Gender reassignment surgery bans being lifted, but many barriers remain
Listen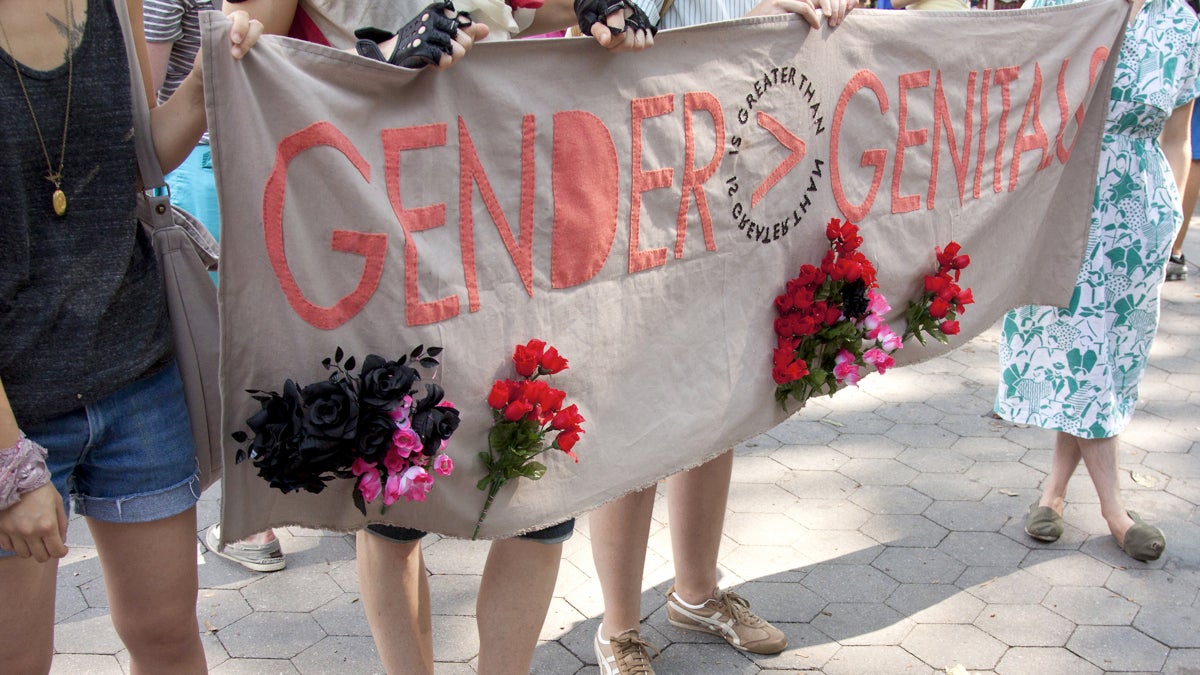
Supporters hold a banner in New York City's Washington Square Park on the 8th Annual Trans Day of Action on June 22
For those seeking gender reassignment surgeries, long stigmatized and rarely covered by insurance, many challenges remain.
Andrew DeVita, 27, was raised as a girl outside of Philadelphia, but at the beginning of college he started identifying as male. Though he knew his body didn’t match his true gender, he also felt surgery to align the two was out of his reach.
“Without insurance, I never thought that I was going to be able to afford it,” DeVita said.
The idea of insurance coverage for gender reassignment surgery seemed “unthinkable” to him back then.
“It was such a different world even five years ago,” DeVita said. “There weren’t a lot of trans people in the media, [and] they certainly weren’t on the front covers of magazines.”
DeVita resigned himself to binding his chest every day to hide his breasts.
Then, when DeVita started a new job three years ago and became eligible for benefits, he was surprised to find his new insurance covered gender reassignment services, up to a limit. It finally sunk in that his dream was going to come true last year, when DeVita had a surgery date on the calendar.
“I was on SEPTA and started tearing up and it was really embarrassing,” DeVita said.
