Why Pennsylvania’s women are struggling to find estrogen patches for menopause hormone therapy
The nationwide shortage is being driven by a steady rise in demand for menopausal hormone therapy that is outpacing current patch supply.

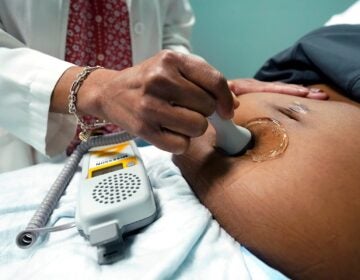
FILE - A low-dose estrogen skin patch is seen on Tuesday, Oct. 2, 2012. (AP Photo/File)
From Philly and the Pa. suburbs to South Jersey and Delaware, what would you like WHYY News to cover? Let us know!
Last summer, Angela Motter started experiencing some changes that began to interfere with her fast-paced job in health care.
“I was just having brain fog and just feeling tired all the time, irritable,” she said.
For a while, the 48-year-old Berks County resident chalked it up to the daily pressures of being a mother, caring for her family and having a career.
When she started suffering hot flashes and night sweats, Motter realized she must be in perimenopause, the time when women’s hormones like estrogen and progesterone begin to fluctuate before sharply declining in the next phase, menopause.
Motter found relief with a twice-weekly transdermal estrogen patch, which steadily releases the hormone through her skin. It is considered one of the safest, low-risk forms of menopausal hormone therapy, making it a popular choice among patients and providers.
“Almost right away, I started seeing improvement in mood, seeing an improvement in hot flashes,” she said.
But an ongoing national shortage of estrogen patches is creating stress and anxiety among women who rely on the medications to manage what can be extremely disruptive symptoms that have a profound impact on mood, cognition, sleep and more.
The shortage is largely being driven by a steady increase in demand for hormone therapy as awareness and education among women about their treatment options grows.
Health providers and menopause specialists like Dr. Kathleen Jordan said they’re helping their patients find alternative brands, formulations and estrogen hormone products to limit disruptions, but worry the shortage could worsen before it resolves.
“We really do need the supply issues addressed,” said Jordan, who treats patients across the country through Midi Health, a national virtual health company headquartered in California that specializes in menopause care. “And, you know, sort of the public asking for it is important. It’s public outcry that will drive the supply chain issues resolution, I think.”
Interest in hormone therapy grows after decades of underutilization
Hormone therapy has proven highly effective in not only treating menopause symptoms, but also in preventing bone loss and breaks. Some data suggests it can also reduce cardiovascular disease risk when prescribed early.
At the turn of the century, an estimated 40% of menopausal women used at least one type of hormone therapy. But use plummeted following the publication of a 2002 study that linked combination estrogen-progestin therapies to an increased risk of heart disease and breast cancer among older, post-menopausal women.
It led to widespread fear and concern, despite health experts who later determined that the results had been misunderstood. The U.S. Food and Drug Administration even added a black box warning on estrogen and combination progestin products for menopausal women.
More recent research has since found that the risks are generally low for women currently in menopause experiencing symptoms, and that evidence showing benefits is strong. The FDA announced last November it was removing “misleading” black box warnings on products.
Still, less than 5% of women currently use hormone therapies today, but the number is growing as access to menopause specialists who are knowledgeable about treatment options increases.
Estrogen patches are considered “a pillar of menopausal hormone therapy” for their reliability and high safety profile, Jordan said.
“The patches are beloved because it’s a continuous release. You don’t have to remember to do it very often,” she said. “And they’re covered by insurance often. So, it’s stressful when these aren’t in stock because it can mean extra time and effort to either locate the stock or it can mean switching to something that might not be as well-covered by your insurance.”
Supply chain issues and patch shortages continue
Motter was able to easily pick up her first prescription of estrogen patches back in August, she said. But by the time she had to refill, her local chain pharmacy didn’t have it in stock.
She drove about an hour away to get her medication at a different chain location. Since then, she’s switched patch brands at least twice and enrolled in the pharmacy program at Costco as she’s had to chase supply.
“It is very stressful when you find something that works for you and improves your quality of life, and then you’re not sure if you can get it again,” Motter said.
Dr. Anna Groysman, an endocrinologist at Penn Medicine, said she is seeing the shortage issues play out daily among the patients she treats in Bucks County.
Groysman and her colleagues often find themselves calling dozens of pharmacies on behalf of their patients, or working with them to find a similar brand and dosing that could work.
In some cases, patients may be eligible to switch to other forms of estrogen hormone therapy, like oral pills, gels, creams, vaginal rings that can emit estrogen or other compounded products.
But the changes are not always simple, Groysman said.
“Just when I found what they need, I’m having to have these women go through a second round of pains in finding what dose works,” she said. “And it really can take six to eight weeks or even longer to see if a given dose works for them. That’s a long time to wait.”
Oral pills also come with slightly higher risks of clotting, stroke and heart attack, Groysman said, and may not be a good option for people with certain chronic conditions. Health insurers are also less likely to cover gels, which are more expensive.
As someone switches products, they may be required to get new prescriptions and prior authorization from their insurer for coverage, which health providers say only creates additional barriers and more delays.
“We’re torturing them with not providing the treatments that they need and deserve and that they’re on already,” Groysman said.
The best thing people can do right now is to work with menopause health care providers to ensure that they find some solution in continuing their hormone therapy, Jordan said. She recommends patients submit a refill request as early as they are allowed to ensure they have time to manage any issues if their pharmacy is out of stock.
“We need to make this easier for women,” she said. “This should not be that hard. But it is right now.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.