Sickle cell disease still persists 100 years after discovery
Listen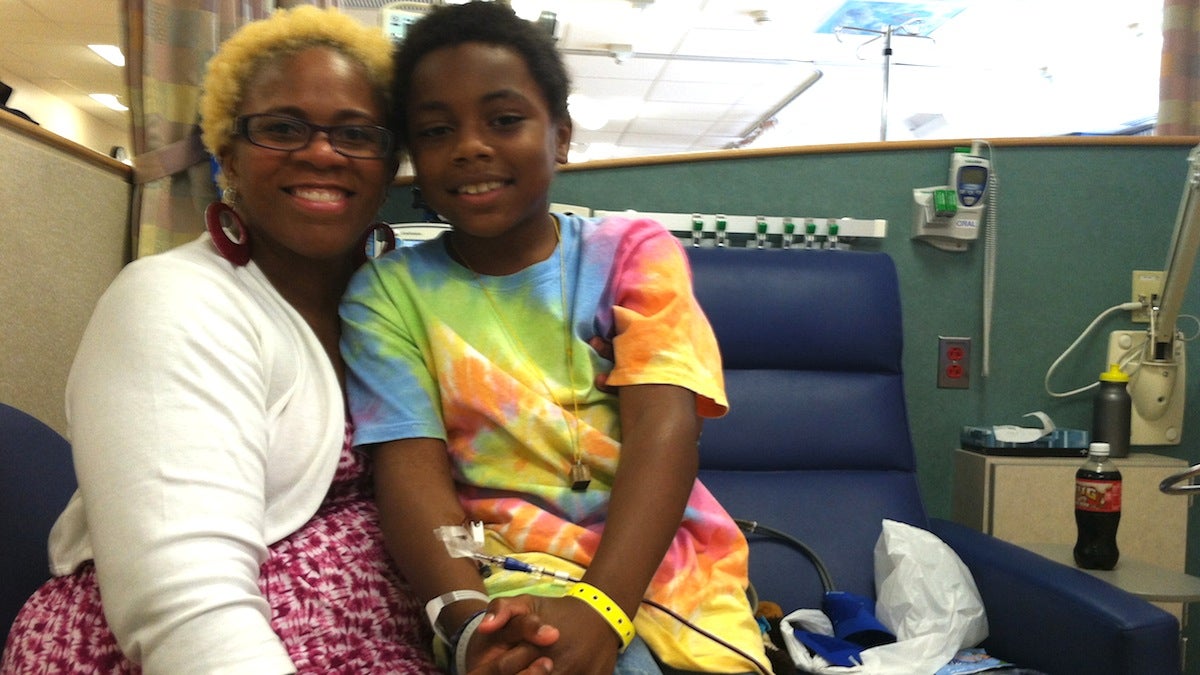
Heather Hodges and her son
A look at sickle cell disease and why there aren’t more promising options for treatment.
Eight year old Nadir Tinsley is getting restless. He’s hooked up to a pint of red blood at Children’s Hospital of Philadelphia, pushing his IV pole down the hall. He wants to go play Wii with a friend in the activities room. Nadir’s mom, Heather Hodges, gives up on trying to make him stay put so the little boy happily wheels his way to the game.
“Nadir’s a ball of energy,” says Hodges. “But usually when its getting time for his transfusion, he’s not so energetic. But after he gets the blood, ohh it’s wonderful! He’s so —extra!”
Nadir has sickle cell disease. The active eight year old gets blood transfusions every three weeks to help him avoid strokes as part of his treatment for the disease.
Sickle cell disease targets red blood cells changing their shape and affecting their ability to carry oxygen and pass through blood vessels. The cells become stiff and sticky, clogging vessels or breaking up during circulation. One common, debilitating symptom is pain – it can be severe and incapacitating sending patients to the ER, and it can persist as constant, chronic pain for years. Patients suffer from anemia, organ damage and failure, stroke and a host of other complications that can lead to an early death.
Sickle cell disease is genetic. It affects about 100,000 people in the United States, mostly people of African descent but also other ethnicities. It is considered an “orphan disease”, defined as a disease that affects fewer than 200,000 individuals. Even though it is categorized as a rare disease, it’s one of the most common genetic disorders in the United States.
‘The forgotten disease’
Doctor Kwaku Ohene-Frempong is the attending hematologist at Children’s Hospital of Philadelphia, and the former director of the hospital’s Comprehensive Sickle Cell Center. He’s been studying and treating the disease for 40 years and knows firsthand how devastating it can be. Last year he lost his 40 year old son to complications from the disease. The average life span for someone with the disease is 40 to 50 years old.
“People used to hear a lot more about sickle cell disease in the 70s than now and often they think maybe this problem has been solved,” says Ohene-Frempong. “It hasn’t been solved yet. There are many more children with the disease now than before.”
Despite the fact that it has been known and studied for over 100 years, and it was one of the first diseases identified as being caused by a flawed molecule – hemoglobin, there is no cure and it lags behind similar diseases in both research funding and media attention.
“Everybody thought that if we embarked on gene therapy, sickle cell disease would be one of the first to be treated because it is so well known. But we’ve had gene therapy for 15 years or so and not a single bona fide attempt at gene therapy has been done on sickle cell disease,” says Ohene-Frempong.
While there are treatments for the disease, and life expectancy has increased over the years, patients and advocates are frustrated there hasn’t been more progress. There is no treatment that will completely block complications and no universally effective cure on the horizon.
Sickle cell disease is often called “the forgotten disease,” but there are many patients and doctors working for better treatments and an eventual cure.
