Letter: Science, not bias, should rule response to Philly ‘safe-injection’ site proposal
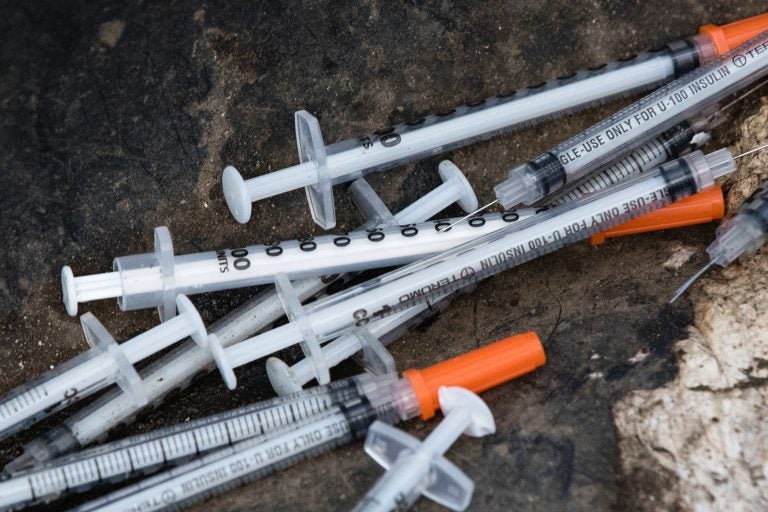
Philadelphia officials cleared the way for a safe injection site for drug users. But there are many details to work out before the idea can become reality. (Matt Rourke/AP)
WHYY recently published a blog post by Solomon Jones, a local columnist and radio host, called “Philly should say no to ‘safe-injection’ sites” (Jan. 26). Jones’ point about the political winds shifting with the racial demographics of our stereotypical “drug user” is fair and correct. The burden of surveillance and incarceration has fallen disproportionately on the poor and on people of color in Philadelphia, especially in neighborhoods like Kensington. But in making his argument against safe injection facilities, he offers no solutions to help those who would use them. Worse, he relies on fraudulent research.
I am a public health researcher who has worked since 2007 with people who use drugs. Since then, I’ve heard a refrain from people working in my field: The only thing you really need to get into drug treatment is to be alive. Safe injection facilities save lives. They give people using drugs opportunities for a healthier and safer future. Overdose deaths in Philadelphia exceeded 1,200 people in 2017. Are we really willing to accept this massive death toll in our city?
A safe injection facility, or SIF, is a place where people who use drugs can go to safely use them. They bring the drug, and the SIF provides them with sterile equipment and a safe place in which to use. Trained staff are on hand to intervene in the event of an overdose. Outreach workers can link clients to medical care, social services, and yes — even rehab or other drug treatment, should that individual be ready for it. The evidence in support of safe injection facilities is clear, consistent, and has been written about multiple times since city officials announced their support for creating a Comprehensive User Engagement Site in Philadelphia. (This site would operate similarly to a SIF but provide a broader range of services.)
Drug use is a divisive issue. Like abortion and gun rights, it brings out our emotions and moral arguments. But while there is a wealth of solid research about how we can address the opioid epidemic, Jones instead presents biased rhetoric masquerading as science.
Jones’ essay links to a decade-old publication that he refers to as a “study.” It is published by The Journal of Global Drug Policy and Practice, a publication that is a running joke among addiction researchers. It’s written by Dr. Garth Davies, a criminologist with a background in counter-terrorism. Yet Davies criticizes a host of peer-reviewed publications on the benefits of SIFs, benefits that have consistently appeared in esteemed publications such as The New England Journal of Medicine, The Lancet, and Addiction, among others.
Davies was paid to write this attack on science. His “study” came out just as Vancouver, British Columbia, was embroiled in the same public debate that Philadelphia is having now, around a safe injection facility there. Vancouver had managed to open their facility, called InSite, in 2003. The Royal Canadian Mounted Police, unhappy with the situation, secretly commissioned Davies to write his manuscript. The commentary was presented as a peer-reviewed study. In fact, The Journal of Global Drug Policy and Practice is not peer-reviewed, nor is it a journal at all; it is a website funded by the Florida-based Drug-Free America Foundation. (A previous iteration of the Foundation ran rehab centers for youth using systematic physical abuse.) Yet, Davies’ article, along with a piece of commentary by Colin Mangham, another paid researcher, was used to criticize the very first SIF in North America.
Opioid users have been dying of overdoses for a long time. Until now, our country’s approach to drug use has been motivated by a moral tone, making drug policy punitive in nature. A compassionate and evidence-based response to crack cocaine use was not present in the 1980s and 1990s. With bipartisan recognition that the War on Drugs is a failed one that has done far more harm than good, we are hopefully moving from an emotional response to drug use to one that is based in science and what we know works. SIFs work. A Comprehensive User Engagement Site in Philly can be expected to replicate the benefits found in Vancouver and other cities across the world that have opened SIFs: higher enrollment in drug detox, a reduction in overdose deaths, and fewer discarded syringes in the surrounding neighborhood.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



