Are good care and compassion lost in efforts to curb opioid prescriptions?
Listen 10:28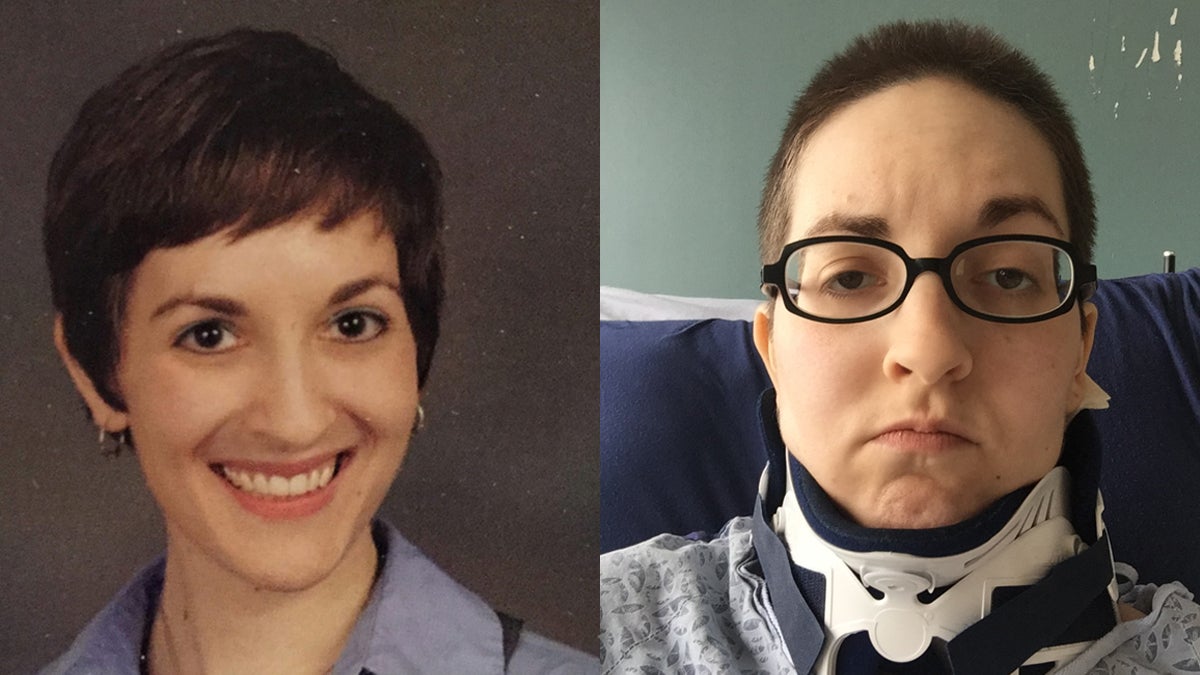
After two car accidents
“I feel like I have to re-prove myself every time I go to the doctor” — a patient and a health policy expert weigh in on America’s attempts to cut back on opioid painkillers.
Jennifer Kain Kilgore has lived with debilitating chronic pain ever since she was rear-ended in two different car accidents, which fractured her spine in four places.
“My mid-section is constrained and throbbing. Sometimes it feels like a jolt of electricity,” she says.
For over a decade, Kilgore, an attorney and patient advocate who blogs about life with chronic pain, has taken prescription opioid painkillers to relieve her pain enough to allow her to focus on her work and function in everyday life. But over time, she says, it’s become more difficult to get these medications as the climate around the use of prescription painkillers has changed.
The medical community has come under fire over the addictive power of these drugs, as the country finds itself in the midst of a heroin crisis that many attribute to years of overprescribing opioids to manage pain. Physicians and policy makers are responding with attempts to cut back on the use of the powerful painkillers. But that may leave some patients who truly need the drugs caught between competing priorities.
“The scale of the opioid problem in America has really escalated tremendously,” says David Deitz, a physician and health policy consultant. Deitz cites data from the Centers for Disease Control and Prevention showing that 259 million prescriptions for opioid pain medications were written in 2012. Meanwhile, Deitz says, “we are seeing somewhere on the order of 10,000 deaths from opioid overdose every year. Babies are born addicted to opioids because their mothers are using these drugs.”
Recently, the CDC has issued new guidelines for prescribing the drugs, and many doctors and clinics have become more restrictive in their use.
The shift has caused some problems and anxiety for patients like Kilgore.
“I feel like I have to re-prove myself every time I go to the doctor,” she says. She is no longer able to get Vicodin, which she says helped her work nine-hour days in a law practice.
When her former healthcare provider stopped prescribing the tramadol she takes for her pain, and instituted mandatory urine testing to safeguard against abuse, she decided to find a new doctor. That meant having to recount her lengthy medical history -—”about a thousand pages-plus of medical notes” — to a new doctor.
Deitz sympathizes with the position that patients like Kilgore now find themselves in, and agrees that some people will not be able to manage their pain without opioids. But, he says, “there is a very important public good that needs to be placed against this.”
He says he’s seen some positive changes in how the medical system deals with chronic pain, with doctors and insurance companies embracing treatments that can eliminate the need for opioids in some patients or greatly reduce their use. Physical therapy and psychological coping strategies using cognitive-behavioral techniques are not just “alternate” treatments to opioids, Deitz says, but proven strategies that have helped many patients.
Nevertheless, Deitz cautions that every case is different, and that opioids still play an important role in treatment for many patients.
“I think it is important to recognize that this is a nuanced issue and that there are different strategies for different folks.”
Kilgore says she understands the pressure physicians are under to stop prescribing opioids, but argues that the voices of chronic pain patients are not heard by those making changes.
“I wouldn’t wish this pain on anybody, but there are some days where I wish I could go to some legislators and say ‘Just spend 10 minutes in my body, and you’d understand why this is necessary.'”
—
Listen to the full interviews with Jennifer Kain Kilgore and David Deitz above.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.







