Many seeking detox are denied treatment because hospitals don’t test for fentanyl
Most hospital drug tests do not test for fentanyl — the cheaper, more powerful, synthetic opioid whose presence has increased in Philadelphia's illegal drug supply.
Listen 2:15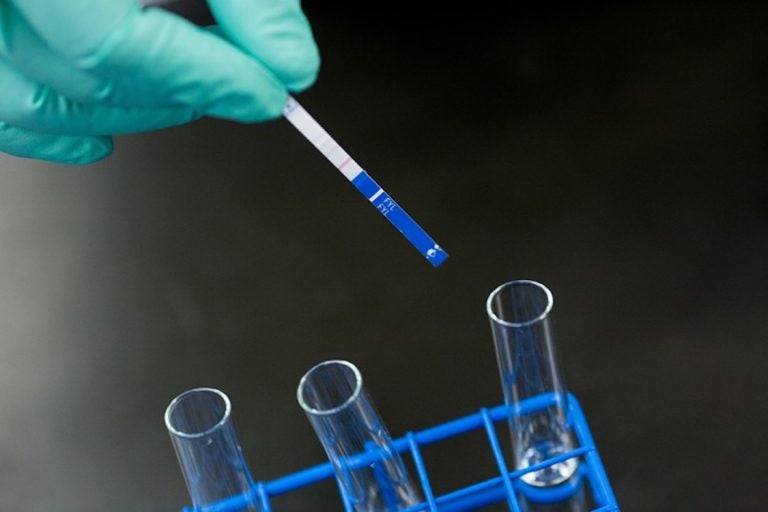
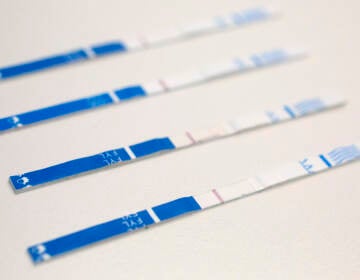
Fentanyl testing strips (JHU BLOOMBERG SCHOOL OF PUBLIC HEALTH/BLOOMBERG AMERICAN HEALTH INITIATIVE)
Julie Wolff has been struggling with an opioid addiction for 14 years. Recently, she decided she was ready to quit.
“I finally mustered up the — I don’t know if it’s strength or courage — I mustered up whatever up that word was,” she said.
Wolff, 51, became addicted to prescription painkillers while working as a nurse. She remembers the day another nurse suggested they split half a Percocet instead of dumping it down the drain.
“If there’s one moment in time that I can pause and rewind, it’s that moment,” Wolff said. “That’s how easily a life can change.”
But last week, Wolff summoned up the determination to make another change. She had a friend drive her to Friends Hospital Crisis Response Center in Frankford, near the apartment where she’s staying, and she asked to be admitted to detox. Because she anticipated painful withdrawal symptoms during the detox process, she used a little bit of heroin on her way to the hospital.
When she arrived at the crisis center, she said, health workers took a urine sample and evaluated her — and she dozed off while waiting to be admitted. Hours later, a nurse came over to tell her she was being discharged.
“She said, ‘There weren’t any opiates found in your urine.’ And I said, that’s not possible, I’ve been using every day — in fact, I used a little bit on the way here,” said Wolff, holding back tears. “I said, I know that mostly everything on the street is fentanyl — and she said, ‘We don’t test for fentanyl.’ ”
Most hospital drug tests do not test for fentanyl — the cheaper, more powerful, synthetic opioid whose presence has increased in Philadelphia’s illegal drug supply. Because fentanyl doesn’t show up in urine screenings, local hospitals and treatment centers say some seeking treatment are being denied — right at the moment they’re ready to ask for help.
Community Behavioral Health, which provides substance abuse and mental health services for the city’s 622,000 Medicaid participants, would not certify Wolff’s claim. The insurance provider later sent Wolff notification that her request for detox had been denied because it was determined that it was not medically necessary. It recommended intensive outpatient treatment instead.
