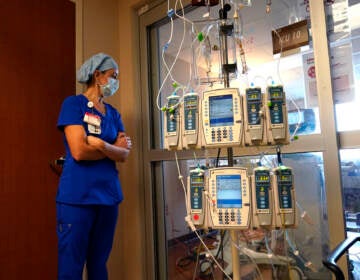
Were hospitals unprepared for the pandemic? How are they planning for a 2nd wave?
The current pandemic exposed some deep-seated issues with disaster planning, and hospitals are working on those before a second wave of COVID cases arrives.
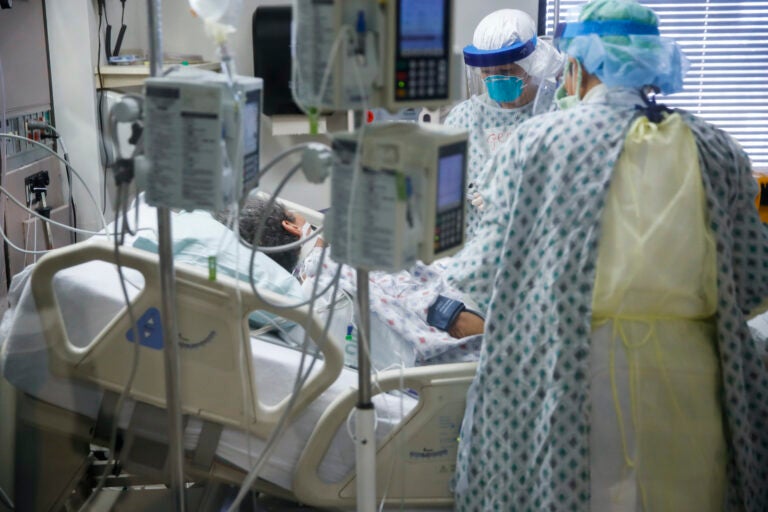
Intensive care unit staff members care for a COVID-19 patient, Monday, April 20, 2020, at St. Joseph's Hospital in Yonkers, N.Y. (John Minchillo/AP Photo)
Updated 10:05 a.m.
Are you on the front lines of the coronavirus? Help us report on the pandemic.
Many scientists say COVID-19 could return with a second wave of infections, which means hospitals have a few months to learn from the first outbreak to prepare for a second one.
The first wave of COVID-19 infections in March seemed to catch hospitals unprepared. Medical staff had to reuse and save protective masks. Hospitals worried about a shortage of ventilators, and drugs. Thousands of health care workers got sick.
But hospitals have disaster plans. The Centers for Medicare and Medicaid require that hospitals that are part of their programs have plans for disasters. The Centers for Disease Control and Prevention, and the American College of Emergency Physicians have guidelines for how hospitals can prepare for disasters.
So what happened with this pandemic, and how can hospitals prepare for a second wave of COVID cases, or other pandemics?
One issue is that emergency planners decide what to plan for by looking at what is likely to happen, which could mean less time and money on catastrophic but rare events, said Rick Murray, director of the EMS disaster preparedness department at the American College of Emergency Physicians, who has been doing disaster planning for more than 40 years.
“Could a 747 crash into our hospital? Well that could happen but it’s not very likely,” he said. “You think, ‘OK we’re in a tornado-prone area, so that’s going to be a high emphasis for disaster training, or we’re in an earthquake zone, or we’re coastal’ … for the most part you want to train and spend … your resources on what is more likely to happen, than the what ifs.”
He said that a pandemic on this scale was a what-if for many hospitals, and even for the CDC. Eric Toner, a senior scholar at the Johns Hopkins Center for Health Security, said that meant the people who warned this could happen early on were not taken seriously before the wave of COVID-19 cases in the U.S. in March.
“While the emergency managers and some of the physicians who take a lot of interest in disaster preparedness were quite alarmed about what was being seen coming out of China and Italy, they were reporting to us that they could not get traction with their hospital leadership,” Toner said. “For the most part hospitals have never taken seriously the possibility that they would need to prepare on something the scale of a 1918 [flu] pandemic. Even the CDC has always thought that that was an extremely unlikely scenario.”
That’s why Toner and his colleagues wrote an article in the Annals of Internal Medicine in early March detailing how hospitals should prepare for COVID-19.
He said that for the most part, hospitals worked hard to cancel elective surgeries, find extra space, get ventilators, and other measures to prepare for a surge of COVID infections.
Toner added that now is the time to think about a second wave of infections, which he and other experts said is almost certain. One thing he said hospitals have to plan for is how to accommodate COVID patients while treating the patients who have had their care deferred for months.
“These elective procedures for cancer operations for heart operations, they weren’t faceless, so those have to resume, and so the question is how can that be done safely,” Toner said.
Hospitals across Pennsylvania have started bringing patients back for elective procedures and in-person care, with extra precautions to follow social distancing guidelines. Scott Mickalonis, regional manager for emergency preparedness at the Hospital and Healthsystem Association of Pennsylvania said many hospitals effectively prepared for a surge of COVID cases in the first wave, and are now reviewing their response, so they have not yet come up with specific improvements when it comes to planning ahead.
But the pandemic has also made other, more deep-seated problems clear. José Torradas, an emergency care doctor based in Bucks County and spokesperson for the American College of Emergency Physicians, said the lack of resources for supplies like masks and gloves, and the lack of planning for disasters, comes partly from the model of treating health care like a business, where pandemic planning is an inefficiency that hurts the bottom line instead of an obligation to the communities they serve.
“I can tell you that we were already short on the amount of [personal protective equipment] that we needed literally in week one,” Torradas said. “Clearly whatever plans … that is written on paper were vastly and grossly insufficient from what is needed in reality. For business folks who are seeing it in a quarterly earnings set up, they’re not incentivized to plan for something that may only happen once per 20, 30, 50 years.”
“This is where business first and patient first models diverge,” Torradas added.
Back in 2007, a report for the National Academy of Sciences found that many hospitals and emergency departments “are already maximizing their existing capacity after years of capacity shedding designed to reduce costs.”
It cited CDC surveys that not all hospitals have plans for creating extra capacity in the case of a disaster. It said that hospitals in most large cities “have problems dealing with a multiple-car highway crash, much less the volume of patients likely to result from a large-scale disaster.” The report concluded that “the lack of adequate hospital surge capacity is a serious and neglected element of current disaster preparedness efforts.”

Get daily updates from WHYY News!
Torradas said that is still the case now.
Another issue that emergency planners now have to prepare for is disinformation, even from the federal government. Toner at Johns Hopkins said in the early days of the outbreak, he and his colleagues sounded the alarm.
“[It] led to a lot of us being called fear mongers and got a lot of nasty emails from people, saying that we’re trying to undermine the president and what we were saying was ridiculous,” Toner said, adding that he’s received hundreds of angry emails.
Murray from the American College of Emergency Physicians said that is something that emergency planners did not fully prepare from the get-go, but it is something they will be thinking about when it comes to planning for a second wave of COVID cases.
“Overcoming that … is going to be a struggle, because people have made their minds up one way or the other and I talked to some friends who I can’t even convince that this is real, and I honestly don’t know how you would address that,” Murray said.
—
This article was updated to correct attribution for a quote.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)