A pill to prevent HIV opens conversations about sex, intimacy, fear
Listen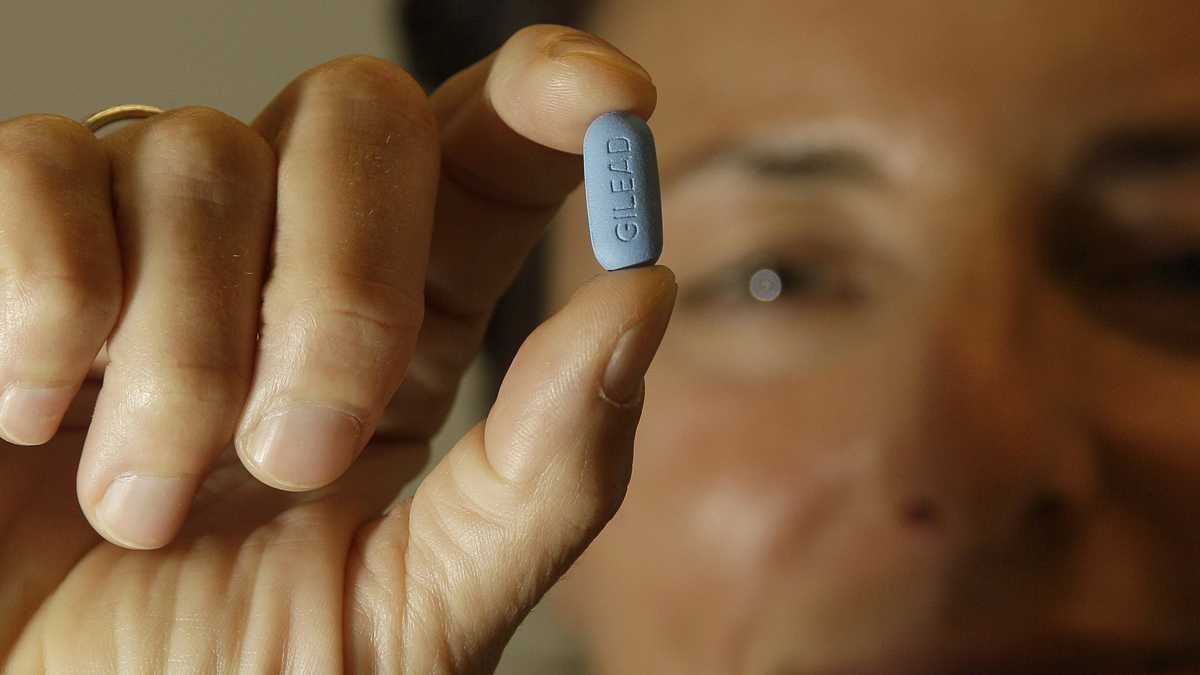
Dr. Lisa Sterman holds up a Truvada pill at her office in San Francisco. The pill
HIV doctor weighs PrEP therapy…for himself.
What if there were a pill that was extremely effective at protecting a person from contracting HIV?
Well, that’s not a hypothetical.
Some liken Pre-Exposure Prophylaxis therapy — commonly referred to as PrEP (pronounced “prep”) — to birth control for HIV.
It’s a once-a-day pill—the combination HIV drug, Truvada—and studies have found if taken consistently, it can lower one’s relative risk of getting HIV by more than 90 percent.
“It just helps me be more secure in knowing I am protected,” explains 23-year-old Christopher Dash of Philadelphia, who’s been taking PrEP for almost two years through a program at Philadelphia FIGHT. “It’s been going great.”
The Food and Drug Administration approved PrEP in 2012. In May of 2014, the Centers for Disease Control and Prevention issued guidelines, recommending those who are at high risk for contracting HIV take it.
For many in the HIV field, including Dr. John Vaz, an infectious disease doctor and HIV director with Chase Brexton Health Services in Baltimore, PrEP represents a major, potentially game-changing, tool in HIV prevention.
“Some of the modeling that the WHO [World Health Organization] did shows that, in the next 10 years, if PrEP was rolled out to men who have sex with men, it could avert one million infections. That’s a huge number,” says Dr. Vaz.
