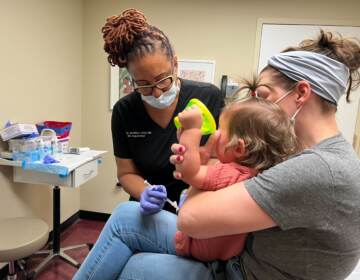
‘Save lives, go home, and do it again the next day’: Working in Wilmington Hospital’s COVID-19 unit
Coronavirus cases are dropping, but Delaware hospitals are still operating under crisis standards of care. “COVID is still deadly,” one nurse manager stressed.
Listen 2:05
Respiratory therapist Raynell Peacock, wearing a breathing apparatus, prepares to enter a COVID-19 patient's room. (Cris Barrish/WHYY)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
All the intensive care beds at Wilmington Hospital were occupied, leaving nurse manager Justin Bartels out of solutions for one of his unit’s COVID-19 patients.
Bartels had a special affinity for the man, who was in his 60s, had experienced homelessness before he became infected, and was not vaccinated.
“He had been here for a while and was getting sicker and sicker,” Bartels told WHYY News about the harrowing night three weeks ago. “But it was when we were at the height of this surge and we had no beds upstairs to put him in.”
Bartels said the patient was very sick, explaining “we just could not get him up to the higher level of care like the ICU that he needed. And we were doing the best we could and trying to take care of him.”

Through the night, the man deteriorated and he “coded and died,” Bartels recalled, his voice cracking.
The man’s COVID-related death was by no means the first in Bartels’ unit since the pandemic first hit Delaware 23 months ago
But that night Bartels left the hospital in tears.
“I’ve been here 11 years,” he said. “And I have not gone home crying in a long time. He was homeless and had nobody. And it was very difficult.”
‘Hopefully the light’s at the end of the tunnel’
Bartels and a few other staffers of Wilmington Hospital spoke with WHYY News during a reporter’s visit to the hospital, which on Jan. 10 joined most others in Delaware by retreating to a “crisis” level of care after being overrun with COVID-19 patients during the worst surge of the pandemic.
The hospitals remain packed and are still in “crisis” mode, though the number of COVID-19 patients statewide has plummeted from 759 to 411 in less than three weeks — a 46% drop that reflects the diminishing impact of the highly transmissible but less deadly omicron variant. Delaware National Guard members have been deployed to escort patients and assist with other clerical duties so caregivers can work with patients.
Bartels and other employees said they are weary and exhausted, both physically and emotionally, but are holding on even as they implore the public to get vaccinated, wear the masks that once again became mandatory in indoor settings on Jan. 11, and physically distance to stop the rampant community spread.
Bartels emerged from his office into a quiet hallway of the fourth floor COVID-19 unit, where 22 patients with the virus were being treated.
At one door stood Raynell Peacock, a respiratory therapist. Peacock was wearing a Powered Air Purifying Respirator, protective headgear that resembles an ice hockey helmet, and a breathing tube that carries air that is purified in a unit contained in his backpack.
Peacock stopped for a few moments before going into the patient’s room.
“It’s strenuous, I guess a little bit nerve-wracking at times,” he said of the daily grind. “Mostly it’s tiring. But you just got to do what you got to do every day. You know, help people out, save lives, go home and do it again the next day.”
Peacock said he’s treated too many patients who have died.
“It’s part of the job, honestly. You really just learn how to cope with it. Hopefully the light’s at the end of the tunnel, hopefully soon.” Peacock said.
To date, 2,531 Delawareans have died of coronavirus-related causes — 197 people in the last month alone.
On Jan. 12, the seven-day average daily case rate was 3,381 — four times the previous peak a year earlier. The current daily rate is 972, also above last year’s high of 850.
