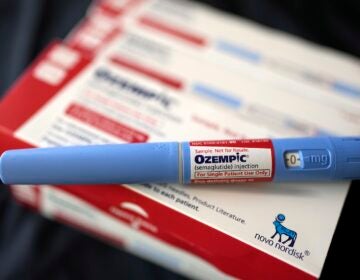
To-go drugs aim to keep repeat patients out of the emergency room
It can be hard for some ER patients to fill prescriptions, so a new Temple program sends them home with medicine, to keep them from coming back.

Cooper University Hospital in Camden, N.J. (Mel Evans/AP Photo)
Kraftin Schreyer is the medical director of the emergency department at Temple University Hospital’s Episcopal Campus in Kensington.
She knows that many of her patients use the emergency department as their first and often the only point of contact with the health-care system. Because of that, she’s always adjusting doctoral procedures to be more nimble and meet patients’ needs.
Schreyer noticed she saw the same patients over and over again for the same conditions. The hospital’s ER serves a lot of patients who use intravenous drugs, so some of the most common issues are skin and tissue infections.
She also saw a lot of people come back repeatedly for asthma.
Infections can be easily treated with antibiotics — if the person completes the full regimen of care.
But instead, Schreyer saw the opposite. Patients were readmitted to the hospital for the same conditions — only they were worse.
“That was a lot of the times because they didn’t have access to the medications that we had recommended they get,” she said. “Sometimes, they were being discharged in the middle of the night. Sometimes, it was on the weekends when pharmacies weren’t open, or they simply had no means to get to a pharmacy or no funds to fill a prescription.”
So Schreyer decided to cut out the middleman.
She made a list of the top medications prescribed for those conditions and cleared them with the Temple outpatient pharmacy. Now, when a patient who doesn’t have insurance or wouldn’t otherwise be able to get medication needs an inhaler, steroids, or antibiotics for an infection, a doctor writes the prescription, a nurse picks up the medication, and the patient leaves the emergency department, drugs in hand.
Most of the medications on the list are available in generic form, so the cost to the hospital is low. Schreyer hopes the program can offer a lot of bang for its buck — re-entry can be expensive for hospitals and patients.
John Flamma, who heads the emergency department at Penn Presbyterian Hospital, agreed.
“If you can spend $3 to keep somebody out of the hospital, I mean it doesn’t take an economist to say that’s probably a good thing,” said Flamma, whose ER has been operating a similar program for the past five years on a roughly $1,500 annual grant-funded budget.
Penn’s program offers month-long courses of medication to prevent seizures, hypertension and diabetes, as well as providing antibiotics.
Measuring the success of such programs can be tricky because patients don’t always return to the same emergency departments for care. For that reason, Flamma doesn’t measure the impact of the Penn program, though he estimated that it sends 30 to 50 patients a year home with meds.
Schreyer said she plans to monitor if patients who are given the drugs come back to the emergency department or any part of the Temple Hospital system with the same condition.
There is evidence to show a lot of potential payoff from these types of programs. One study at the University of Maryland Medical Center found that sending patients home with prescription medication reduced readmission by 50 percent.
“Providing patients with meds at discharge is a great way to remove three of the biggest barriers to filling prescriptions: cost, transportation, and wait times,” study author and Massachusetts General Hospital pharmacist Bryan D. Hayes said via Twitter.
Despite the potential payoff, such programs are not common: Penn and Temple are the only emergency departments in town that have to-go med systems in place. The heads of both departments said they didn’t have many models to look at when developing their programs.
“We don’t really have any clear budget or clear plan,” Schreyer said. “We’re just going to monitor it and see how it goes.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.