Nemours and Christiana hospitals open delivery unit for babies with congenital conditions
A Nemours-Christiana Care partnership creates rooms big enough to fit 2 teams of doctors, so that newborns with congenital issues stay close to their moms.
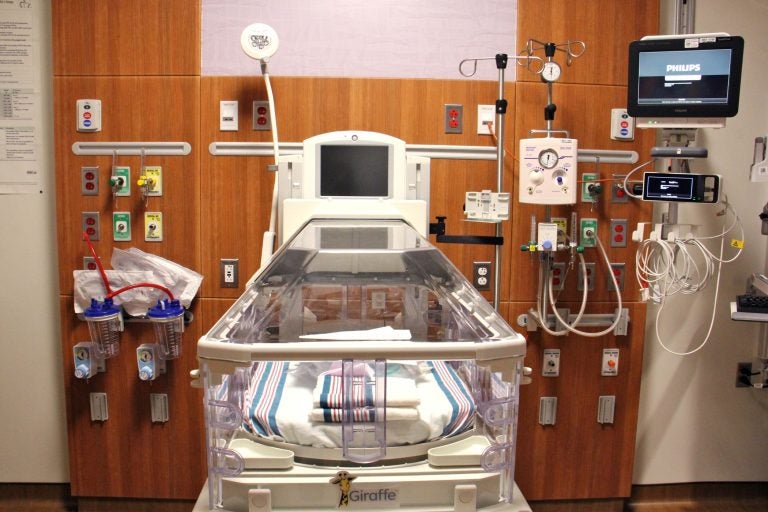
The newborn station in the labor, delivery, recovery, and postpartum rooms at Nemours is equipped to allow critically ill newborns stay with their mothers in the hours after birth. (Emma Lee/WHYY)
When Stephanie Nolasco went for an ultrasound last year to determine the gender of her baby, she was told he had some issues with his bowels. After a fetal MRI, she discovered he would be born with a condition called jejunal atresia, a birth defect that involves the partial or complete absence of the membrane that connects the small intestine to the abdominal wall.
Doctors said her son would need surgery 24 to 48 hours after birth. At the time, that meant Nolasco, who lives in Bear, Del., would deliver at her hospital, Christiana Care, and then her son would be transferred to the Nemours/Alfred I. duPont Hospital for Children a day or two later.
But a few hours after her son, Leo, was born, there was a change of plans. Doctors said he needed to be transferred immediately to undergo surgery.
Although Nolasco had given birth less than 24 hours prior, her obstetrician discharged her about a half-hour later so that she could be with her son.
“I don’t think I could have handled being away from him, knowing that he was struggling through the issues he was having,” Nolasco said. “He had to have PICC lines, and he was having surgery. To not to have been able to be there and see him before he went to surgery, it would have killed me.”
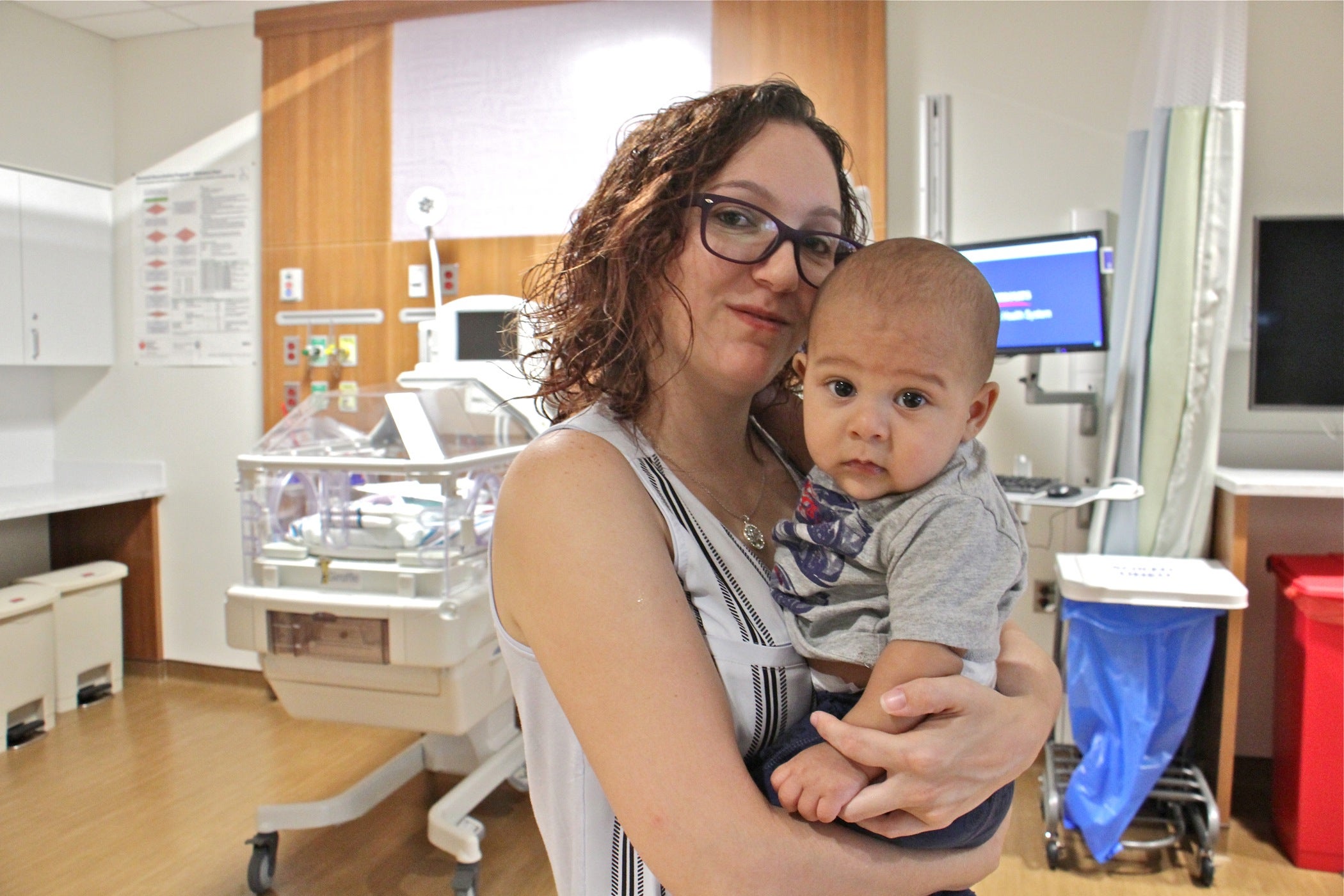