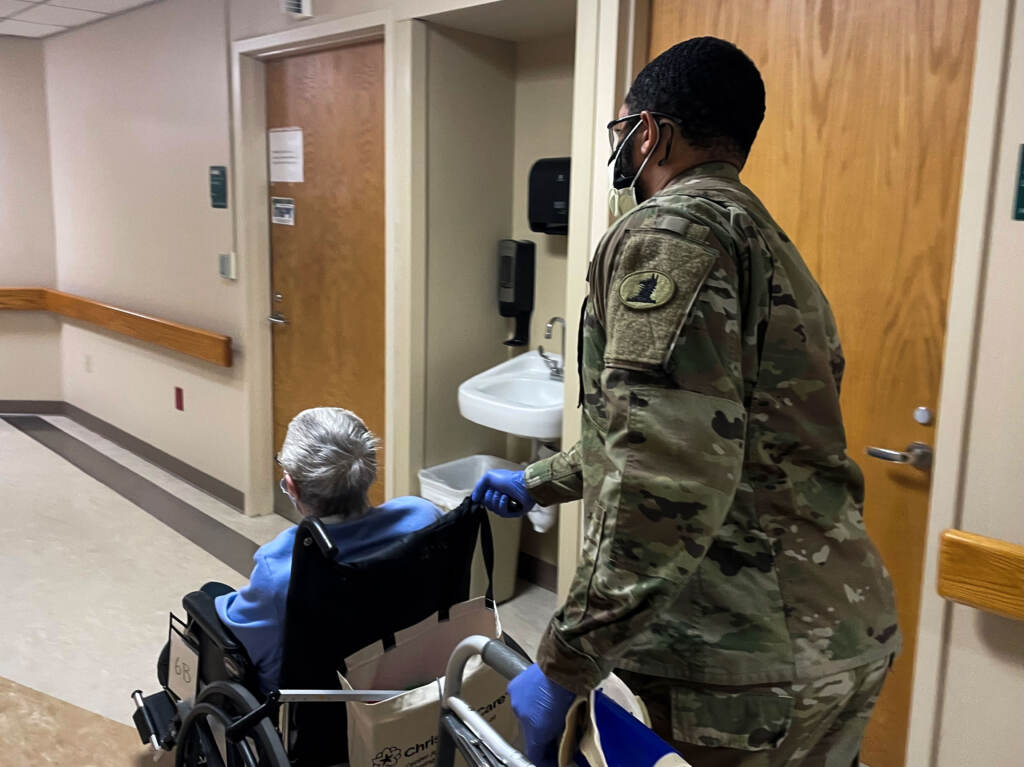
National Guard assists in overwhelmed units
Elsewhere in the hospital, the business of treating patients continues.
Jamie Ayala is a nurse manager in the rehabilitation unit for patients working to regain independence while recovering from strokes, injuries from accidents, and other maladies.
She said the post-Thanksgiving escalation has taken a toll even on the rehab unit, which has had to take other patients as beds in other units have been overwhelmed by people needing inpatient treatment for COVID-19. The unit has persevered even as nurses and other staffers have come down with the virus or have had to quarantine after possible exposure.
“The past two months have certainly been a challenge for us here in health care,” Ayala said. “We have just been having ups and downs, ebbs and flows. Our staff have been great, getting their vaccinations and showing up for patient care every day. But they are getting tired and fatigued, certainly.”
Ayala spoke as a Guardsman, wearing military fatigues, wheeled a patient into the unit. “Having them here is very surreal, but we’re very grateful,” Ayala said. “They do small tasks, but these small tasks add up to hours and minutes so the nurses and the clinician [are] able to take care of the patients. And so having them here allows us to focus back on patient care, and it actually has a ripple effect throughout the system.”

She said that having the National Guard members “taking patients back and forth to therapy, being on time, allows the therapist to start on time, allows the therapists to focus on medications, wound treatments, patient education. And so it also frees up escorts in the rest of the system to discharge patients or to take patients to tests on time. So just having a few of them here has been a tremendous help.”
Specialist Marcus McCray of the National Guard had escorted Ellen Schwartz, who is recovering from a stroke, into the rehab unit.
McCray, an aircraft mechanic in his civilian life, said he enjoys helping the nursing staff.
“I’m just doing my part,’’ he said.“ I love serving the community and just helping out, especially the elderly. I lost my grandmother a couple of years ago. I get pleasure out of it.”
Bartels said the National Guard members have been a godsend.
“They are able to come in and help take some of those tasks that nurses are struggling to get done. The stocking, the answering the call bells, taking refreshments, and things like that into the patients, or at least the doors. Nurses are used to juggling things but not having to juggle so many and someone there to catch those balls before they hit the ground has been a huge help.’
While COVID-19 cases are dropping after January’s astronomical numbers, Ayala is urging the public to care about caregivers and the situation in hospitals.
“The best way honestly to help us is to wear your mask, social distance, get vaccinated, and get boosted. And that keeps you out of the hospital,” Ayala said. “Take the precautions to stop the spread.”
Bartels said most of his COVID-19 patients have not been vaccinated. In recent weeks, about 60% of patients statewide have not been fully vaccinated, and 90% have not been boosted.
“COVID is still deadly,” he stressed. “It is still deadly for those who are not vaccinated or have underlying health conditions, and those are the ones that you need to protect. You may have COVID and be just fine. But there are other people who may not survive.”
“You owe it to your fellow human being to be kind and to take care of humanity that way,” Bartels added. “And you may be fine, but the hospital cannot keep taking care of this huge surge of people who need our services.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)