“I couldn’t quite understand it,” said Wolff. “How am I going to do that without first being detoxed?”
Fentanyl undetected in urine samples
People with withdrawal symptoms — but negative urine screenings — are starting to arrive daily at the Crisis Response Center at Temple University Hospital-Episcopal Campus, said medical director Dr. Camille Paglia.
To be admitted to detox, a patient must test positive for a drug that requires detoxification — alcohol, benzodiazepines or opioids.
“Opioid or opiate withdrawal is not life-threatening, but you will wish you were dead,” said Paglia. “It’s very rough.”
But Paglia said her lab does not have the capacity to test for fentanyl — and neither do the labs at any of the city’s other crisis response centers, where patients are screened and referred for rehab or detox and third-party treatment facilities.
If someone is clearly demonstrating symptoms of withdrawal — sweating, shaking, diarrhea or vomiting, dilated pupils — Paglia said she might be able to make the case to an insurance company for detox even with a negative urine test.
“But patients frequently use just before they come here so they don’t get sick. For those patients, the insurance companies aren’t going to give them treatment,” said Paglia (who shares a name with the Philadelphia academic and social critic).
That’s what Wolff did — she used heroin, which was likely fentanyl before she went to the hospital to prevent herself from going into withdrawal while she waited. But her lack of withdrawal symptoms upon arrival actually hurt her chances of getting into detox.
Working out the kinks
Community Behavioral Health is in conversations with the city’s crisis response centers and is aware of this dynamic, said Geoffrey Neimark, chief medical officer. And he said the insurer has never officially required urine tests as a prerequisite for approving detox.
“It is considered a part of the evaluation, and, when it’s present, it helps confirm — but its absence does not disqualify or disprove,” he said.
The combination of a negative urine screening and lack of immediate withdrawal symptoms — as well as having a permanent address — could have been factors that led the insurance company to conclude that outpatient treatment would be more appropriate for Wolff.
Still, Neimark said, there are kinks to work out with the approval process to make sure everyone is getting the treatment they need when they seek it.
“We’ve heard about bumps in the road, so we’re going to remessage based on the feedback provided — because we want to be very clear,” he said.
Paglia said even if she could get the insurance approval, she worries that detox facilities themselves would still require urine tests for liability purposes. She thinks an easier, more efficient solution would be for hospitals to start testing for fentanyl.
Harm-reduction advocates use testing strips to detect fentanyl in illicit drugs before their use to gauge risk, and the strips can also test for the presence of fentanyl in urine.
According to Paglia, the strips are currently not approved for hospital use. And, because of complicated regulatory processes, Neimark said, it’s possible that fentanyl testing in-house would be easier to do outside of a hospital setting.
The outpatient option many resist
Meanwhile, Julie Wolff isn’t sure what to do. She wasn’t in withdrawal when she showed up at the hospital, but she started to feel uncomfortable as she was discharged. She began using again to prevent herself from becoming sick.
Instead of detox, Friends Hospital referred Wolff to an intensive outpatient treatment facility at the insurance company’s urging. The facility offers group meetings as well as medication-assisted treatment such as Suboxone or methadone.
Clinically, Paglia said, intensive outpatient treatment can be just as appropriate for someone who wants to stop using opioids as detox. But many resist the outpatient option.
“A lot of our patients have barriers that prevent them from going to a clinic every day, such as homelessness,” she said. “And they want to be inpatient. They want a roof over their heads, they want three meals a day. They don’t want to go to a clinic every day.”
Wolff said she knows it’s risky, but she’s considering trying to admit herself again after buying drugs that she’s confident will show up on the screening.
“My final thought is, go to a corner out here, which I hear by word of mouth on the street, and hope that it’s heroin and not fentanyl,” she said. “And hope that that day, there’s a bed available.”
Wolff’s voice quivered again.
“I’m not proud of any of this,” she said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.