The choice took a toll on Nolasco’s body. She had to be wheeled around the neonatal intensive-care unit in a wheelchair for the first two days because she was in so much pain and hadn’t had enough postpartum recovery time.
“I’d given birth less than 24 hours ago, and now I have to navigate to the NICU,” she said. “It was hard on my body, but mentally it was the best thing.”
Now, a new partnership between Nemours and Christiana will allow women like Nolasco, whose babies are diagnosed prenatally with congenital abnormalities that require care immediately after birth, to deliver at Nemours so that the mothers and babies can stay together, without compromising the care of either.
“This enables the mom’s doctors to deliver the best care that they can, and mom doesn’t feel like she has to sacrifice to be here for the baby,” said Margaret Chou, medical director of obstetrics at the new Advanced Delivery Program.

Obstetricians from Christiana Care will deliver the babies, regardless of what practice the woman sees for her routine prenatal care, though there will be ongoing coordination and communication between the teams. The babies will be cared for by Nemours physicians.
Before the launch of the program, babies with congenital abnormalities were transferred to Nemours from other hospitals, as Leo was. Though safe, there is always a risk in transferring a patient who requires stabilization.
“Babies can change, and the needs can evolve pretty rapidly,” said Daniel Dirnberger, medical director of neonatology at Nemours. “We want them to be in that definitive care location so that we can intervene, and our surgeons can intervene right away.”
There are two specially designed rooms in the unit, both big enough to accommodate two medical teams — one for the mother, and one for the baby — without them being elbow to elbow.
