A cardiologist wanted to prevent long COVID. He turned to meditation.
A recent review of research suggests meditation may be effective for some in treating long COVID and other post-viral conditions.
Listen 10:53
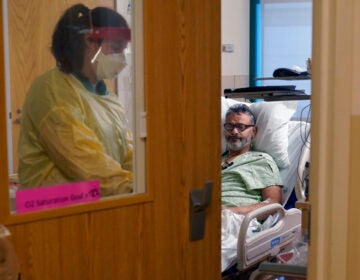
When Boon Lim tested positive for COVID after a ski trip in the French Alps, he turned to meditation to prevent long COVID. (Courtesy of Boon Lim)
This story is from The Pulse, a weekly health and science podcast.
Find it on Apple Podcasts, Spotify, or wherever you get your podcasts.
In March of 2022, Boon Lim was nearly 6,000 feet above sea level on a ski trip in the French Alps when he developed a cough.
“A very nasty cough that really hurt,” Lim said. “I thought I had fractured a rib. That’s how painful it was.”
Lim, a cardiologist from London, barely toughed it out on the slopes the first day. Later that evening, he couldn’t keep up with his wife at the supermarket.
Shortly afterward, he tested positive for COVID-19.
“I said, ‘What COVID? Shmovid. I’m a fit and healthy guy. I should be out on the slopes with the kids in three days time.’ By three days, I couldn’t breathe,” Lim said.
Lim bought a pulse oximeter to monitor his symptoms and discovered his blood oxygen level had fallen to 82 percent – dangerously low. He was rushed to a medical center by ambulance where a CT scan revealed his lungs were severely inflamed.
The images looked remarkably similar to the scans of his patients back in London who had long COVID.
“I said, ‘Okay, I’m a sitting duck for a long COVID,’” said Lim. “I was sleeping 14 hours a day and feeling breathless for the rest of the time of the day and feeling extremely exhausted. And I thought, ‘Gosh! If this is how long COVID feels, if this is how I’m going to feel in 12 weeks, in 24 weeks, I’m in trouble and I can’t work.’”
Once Lim returned to London, he decided to take a radical step.
“I recognized that what I needed to do was to turn off my mobile phone, just have an auto reply, and I said to my secretaries, ‘just no response from me.’” Lim said.
He put his practice on hold and dedicated the foreseeable future to his recovery.
“I got into a very deep practice of meditation, really deep. And I was able to practice this for about 3 hours a day where just to focus on diaphragm breathing and a focus on positive healing from my mindset,” Lim said.
But could something as simple as sitting and thinking positive thoughts and meditation really fight off long COVID? Could it stop these symptoms from becoming chronic?
Subscribe to The Pulse
The hypothesis stemmed back years earlier to Lim’s PhD research at Imperial College London on the autonomic nervous system.
“In a nutshell, it’s that bit of the brain which is quite primitive,” Lim said.
The autonomic nervous system is responsible for the body’s involuntary, but absolutely crucial actions, such as the heartbeat, breathing, digestion, reproductive functions, sweating, the immune response, and more.
While these functions remain almost entirely beyond conscious control, Lim knew under the right circumstances it is possible to “rile up” some of these functions.
For example, an adult’s heart rate can rise more than 20 beats per minute when simply pressed to answer a surprise middle school math question in front of an audience, according to Lim.
But is it possible to provoke an opposite response – one that calms rather than excites? And could that response impact the devastating effects of long COVID which seems to be related to inflammation and immune system dysregulation?
Lim wanted to find out. He saw long COVID patients struggle to find solutions to seemingly unrelated problems, as various specialists attempted to alleviate the individual symptoms of long COVID that fell within their realm of expertise.
Long COVID treatment plans often reminded Lim of the famous Indian parable about a group of blind men who each try to describe an elephant by touch.
“The blind man that approaches its tail and pulls a tail says, ‘The elephant is just a rope.’ And the one that approaches his tusk says, ‘The elephant is like a spear.’ And the one that approaches his side [says], ‘it’s just like a wall,’” Lim said.
Because each specialist faced a unique manifestation of long COVID, his patient’s symptoms were often treated as if they were isolated from the larger diagnosis.
