Crowdsourcing cures hidden in our DNA
Listen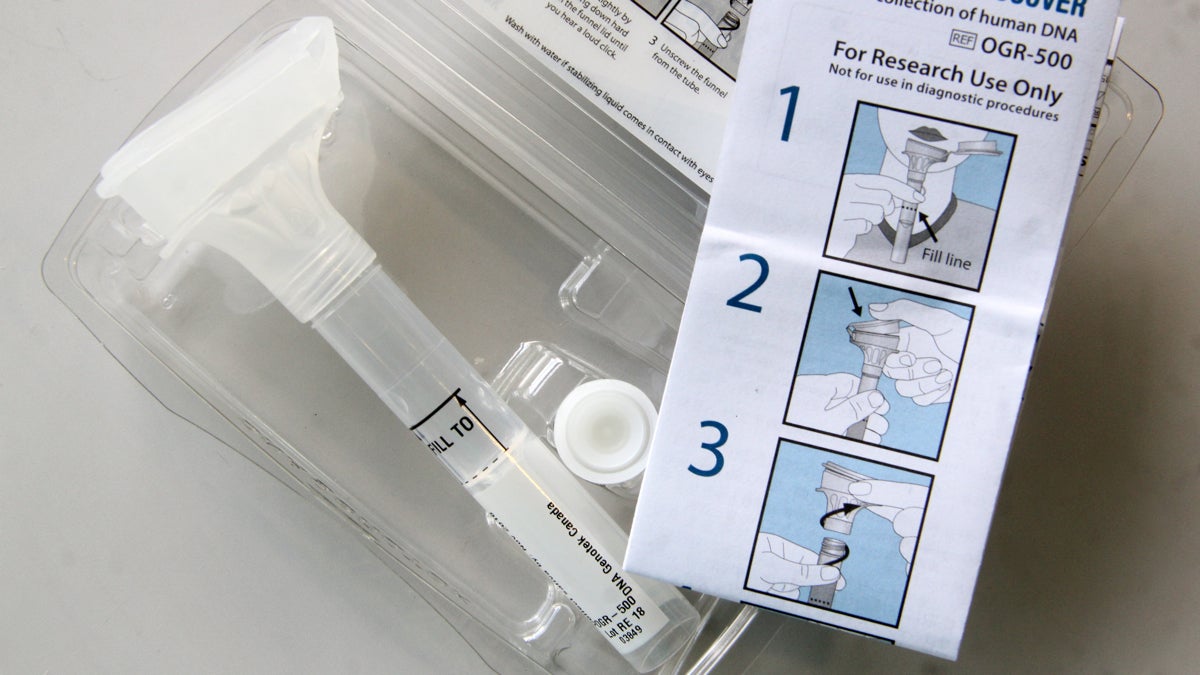
This test kit is similar
This fall, scientists are hoping you, along with a million of your closest friends, will spit in a test tube and mail it to New York.
As early as next month, geneticists hope to launch a massive, crowd-sourced genetic treasure hunt to find what they are calling “unexpected heroes”: people who carry genetic mutations that by all accounts should lead to rare inherited diseases, but who somehow remain healthy.
Dr. Stephen Friend introduced the idea, called the Resilience Project, at a TED talk in Vancouver by suggesting that scientists have been looking for new drugs in all the wrong places.
“We do a lot of studying of those who are sick,” Friend told the audience at the March event.
“But maybe, if what we’re trying to do is to develop therapies for prevention, maybe what we should be doing is studying those who don’t get sick.”
Friend, head of Sage Bionetworks in Seattle, partnered with Eric Schadt at the Icahn School of Medicine at Mount Sinai in New York to launch the project.
The goal: test the DNA of a million adults thirty and older for genetic mutations that typically lead to about 125 different inherited diseases that manifest in childhood, including sickle cell disease, cystic fibrosis, and Gaucher disease.
“Are there a very few set of individuals who are actually walking around with the risk that normally would cause a disease, but something in them, something hidden in them, is actually protective?” Schadt asked.
Schadt and Friend’s plan is to find out what within an individual’s genes or history has protected him or her from disease, and translate that knowledge into new treatments or therapies.