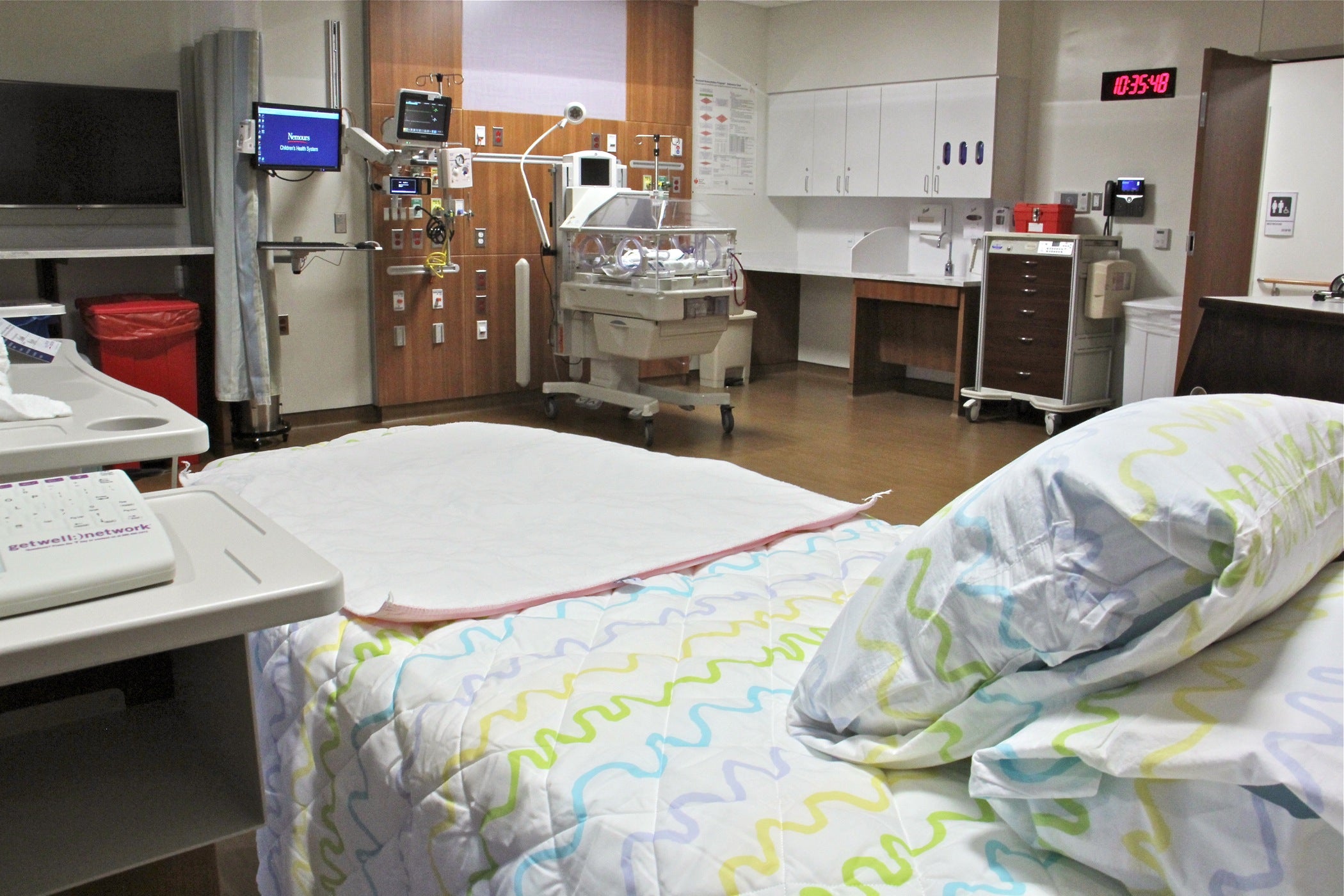
“We very thoughtfully designed this space to allow us the room and the environment to be able to provide optimal care for the mother without compromising what she needs and optimal care for the baby without compromising that space,” Dirnberger said.
The mother has a direct line of sight to her baby and can see what doctors are doing to care for her child. There are also extra-wide doors, allowing an easy and swift exit, in case the mother or baby needs immediate emergency care.
Similar programs are currently offered at Children’s Hospital of Philadelphia, but the location is nearly an hour away from someone like Nolasco.
“That can be a big challenge, particularly for our patients in Delaware,” Dirnberger said.
Christopher Beaty, nursing director for the Advanced Delivery Program, said the new unit will lead to better outcomes for everyone.
“What we’ve learned is that the seconds and the minutes matter for the outcomes of the baby,” he said. “What we also know and we’ve learned is the separation of the baby from the mom and the family can be devastating.”
Beaty estimated the program will deliver 30 to 50 cases in the first year and said the program has the option and opportunity for growth if the hospital sees the need for it.
For Nolasco’s part, she cheers the launch of the program, one she wishes had been in existence when Leo was born.
“I think that it’s going to keep families together,” she said. “I think it’s going to help babies do so much better. And I think it’s going to help prevent moms from ending up back in the hospital.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





