Penn Medicine accepting pregnant women in COVID-19 study of convalescent plasma
Historically, those expecting babies have been excluded from non-pregnancy related clinical trials.

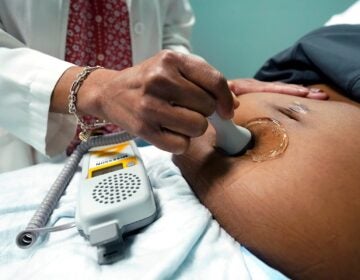
Dr. Michal Elovitz is one of the Penn Medicine researchers involved in a clinical trial for COVID-19. Its one of the first in the world to accept pregnant women. (Courtesy of Penn Medicine)
Pregnant women now qualify for Penn Medicine’s convalescent plasma study, in which scientists seek to learn whether the blood of recovered COVID-19 patients can help hospitalized patients fight the virus.
It’s the first time Penn Medicine has enrolled pregnant women in a clinical trial that’s not pregnancy-specific. Officials there say they believe this is the only non-pregnancy-specific coronavirus trial accepting people who are expecting.
Of the 900 COVID-19 clinical trials that have been conducted worldwide, fewer than 2% have been pregnancy-related, and most exclude pregnant women altogether, according to Penn Medicine.
Historically, pregnant women worldwide have been excluded from most clinical trials, with the exception of pregnancy-focused studies.
“We have a natural misplaced default action to exclude pregnant women from trials. It’s a very paternalistic view; it’s an overprotective view,” said Emma Meagher, vice dean for clinical research at the Perelman School of Medicine. “… And part of that historically is you have to consider two lives, and the impact on the child is virtually impossible to assess in utero.”
“It was done with a sentiment to protect the mother and child, and I think the restrictions have gone on so long we have forgotten to look at the question carefully,” Meagher said. “And what COVID really brought to the forefront was a need for us to challenge this accepted principle and dogma that pregnant women cannot be enrolled. And it was so stark, because at the time these studies were designed, there was no accepted therapy.”
Excluding pregnant women from clinical trials has left scientists somewhat in the dark, said Michal Elovitz, vice chair for translational research at Penn Medicine and the Hilarie L. Morgan and Mitchell L. Morgan President’s Distinguished Professor in Women’s Health.
“Unfortunately, after decades of following that, what we are left with is no science to direct appropriate and effective care to women. At the height of the pandemic, when there are all these clinical trials to try and find ways to decrease morbidity and mortality, at the end we are going to be left guessing for pregnant women again, because they’re not involved in a clinical trial,” Elovitz said.
“The use of most interventions in pregnancy are based on non-pregnancy trials…Take a randomized clinical trial for most antibiotics; all of those trials were not done in pregnant women,” she added. “We assume we’re doing benefit, but we don’t actually know.”
Convalescent plasma therapy in itself is not new, though its use with patients hospitalized with COVID-19 is still experimental. (With the exception of remdesivir, no drug has been proved safe and effective for treating the virus.)
Those who have recovered from COVID-19 have antibodies in their blood that have helped them fight the virus. Researchers want to know if the blood of recovered patients can be donated to patients with severe cases of COVID-19 to help them fight it as well.
Penn Medicine is conducting two trials for all COVID-19-infected patients, including pregnant women: One is for individuals who are on ventilators or in the ICU; the second study is a randomized controlled trial for moderately sick patients, in which half of the participants receive convalescent plasma and half do not.
So far, there have been 126 donors, 18 intensive care patients, and 11 moderately sick patients involved in the study. Penn Medicine aims to enroll a total of 50 ICU patients and 80 moderately sick patients.
More than 125 of Penn Medicine’s COVID-19 patients have been pregnant women. Last month, the health system began testing all women in labor, and nearly 4% tested positive for the coronavirus. But thus far, a pregnant woman has not been enrolled in the convalescent plasma study.
What the data says
Data about the effects of COVID-19 on pregnant women differs, Elovitz said. For other coronaviruses, such as SARS and MERS, as well as the H1N1 influenza, there is an increase in maternal morbidity, or illness, and mortality.
The limited data on COVID-19 suggests there is not greater morbidity in pregnant patients compared to non-pregnant patients, but that has to be put into the context of the pandemic, she said.
“So, when there are a lot of people who are infected, that means more pregnant women will be infected, and we have seen a number of very severe cases at our institution at Penn — we’ve had about seven women who required mechanical ventilation during their pregnancy for COVID-19,” Elovitz said. But because the virus has only been in the United States for a few months, “it’s hard to make definitive conclusions.”
“It seems while pregnant women may not be at higher risk than non-pregnant, they are still definitely at risk, and definitely can have severe disease — so it’s imperative we understand how they might respond, or benefit or not benefit, from treatments that are being offered to combat the disease.”
There’s still a debate about whether the virus affects the placenta, and if it does, whether it causes fetal infection, Elovitz said. Some studies have shown the virus does not transmit from mother to baby, but there have been other reports of the virus in the placenta or in a fetus or newborn.
“I think the question most people have is, ‘Does it affect the fetus and the placenta because the mom becomes so sick? Or because the mother has an exaggerated inflammatory response that affects the placenta, subsequently affecting the fetus?’” Elovitz said. “We won’t know for months or a year whether COVID-19 in pregnant women affects miscarriage, preterm birth, or fetal demise.”

Show your support for local public media
It’s difficult to estimate how many pregnant women will enroll in the study, Meagher said, especially as the number of new hospitalizations for COVID-19 has been declining. However, she said the trial is prepared for a second wave of the coronavirus.
“We anticipate keeping these trials open, expecting another surge of cases in the fall, and given the pregnancy rate in our geographic area, I will be optimistic we will enroll pregnant women into the trial,” Meagher said.
“When we designed these studies, we were in the thick of it, we had so many patients and had several pregnant patients at the time, and then the number of cases decreased sooner than we anticipated they would,” Meagher said. “So I think it will depend on what does the second wave of this look like? What will be the impact of protesting and peaceful demonstrations? Will that cause an uptick in cases in women who are maybe in early pregnancy? We’re sort of guessing with numbers that so far have been pretty unpredictable in delivering on our expectations.”
Meagher and Elovitz said they hope this clinical trial will open the door to more vigorous conversations and continued advocacy around reducing the barriers for pregnant women’s participation in such trials.
“We need to think about the best way to care for moms and their babies, and if we’re going to do that, we have to have the best science, and the best science usually comes from anonymized clinical trials. And so, while people have leaned toward benevolence, and the idea that we don’t want to harm — by not doing the clinical trial in these patients, we are actually not able to do good,” Elovitz said.
“Many of my colleagues believe pregnant women and lactating women should be included, NIH [the National Institutes of Health] believes in it, I think the majority of people who do this kind of work believe in it, and I think pregnant patients want to be included so they can get the best care,” she added. “And I think it’s a matter of just pushing that needle to say, ‘Yes, let’s do it,’ and actually make those words action, which we have been fortunate to do with this trial.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)