Delaware hospital curtails opioid prescriptions in effort to combat addiction
Christiana Care has cut opioid prescribing by as much as half in some departments by adopting guidelines and best practices for post-surgical recovery.
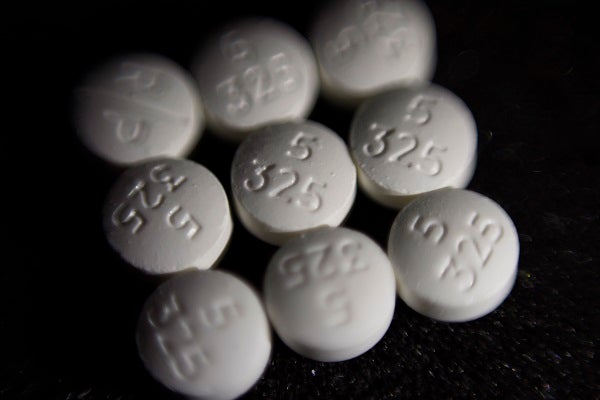
Doctors are working to prescribe fewer opioids in Delaware. (Patrick Sison/AP Photo, File)
In an effort to decrease chronic opioid use, combat addiction and prevent overdose deaths, health care professionals in Delaware are striving to reduce opioid prescriptions.
Christiana Care has cut opioid prescribing by as much as half in some departments by adopting guidelines and best practices for post-surgical recovery.
“Over the past few decades, surgeons have been prescribing more pills than needed because they were trying to do the right thing, and there wasn’t any literature out there showing how many pills to give,” said anesthesiologist Dr. Matthew Powell. “Now we have that information, we’ve implemented those guidelines, which has been very successful.”
Last year, 345 people died from overdoses in the state — up 12 percent from the year before. And health care professionals and advocates say many people who struggle with heroin addiction began by taking opioids prescribed by a doctor.
“If we have more of an effort to use other means to treat pain than opiates, we’re going to potentially reduce the number of people that get addicted to opioids and then move on to heroin as well,” said Dave Humes of atTAck Addiction.
“I’ve always said every story is the same, yet every story is different, but we hear a lot about people who have started on opiates. It’s a common thread,” he said, adding that the public is becoming aware that manufacturers misrepresented the opioids as not addictive.
Overprescription of opioids can lead to dependency or abuse, while leftover drugs can get into the wrong hands, Powell said. Patients who are prescribed more opioids than needed may use them later for pain, depression or trouble sleeping.
“We’re trying to optimize the amount of pills given out so patients have enough to get over whatever they’re being prescribed for, but not too many it starts causing diversion, and increased abuse, and increased chronic opioid use,” Powell said.
“What we’re trying to aim toward is prevention, so that we try to cut off the supply before it starts. This is a lot more effective and efficient and long-lasting solution.”
Declining prescription rates
Christiana Care reports a 40 percent decline in opioid prescriptions after OB-GYN and general surgery procedures; a 50 percent drop among discharged emergency department patients; and a 37 percent decline in primary care patients on chronic opioid therapy for pain as part of a pilot project.
The hospital borrowed guidelines from a University of Michigan initiative called the Opioid Prescribing Engagement Network to reduce opioid prescriptions after surgical procedures.
Doctors are now encouraged to measure pain in terms of function — such as ability to work, sleep, and perform everyday tasks.
Doctors have been using alternative methods of pain relief, such as a nerve block after surgery combined with an anti-inflammatory medication.
Doctors at Christiana Care also worked to identify patients at high risk of addiction and wean them off opioids. They have also helped patients struggling with addiction receive medication-assisted treatment.
Christiana Care has focused on 20 different procedures, but would like to expand to others. The facility also wants to reach out to other health systems to make it a statewide effort, Powell said.
The effort to reduce opioid prescriptions is not new, however. At the end of last year, the Division of Professional Regulation reported a 12 percent drop in opioid prescriptions statewide compared with the first quarter of the year.
The division attributed the drop to new regulations that limit opioid prescriptions to seven days — unless a prescriber can prove it’s necessary following a physical exam, and after checking the patient’s history in the state’s prescription database.
Palliative care physician Dr. John Goodill, a member of the Medical Society of Delaware, said facilities across the U.S. are working to reduce opioid prescription.
EBrightHealth, a coalition of several health care facilities in Delaware, also plans to roll out similar guidelines and best practices, he said.
“In the past, we’ve been in the habit of using and prescribing a lot more opiates than needed, and we’re just kind of recalibrating that and finding out through evidence-based research and data that we can get by with either no opiate prescribing or much less than we were used to in the past,” Goodill said.
Striking a balance is important, however. Goodill said some people do benefit from taking opioids.
“We don’t want to go too far in the other direction where opiates aren’t available to people who could benefit from them, so we have to be careful and mindful and use the information we have to do safer, more effective opioid prescribing,” he said.
Delaware’s newly formed Behavioral Health Consortium, recommended by Gov. John Carney’s Action Plan for Delaware, has been working to enact 114 recommendations outlined in a three-year action plan.
The consortium was a recommendation of Gov. John Carney’s Action Plan for Delaware to address the opioid crisis in the state. The group consists of health officials, law enforcement, state leaders and advocates.
The group is also focused on overprescription, said Lt. Gov. Bethany Hall-Long, who leads the consortium of health officials, law enforcement, state leaders, and advocates.
“I also want to reiterate prescription is just one component,” she said. “It’s also behavioral health issues, not just substance abuse disorder. Not all persons addicted came out of this from a prescription — perhaps the person was self-medicating for depression, anxiety or bipolar disorder. So again, we have to make those distinctions.”
“But today I think we can give a shout out to Christiana and the other hospitals, independent practices, dentists and others who are thinking before they write a prescription what is the best avenue for the patient. These reductions in prescriptions will absolutely help us as we address the heroin epidemic.”
Goodill said more work is needed to ensure treatment is readily available in a number of health care settings.
“Addiction has been on the margin of mainstream medicine, and we need to develop ways of treating it that move toward the mainstream where all providers can recognize it, refer it and treat it as they see it,” he said. “We have to remove the stigma and marginalization that’s gone on for a long time.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.