Penn-Inovio DNA vaccine prevents MERS infection in monkeys
Listen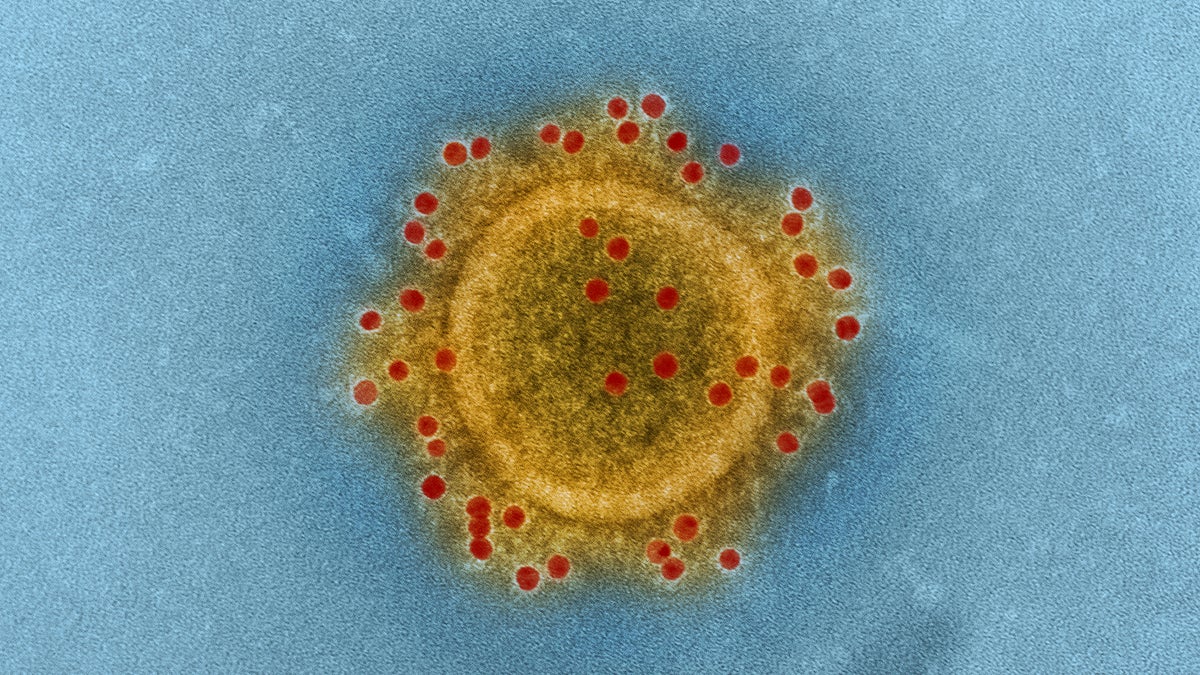
The Middle East Respiratory Syndrome (MERS) coronavirus.(Image courtesy of NIAID)
A synthetic DNA vaccine has successfully triggered an immune response in rhesus macaques and protects the animals from Middle East Respiratory Syndrome, according to researchers.
The study, published in the journal Science Translational Medicine, is one of the few to demonstrate such a complete response in monkeys; it’s a first for a DNA vaccine against MERS.
“One-hundred percent of the animals developed antibodies after just two injections,” said David Weiner, a molecular immunologist at the University of Pennsylvania and the senior author of the new work. “And 100 percent of the animals were protected when challenged with a disease-causing strain.”
The MERS coronavirus produces a severe respiratory illness in people, and is deadly in 30 to 40 percent of cases. Although camels are thought to initially transmit the virus to humans, those infected can spread it to other people by coughing.
Indeed, an outbreak of MERS in South Korea earlier this summer sickened more than 180 people and led to 36 deaths. According to the World Health Organization, last week Saudi Arabia reported 12 cases over a three-day period. No specialized treatments or vaccines exist for the disease.
In the current study, researchers vaccinated eight macaques three times over six weeks. Shortly after vaccination, the animals began churning out specific antibodies and also mounted a T cell response. When challenged with the MERS virus, just two of the vaccinated monkeys developed small lesions in the lungs, and those cleared within a few days, Weiner said. In contrast, the four control macaques developed severe pneumonia-like symptoms that persisted until the end of the study.
Other experiments showed the vaccine could produce neutralizing antibodies in camels, a natural host of the MERS virus.
The newly tested vaccine is a piece of DNA that includes sequences from a variety of different MERS viruses’ spike proteins — a design accomplished on the computer that makes it more difficult for the virus to simply mutate and render the vaccine ineffective. Because it’s just nucleic acid, Weiner said, it doesn’t pose the same risks as a traditional vaccine.
“It’s non-live and it doesn’t grow, and it can’t spread,” he said.
To work, the DNA must enter cells where the spike protein is temporarily made and available for the body to react to. In this case, scientists relied on delivery technology developed by Inovio Pharmaceuticals, a biotech company based in Plymouth Meeting that contributed to and partly funded the research.
“We use a delivery system that uses a small short burst of electrical energy to coax open our cell membrane to allow our products to get into our cells,” explained J. Joseph Kim, the Inovio president and CEO.
Given the promising results, he said, the company will begin a phase I clinical trial by the end of the year to evaluate vaccine safety in people.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.