Lim wondered whether the virus caused the autonomic nervous system, the control center for the body’s immune response, in these patients to go awry, causing these mysterious symptoms. If so, perhaps reversing this dysregulation would provide a lasting solution.
“I think if you really want to get a holistic picture of long COVID, you need to see the elephant in its full glory, with all the multi facets and components of the elephant, and try and develop, if you can, a unifying diagnosis to explain why all these things occur,” Lim said.
In fact, Lim had already heard encouraging anecdotes from several of his patients, who told him about a promising long COVID recovery program centered around yoga and meditation.
The program was designed by Suzy Bolt after she contracted COVID-19 early on in the pandemic.
“I just felt like I had been poisoned. Like, seriously poisoned,” Bolt said.
Weeks passed following her infection, but her condition stayed the same. She didn’t suffer blood clots or lung damage, but she had a crippling sensation that something inside her body was off – like she was stuck in fight or flight mode all the time.
“I [felt] like everything has got 6000 volts of adrenaline pumping through me,” Bolt said.
Bolt desired to reset her body’s programming like a computer. Maybe, she thought, if she shut everything down and rebooted herself back up again, she could jolt her system out of this terrible funk.
“And it was in that moment that I went, ‘Okay, so I know about the autonomic nervous system,’” Bolt said.
She believed meditation and mindfulness could act as a backdoor into this innermost program — allowing one’s conscious thoughts to affect the body’s most basic processes.
“My hunch is that calming ourselves down … just literally calming the nervous system, slowing down the breath, working with the mind, the body, just to kind of come home,” said Bolt. “I felt so abstracted from myself. I was so ill. I felt like my body was a kind of battle zone. It was like a wasteland and I needed to do that.”
It was just a hunch, but Bolt was determined to test her theory and share her findings with others along the way as a possible supplement to the treatments provided by specialists.
She also believed community and support were key to her reboot. So she started a Facebook group.
“And it grew and then it grew and then it grew,” Bolt said.
Bolt’s program was a hit and soon evolved into a business. She started offering classes day and night, live and on-demand, taught by herself and instructors all over the globe.
“We have had thousands and thousands of people come through the program now,” Bolt said.
The classes range from 30 to 90 minutes, varying from mindfulness meditation and breathing exercises to pilates. Bolt likes to keep things open and experimental.
Now, science is backing up some elements of this approach. A recent review of research suggests that meditation could have measurable effects on outcomes for long COVID patients potentially due to its ability to limit the presence of pro-inflammatory proteins and encourage the production of anti-inflammatory proteins.
“The research does suggest that post-viral illnesses can be in some ways improved in terms of the conditions of the person by basically doing meditation,” said Leonard Jason, a psychologist at DePaul University who co-authored the review.
“I would say that there’s pretty good research. Why it happens is something we’re still trying to understand. We have some good theories and we have some good data, but this is really for the future and this is where I think medicine and health care will be moving as people learn to basically self-regulate, to improve, and through their own efforts make an important change in their lives.”
Boon Lim listened to his patient’s stories about Suzy Bolt’s yoga and meditation protocol. And it all made a lot of sense to him. He decided to go all in on this idea in the weeks after his COVID-19 infection, as his symptoms lingered.
“I let go of work, I let go of my research commitments,” said Lim. “I let go of all these responsibilities and I fully trusted my the team who support me. So my medical secretaries, I just said, ‘Look after me because I can’t do this now.’”
In addition to traditional treatments, Boon decided to completely eliminate the stress of everyday life and place his entire conscious focus on recovery through meditation and deep relaxation.
He knew this wasn’t feasible for many people with long COVID as most can’t afford to completely shut life down, but he credits the opportunity to do so with keeping the disorder at bay.
“I was able to drop and go to a moment of self-connection, self-recovery, and really focus on the things that I should be focusing on when you’re recovering, which is self. And in being able to give myself 3 to 4 hours a day to meditate and to breathe, I was able to, after six weeks, come back to full working health and within three months back to normal completely,” Lim said.
He is now back to work and life – feeling even better than he did before he got COVID-19, he said.
Editor’s note: This story has been updated to clarify the review of research findings on meditation as a treatment for long COVID.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.