as far as getting access and word out there to people,” Bell said.
Soon, the New Year rolled in, and in 2017, while I was trying my best to adhere to my “sex lite” diet and get on this medication, something was changing in my backyard.
“Baton Rouge has the highest incident rate of people living with HIV, as well as people who have a confirmed AIDS diagnosis within one year of being diagnosed with HIV,” Matthews said.
From this, I know that I could not be the only person who needs PrEP. I mean I’m not some reckless maniac.
Yes, sex was my risk factor. But it’s also what ended up protecting me.
Early one morning at 3 a.m., I got a series of attractive images on Grindr, a gay hookup app, and decided to go over to this guy’s house. It was a run-of-the-mill meet-up for me. When I asked him about his HIV status, and he said, “Negative and on PrEP. Yourself?” I turned the conversation to how hard it had been for me to get a prescription.
His face lit up, he grabbed his computer and said he could help, and that PrEP was actually his job. I stood there in shock and awe. He pulled up this map I’d never seen where I could put in my zip code and find a clinic that offered PrEP specifically. The clinic-finder tool was new, and my head exploded.
Matthews wasn’t surprised I found this information during a rendezvous.
“People who are on PrEP need to be having talks with their sex partners. `Why aren’t you on PrEP?’ Because, real talk, if I’m on PrEP and I’m having sex with someone, that does not protect them from anything,” Matthews said. “But … once you know what people are into, you can have better sexual relationships.”
I agree with Matthews.
He continued, “When you know what people are into, when you know their background, when you know what’s up and what’s not, you can have a much better, happier, healthier sex life.”
I got home, plugged in my zip code, and called the nearest clinic. I found out that the soonest appointment was in four weeks, a present-day unheard-of wait time for PrEP, and that the clinic operated only one day a week, putting a huge strain on patients.
I drove down to the clinic on my one day off to do the new patient rigmarole, and I met my PrEP navigator. This was the moment!
I answered some intake questions, confirmed my insurance, and then I was shown the door.
“It will be another week before we do an HIV test, then two more weeks after that, we do another one, and then you’ll get your prescription.”
I can concede the fairness of this barrier, but all the others put me in a precarious position for longer than felt comfortable.
All in all, getting on PrEP took the better part of a year. The process was convoluted, bureaucratic, and degrading, but I made it.

At any point in that journey, if one night didn’t go as planned, if one guy persuaded me past my boundaries, if any fiber of my will to avoid HIV had faltered for one moment, I would have become positive. And this would be a very different story.
PrEP changed my life.
I am without a doubt high risk … like honey.
But more importantly, I felt more secure. I respected more people’s kinks and interests, and I could even begin to explore my own.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.