The duo published a proof-of-concept article in the journal Science in May, and are hiring staff and developing digital consenting protocols with an aim of collecting saliva samples beginning this fall.
Searching for a needle in a haystack
“We know that maybe 1 in every 25,000 or 50,000 adults is walking around who carries these gene changes but they’re healthy,” said Elissa Levin, head of genomics and health innovation at Mount Sinai and head of operations for the Resilience Project. The team arrived at these numbers after combing through de-identified DNA samples from medical institutions and genetic testing companies like 23andMe.
To find mutations in a new cohort of consenting volunteers, the team will look at nearly 700 different points on the genome where disease-causing mutations are known to occur.
By sequencing those specific portions of the DNA double-helix, they will look for missing or misplaced nucleotides, represented by the letters A, C, T, and G, which typically cause mutations that lead to cystic fibrosis, sickle cell disease, and other rare Mendelian disorders.
Because healthy carriers of deadly mutations are thought to be so rare, Levin’s team is expecting to find only about 50 of them among the million people they test.
This kind of genetic needle-in-a-haystack hunt has only recently become possible. In about the last decade, advances in DNA sequencing and supercomputing have allowed scientists to comb through genetic information relatively quickly and easily.
“The original human genome project… took over a decade to implement and billions of dollars,” said Levin’s colleague Bobby Sebra, director of technology development at the Ican Institute at Mt. Sinai. “Whereas today, for reference, you can basically sequence an entire genome for thousands of dollars in a matter of weeks.”
The Resilience Project is looking at less than one percent of the entire genome for each of its subjects, so the analysis will be completed much more quickly.
Next-generation sequencing makes it possible
At the Mount Sinai sequencing lab, Sebra pointed out two sequencing machines his team used to screen pilot samples for the Resilience Project, collected at the TED conference in March.
The machines, which both look like crosses between a microwave and dishwasher, can sequence the relevant DNA from 12 different samples in about two hours.
That’s compared, Sebra said, to about a month of sequencing around the clock that it would have taken with older, much more manual methods employed in the 1990s.
Given these technological advances, scientists say the sequencing will be the easy part of this project.
“I think the hardest part is going to be, once you find those people, figuring out why is it that they didn’t develop the disease they should have developed based on the mutation they have,” said Dr. Dan Rader, chair of genetics at the University of Pennsylvania, who is unaffiliated with the project.
“That’s where the real creativity’s going to come in,” Rader said. “There’s going to be a lot of work to try to figure out, looking at other genes and other aspects of those individuals, why are they so healthy when their DNA says that they shouldn’t be.”
If the Resilience Project team finds someone with a mutation, they will ask for consent for a battery of further testing, looking at the rest of the volunteer’s genome and medical history to try to ferret out exactly what is protecting the “unexpected hero” from what should be a genetic time-bomb.
Whatever is protecting that patient could be used to develop a treatment or therapy for those who do get sick.
Rader gives an example of how that has worked in the past, with an individual who appeared to be resistant to developing HIV, despite being exposed.
The patient did not have a specific receptor, the CCR5, that is required for the HIV virus to get into cells.
“That (single) example, which was published in the New England Journal and widely disseminated, I think is a great example of how just one person told us the importance of CCR5 in terms of HIV infection, and the concept that CCR5 could be a target for actually targeting therapies,” Rader said.
Rader said the scientific community is largely behind the project.
“It’s a bit of a moonshot, we don’t know what they’re going to find, but I think the chance they’re going to find something interesting is pretty high,” Rader said.
More projects of this kind to come
Mount Sinai is currently retro-fitting a 19,000-square foot DNA sequencing lab in Connecticut to handle Resilience Project samples when they start arriving this fall.
Elissa Levin said the new facility is designed with more of these large, genetic treasure-hunts in mind once the current project is used as a proof of concept.
“We’re looking to expand out these databases to look at common diseases like cardiovascular disease, diabetes, Alzheimer’s, schizophrenia,” Levin said, “and applying these models where we know that we’re going to have many more people that come up as potential unexpected heroes.”
Screening a million samples is expected to take at least three years. Mount Sinai is funding the initial stage, and looking to private foundations and institutional partners for further support.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