In January, DeVita had his breasts removed and his chest reconstructed to look more masculine. He paid about $1,500 out of pocket for a surgery that would have cost him four to five times that much without insurance.
Now, he is much more at ease with his appearance.
“I don’t feel anxious, I don’t feel embarrassed, I don’t feel uncomfortable,” DeVita said. “It’s sort of like when you put on clothes that finally fit, you don’t notice all the ways that they’re uncomfortable and that they’re not for you. You just go about your life and you don’t notice a thing.”
Gender reassignment procedures historical excluded
Chest procedures like DeVita’s, as well as genital surgeries and facial contouring procedures, have historically not been covered by insurance.
Male-to-female genital surgeries cost between $20,000 and $25,000, and female-to-male procedures cost about twice that, putting them out of reach for many.
But insurance policies are slowly starting to include gender reassignment procedures.
“It varies a great deal across the country and across different types of insurance, but the overall trend is undoubtedly in the direction away from blanket exclusions and towards covering treatment for gender dysphoria based on individual medical need,” said Harper Jean Tobin, director of policy at the National Center for Transgender Equality.
Medicare, the public insurance for older Americans, lifted its decades-long ban on transgender surgeries last year, though many doctors still don’t accept the insurance because of uncertainties surrounding reimbursement policies.
Medicaid programs in six states and Washington, D.C. cover gender reassignment services. Eleven states and D.C. require private insurance plans to do the same, and more companies outside of those states are starting to do it voluntarily. The large insurer Aetna announced this year that it would phase in transgender health care coverage for most of its plans at small and medium-sized companies.
“But because of this long history of blanket exclusions in insurance, there still are additional difficulties,” Tobin said.
Other barriers to care remain
Insurance companies sometimes make it difficult for patients to prove that their procedures are “medically necessary,” the threshold that must be met for insurance to pick up the tab. And many surgeons who specialize in gender reassignment procedures don’t even take insurance.
“This area of healthcare—treating gender dysphoria—has historically been just cut out of the ordinary system of healthcare and insurance coverage,” Tobin said. “Eliminating those long-standing but completely arbitrary exclusions turns out to be a very complicated process.”
Creating a formal training program to meet future demand
Even as insurers and doctors start talking about reimbursement rates and standards of care, another key barrier remains for transgender people seeking surgery: There simply are not many doctors qualified to perform gender reassignment procedures, especially genital surgery, and waitlists can be long.
Mount Sinai Health System’s director of LGBT programs Dr. Barbara Warren remembers the day New York State announced its Medicaid program would cover transgender procedures, a policy that took effect in March.
“The day the announcement came out I got a lot, a lot, of phone calls from many folks who had Medicaid coverage who said to me, ‘Oh, at long last, I can get my surgery, where do I sign up?'” Warren said.
But Warren said there aren’t any surgeons at Mount Sinai, or anywhere else in New York City, who perform genital or “bottom” surgeries.
“I had to tell people who were very disappointed, we’re working on it, we’re working on it,” Warren said.
Mount Sinai is establishing a comprehensive transgender health care unit and working to recruit a gender reassignment surgeon, both to perform surgeries for those newly eligible for insurance coverage and to prepare for an expected increase in demand.
“We want to be able to train the next generation of healthcare providers,” Warren said, by creating a fellowship training in transgender surgery and teaching medical students.
“We really have to begin to make this part of the medical curriculum, and we have to have a program that is sustainable.”
There are currently no accredited training programs for transgender surgery procedures, so doctors interested in providing them have to learn on their own by shadowing a small cadre of pioneering practitioners. And for patients, it’s still relatively rare for a transgender person to easily glide through the insurance reimbursement process for a gender reassignment surgery like Andrew DeVita did.
It’s something the transgender community hopes continues to change.
“I wish that people understood that I wasn’t doing this because it would make me happy,” DeVita said. “It made me feel normal.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



