How doctors are framing the flu conversation, after strain mutation
Listen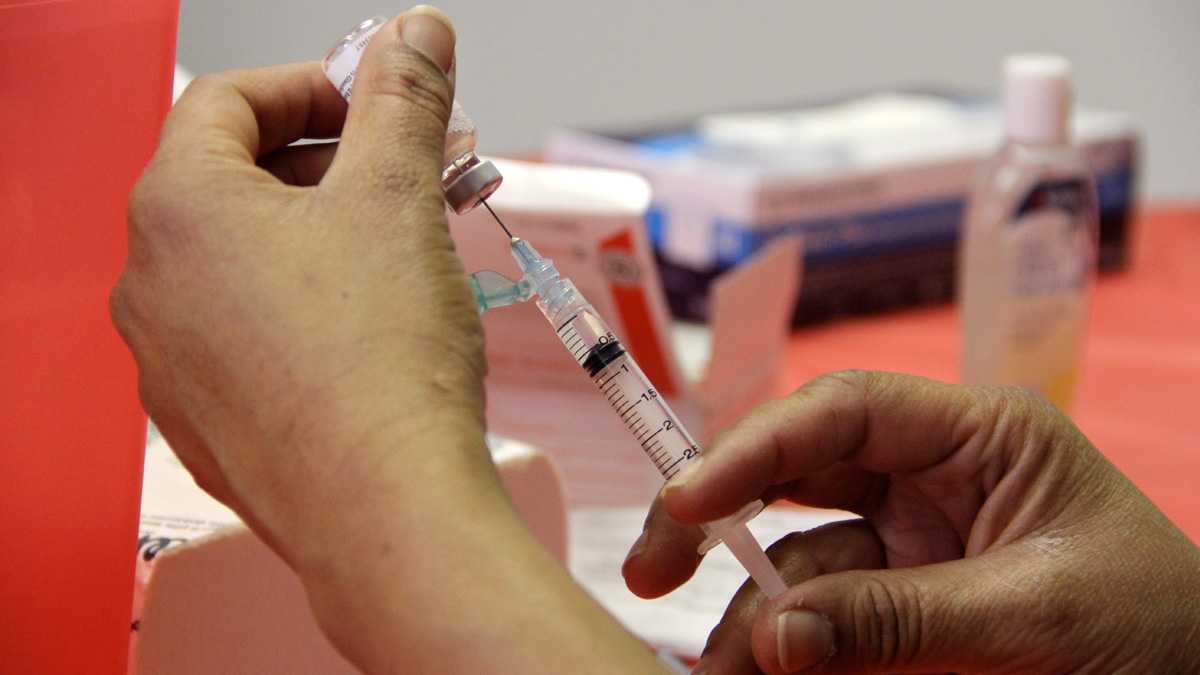
(Emma Lee
After the big announcement that this year’s flu vaccine may offer less protection than expected, some doctors are scrambling for the right way to talk about why the vaccine is still important.
But, urgent care physician Gary Kaplan says his message to patients this year hasn’t changed a lot since last year.
“So far, I haven’t gotten much pushback because I explain to them that it still offers some protection,” said Kaplan, medical director of Doctors Express in Hamilton, New Jersey.
It’s still early, but in a few weeks, the urgent care center will be on the front lines of cold and flu season.
“Flu is very serious, especially in the elderly and the very young and also in people who have chronic diseases, such as diabetes, cancer, asthma, heart disease, and patients who live in long-term care facilities,” Kaplan said.
“If you do get the shot, you are less likely to get the flu itself,” Kaplan said.
And even if you do get the flu, he said, this year’s partial protection may be enough to keep flu from becoming serious.
“You’ll recover quicker, and get back to your normal life quicker,” Kaplan said.
Vaccine scientists have one chance each year to predict which influenza strains are most likely to make us sick, and those estimates have to happen months and months in advance.
“To give you perspective, in two months we’re going to be choosing what’s going into next year’s flu vaccine,” said Scott Hensley, a vaccinologist at Philadelphia’s Wistar Institute.
He studies how the flu virus mutates, and that’s what happened this season.
The protection in this year’s vaccine is designed to fight three sub-types of flu. But one strain—H3N2–has changed. It’s morphed a little in the months since government scientists made their early prediction.
“By the time we realize the mutation has crept up, it’s too late to go back and re-make the vaccine,” Hensley said.
Complicated public health conversations
The World Health Organization and the Centers for Disease Control and Prevention usually do a pretty good job, but in the past two decades, Hensley guesses that there have been three or four years where there was a mismatch.
“Most of the time they get it right,” he said.
Here’s another thing to know about the flu vaccine: its effectiveness varies year to year.
Even in a ‘good’ year when the protection packed into the vaccine closely mirrors the flu sub-types circulating, even then, the vaccine is often only about 60 percent effective.
That reality and this year’s big mismatch pronouncement make for complicated public health conversations.
“I imagine there will be more reluctance to get the flu shot because of this news,” Hensley said. “That’s really not the right message.”
Doctors and health officials still want people to get the flu vaccine because even a less effective vaccine is the best tool we’ve got to fight influenza.
Flu can kill. Each year, across the United States, 100 children, or more, die from flu-related illness.
“It happens,” said Kristen Feemster, an infectious disease physician at The Children’s Hospital of Philadelphia.
Feemster says flu sometimes causes achiness, cough and fever that can send someone to the emergency room.
“Physicians will say they can see it in a child’s face,” Feemster said. “You can tell when flu may be the culprit. My kids have had influenza before,” she said. “There’s maybe a little bit of lack of light in their eyes. They just look tired.”
A well-funded, science-based guessing game
This year, the vaccine’s protection against the H1N1 and influenza B strains seems to be a good match. And it’s too early to know if the H3N2 sub-type that’s making most people sick right now will continue to be the big problem in coming weeks, Feemster said.
“We don’t know whether this H3N2 strain is going to be the dominant strain for the entire season,” she said.
“We’ll see what happens,” said researcher Scott Hensley. “Anyone who makes concrete predictions about flu is bound to be wrong.”
Engineering a good flu vaccine is a guessing game, although it’s a sophisticated well-funded, science-based guessing game.
Vaccines have been produced essentially the same way for the last 50 years, but scientists are looking for other strategies to defend against flu.
The next step is to move beyond annual flu predictions and build a better, universal flu vaccine, Hensley said.
Before that’s possible, he says, basic-science researchers need to understand better how the flu and immune system interact.
“Flu has a crazy high error rate,” Hensley said. “It’s constantly making mistakes. Sometimes those mistakes are beneficial for the virus.”
Those changes help the virus escape the body’s defenses against the germ. But sometimes those mistakes are bad for the virus’ own survival.
“What happens is the virus is just crippled, it can no longer enter a cell, the virus can no longer replicate, it can no longer spread from me to you,” Hensley said.
Future flu vaccines may target the parts of the virus that never change.
“We are starting to really figure where these are, to identify the Achilles heel,” Hensley said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