Disparities and diagnoses
If you are up early enough, and brave enough, you might be one of the regulars at Marjorie Dejoie’s boot camp fitness class at the 12th Street Gym in Center City.
Katy Perry’s girl-power anthem “Roar” pours out of wall mounted speakers. “It’s the M.A.D. Fit morning wake up call!” says Dejoie, as she turns up the volume, turns up the bass and turns up the tempo to energize the class.
Dejoie’s class is a one-hour, customized version of cross fit training called M.A.D. Fitness. If you watch Dejoie in action at 6 a.m., you might think that “mad” refers to anybody willing to submit to pushups at that hour. But the letters stand for “Make a Difference,” which is what Dejoie strives to do, helping her students build strength and stamina.
She teaches M.A.D fit twice a week, is a practicing physician and the medical director of the Philadelphia and Delaware Valley chapter of the Sickle Cell Disease Association. Dejoie has been teaching M.A.D. Fit since med school. She starts each day at 4:30 am and barely has enough time to fit everything in.
Doctor Dejoie has sickle cell disease and for her, fitness is “prescribed.” It’s as important to her treatment as drugs and she has written about managing sickle cell pain without the use of drugs.
“Even if you can never stay ahead of a chronic illness, this helps me keep going,” she says. “I was diagnosed late in life. I wouldn’t be as healthy without it.”
Dejoie suffered for years from debilitating attacks of severe pain, called a pain crisis. She was mystified by her symptoms.
“I would get into a lot of pain and nothing would seem to alleviate the pain. And I couldn’t reboot, I couldn’t get any energy or even think until the pain subsided.”
For years doctors did blood work and took x-rays but never tested her for sickle cell disease.
“At one point they thought I was just making it up,” says Dejoie. “And I was like ‘trust me, I would not make up what I’m going through right now.'”
When Dejoie was born in New York in 1971 sickle cell disease was not included in the mandatory battery of newborn screening. The testing was not mandatory across the United States until 2006, although some states did test prior to the national mandate.
She was diagnosed at 23 while she was a medical student at The University of Pennsylvania. She says she was lucky to be a student at a teaching hospital that was experienced in treating the disease.
In my first year I had a crisis and one of the administrators looked at me and said, ‘Your symptoms sound like sickle cell disease,’ and I said, ‘What in the world is that?”
Doctors and advocates celebrated mandated testing but the lateness ofthe mandate is still frustrating.
Pushing for public awareness
At a time when branding and messaging extends to disease awareness – think pink ribbon campaigns for breast cancer and red ribbon campaigns for AIDS – sickle cell disease is still playing catch up. In looking at disparities, the disease is often compared to hemophilia, a much rarer blood disease that seems to have better public recognition — and cystic fibrosis, also more rare, but which annually brings in about 10 times more research funds.
Dr. Carlton Haywood is a core faculty member of “Johns Hopkins Berman Institute of Bioethics.” He has written about the role that race plays in the health care experiences of sickle cell patients. He recently had his second hip replaced due to complications from the disease. He had his first hip replaced in his early 20s after years of joint pain.
His recent publication, The Impact of Race and Disease on Sickle Cell Patient Wait Time in the Emergency Department, found that sickle cell patients experienced wait times 25 percent longer than the “General Patient Sample.” This occurred even when sickle cell patients were assigned higher (more urgent) triage numbers.
He says “it would be naïve to overlook” the notion that race might be behind some of the disparities in funding and research advances for other diseases compared to sickle cell. He points to the predominately white “demographic make up of hemophilia and cystic fibrosis.”
“Given the nature of race and race relations in the history of the United States and given the history of this disease, and the fact that it has been mistakenly thought to be a purely race specific disease that only affects the black population and no other, I think that it certainly has played a role.”
Haywood says it’s impossible to quantify the affects of race or racism on the advancement of treatment and research, but the issue is troubling.
“When you take a look at some of the wide resource disparities between sickle cell disease and other conditions, unfortunately it still begs the question, it still raises the concern.”
Hoping for a cure
Since newborn screening was mandated, the treatment landscape has looked more promising. The use of penicillin, starting early in chldhood, has made a big impact and cut down on complications. Diagnosed as a newborn, Nadir Tinsley was able to begin penicillin immediately and contiues to take the antibiotic.
“Penicillin prophalaxis has reduced the highest rate of mortality in the disease that used to be seen in the first three to five years of life,” says Dr. Ohene-Frempong, hematologist at CHOP.
While nothing has been developed to completely block complications, Hydroxyurea, a drug originally developed for cancer, has been used to treat adults, and is close to being recommended for treatment in children.
Bone marrow transplants have cured a small number of patients and Doctor Alan Flake, Director of Fetal Research at Children’s Hospital, is working on a bone marrow transplant procedure that could be done in-utero – on fetuses diagnosed with the disease. Flake’s research is seen as a “potential breakthrough” in moving towards a cure.
While there are advancements on the horizon, adequate funding from individuals and corporate sponsors is still the main issue in sickle cell disease research.
Dr. Ohene-Frempong says that sickle cell disease research has been going on at Children’s Hospital since the 1970s and it still comes down to finding enough money to move the research forward. “We are close to solving some of these problems and we need the public’s support and attention”.
Since she found out she had sickle cell disease, doctor Dejoie has focused improving the lives of patients and ending the disease – she lobbies on Capitol Hill, organizes fundraisers, researches and writes journal articles. Every day, she pushes herself to do a little more. Every day she pushes against time.
“I get sick every week, every other week, every month, says Dejoie. “But I find a way to keep moving forward. We are survivors. We are warriors.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