But last winter, he debated whether to take the drug himself.
“You know, we’re also human even if we are physicians,” he says.
From movies, to moving in together, to…
They met on Grindr.
“Really, it was fairly innocuous,” says Vaz, laughing.
It was a little over a year ago. Vaz was at home in D.C. watching a french movie with a friend.
“And he was somewhere else in D.C. watching a movie on a Shabbat dinner night with his friends,” he recalls.
They talked movies for a bit, exchanged phone numbers, and then met for coffee the next day.
“We really enjoyed spending time with each other, and a coffee date became a sort of hang out date, and then lets get dinner, and then let’s go back to yours, and you know…”
The two moved in together a few months later. “It was fantastic,” Vaz recalls.
Sort of. It was comfortable. But something was … missing.
“Suffice to say, life is too short for bad sex,” says Vaz.
The two talked it over and decided to open up their relationship. They were still committed to each other, but agreed it was okay to have other sexual partners. Vaz was totally on board, but he did worry about one thing: HIV.
With their new dynamics, he worried about the risks, even though he always uses condoms.
“You just never know what will happen in that moment of passion,” he says. “The barrier methods of prevention might fail.”
This brought him face to face with that new option, PrEP.
Meanwhile in his practice
Vaz actually knows a thing or two about PrEP. He was in Philadelphia last week presenting on it at the Trans-Health conference, and he has several dozen patients who take it.
So how, exactly, does it work? While HIV is a powerful virus, Vaz explains, it needs to take control of cells to proliferate.
“They cannot do anything by themselves,” he says. “They need to get into a cell and hijack a cell’s machinery to survive.”
But Truvada, if it’s already in a person’s body at the right levels, basically stops the HIV virus from taking over that cell. And so the virus dies.
Reported side effects can include some nausea at first. Vaz says the main thing is monitoring a person’s kidneys, because that’s how the drug is secreted. Patients must come in for a checkup and refill every three months.
For Vaz, last year’s CDC guidelines signified greater access to PrEP for many patients. That’s because it meant insurance would start covering it.
“For me personally, I went ‘Yes!'” says Vaz.
The drug costs about $1200 a month, though, in many cases, the drug company Gilead, which makes Truvada, offers direct patient discounts. Philadelphia is one of four cities, as part of a national project, that’s offering PrEP through its public clinics.
PrEP has stirred some controversy. What if it leads to riskier behavior and, in turn, higher sexually transmitted infection rates? That hasn’t shown to be the case. But why would a seemingly healthy person take a pill for something they don’t have? And what if people miss doses? How protected are they?
For many patients and providers, PrEP is still a really new concept.
But in his own practice, Vaz says the real success of PrEP has not been about him merely writing a prescription.
“It also allows for us then to have this forum of someone’s life, which, you know health is about so much more than giving people pills,” he says.
He has seen it open up conversations about stigma, about HIV (whatever one’s status). He has seen it create spaces to address sexuality, fear and intimacy.
“It really just starts people to think about their sexual health and make good decisions ‘in the quieter moments of their lives,'” he says, borrowing something he read from Robert Grant. “That hopefully will pervade those heat of the moment, lustful, passionate moments.”
Of love and friendship
Vaz was “fifty-fifty” about taking PrEP himself a few months back.
He consulted his own primary care provider, “a feisty nurse practitioner.” In the end, after consulting with her and further assessing his situation, he decided it wasn’t right for him.
At least at that time.
“But trust me, if I felt like I needed it, I would have said, “No! I’m going on it.”
Part of his reasoning was his open relationship, it didn’t pan out.
“I think there’s no prescribed way to do things. And we really did enjoy the year we had together, just shaking together,” he says. “And we are the best of friends. And I love him dearly. And I always will.”
But, Vaz realized, they weren’t in love.
Vaz is in a new, exclusive relationship now, and while he’s not taking PrEP, he says his former partner and now dear friend, is. That gives him a lot of peace of mind because Vaz thinks weighing those decisions and in turn, taking care of one’s health, is as much about loving oneself as it is someone else.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



