The Freddie Gray effect: Black Americans’ mental health suffers after police killings
The negative effect on African-Americans’ mental health peaked in the month after a police killing, and it dissipated after three months.
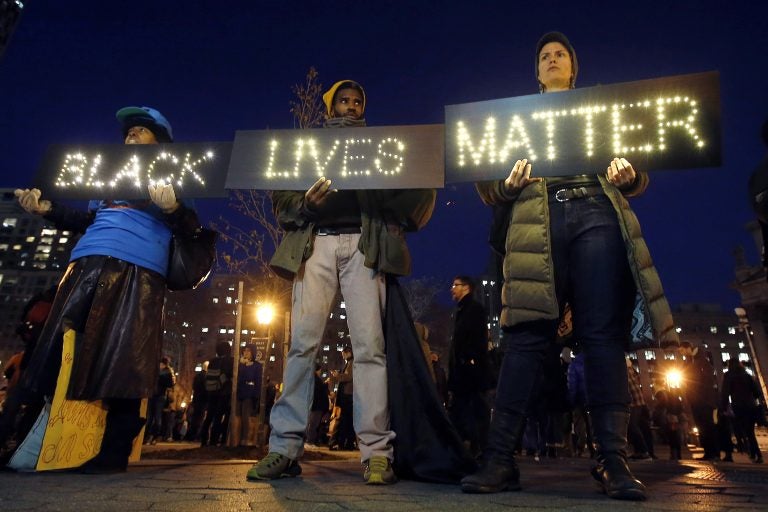
In this Dec. 4, 2014, file photo protesters rally in New York's Foley Square against a state grand jury's decision not to indict the police officer involved in the death of Eric Garner. (Jason DeCrow/AP Photo, File)
When Baltimore resident and social activist Erickka Bridgeford heard about the killing of Freddie Gray, she felt horrified — and, more than that, she questioned her self-worth.
“It pulls up something in you that reminds you like, ‘Oh, right, this is what they think we are worth, this is who they think we are and what we deserve,’ ” she said.
It turns out the emotions Bridgeford described are part of a bigger public health problem. A new study published in the Lancet found that police killings of unarmed African-Americans contribute significantly to poor mental health among other black adults living in the same state. It affects their mental health nearly as much as having a chronic disease such as diabetes does.
Researchers looked at health survey data from the U.S. Behavioral Risk Factor Surveillance System, a national random survey of non-institutionalized adults 18 and older. As part of that survey, participants were asked, “Now thinking about your mental health, which includes stress, depression, and problems with emotions, for how many days during the past 30 days was your mental health not good?”
They then compared that data with data from the Mapping Police Violence database, which has tracked police killings in the United States since 2013.
They found that police killings of unarmed black Americans contributed 1.7 poor mental health days per year, or 55 million excess poor mental health days per year among the 33 million black adults in the United States. To put that number in perspective, the researchers estimate that diabetes — which has known negative mental health effects on patients — contributes about 75 million poor mental health days per year among African-Americans.
The negative effect on African-Americans’ mental health peaked in the month after a police killing, and it dissipated after three months.
What surprised researchers most, aside from the magnitude of the problem, was that these events negatively affected people who had no personal connection to the victims.
“They don’t necessarily implicate or affect anybody directly, but the fact that they happen provides a signal about what society is like to people that gets under their skin,” said Atheendar Venkataramani, assistant professor of health policy at the Perelman School of Medicine at the University of Pennsylvania and a co-author of the study.
Venkataramani said the data also probably understate the problem. The study design only looked at the impact on people who reside in the state where a police killing happened. But many events, including the killings of Philando Castile in Minnesota and Eric Garner in New York, were known beyond those states and were discussed nationally.
“You have a control group of people, that we’re considering a control group, that actually is affected by a lot of these events,” Venkataramani said. “And so when you look at the difference between the people who are exposed [to news about these killings] and who we consider to be unexposed, it probably vastly understates the true difference in the mental health burden.”
Researchers observed no effect on the mental health of white individuals, nor did they see an effect on black or white mental health when the person police killed was armed.
More than anything, Venkataramani said, the results show that police violence is a public health issue.
“Structural racism is a potentially really important source of mental health morbidity among black Americans,” he said, “and it’s something that we should continue to try to tease apart.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





