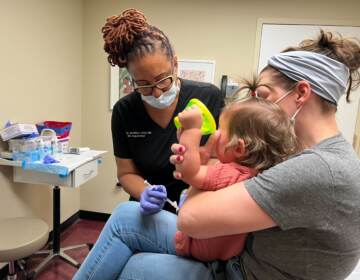
How Philly area hospitals plan to distribute the vaccine to their staffs
They’ve set up ultra-cold storage, prioritized who goes first, and created inoculation rotations so frontline workers can get shots when the doses arrive.
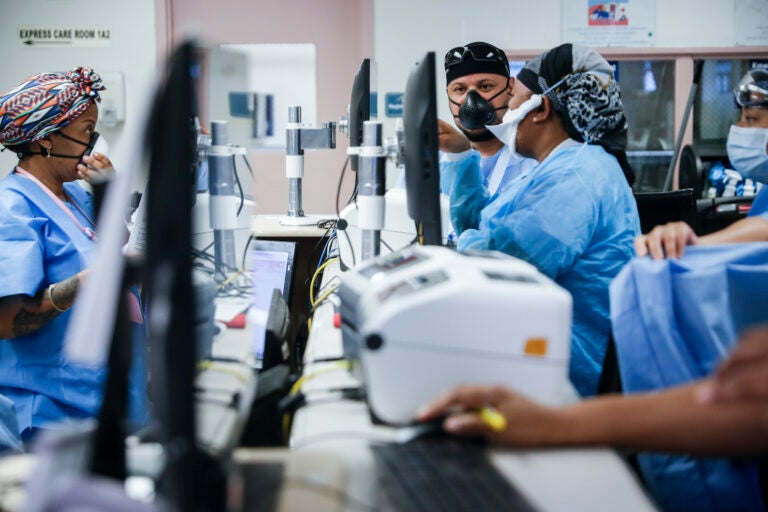
Medical personnel work in an emergency department on Wednesday, May 27, 2020. (AP Photo/John Minchillo)
Ask us about COVID-19: What questions do you have about the current surge?
Hospitals in the Philadelphia region have known their frontline workers would be first in line to receive the COVID-19 vaccine once it got the green light from the Food and Drug Administration. Until that happened, they weren’t just going to sit around and wait.
So hospitals have spent the last few weeks making arrangements — from ultra-cold storage, to prioritizing who goes first, to creating inoculation rotations so they are poised to vaccinate their workers as soon as the first round of doses arrive.
Now that the first vaccine, from Pfizer, has been endorsed by an FDA advisory panel, with emergency use authorization by the agency imminent, shipments will likely arrive in the coming days. Health systems are kicking their plans into gear, scheduling staff members to sign up for their first shots Wednesday and Thursday of next week.
The Philadelphia Department of Public Health will receive a vaccine allotment from the federal government and divvy up the number of doses to the city’s hospitals. The same will happen at the state level for hospitals outside the city. Health systems such as Einstein Medical and Jefferson Health, which have campuses in both Philadelphia and the surrounding counties, will coordinate between the city and state. While most states have released detailed plans on vaccine prioritization and distribution, Pennsylvania is one of only four that did not.
James Garrow, spokesperson for the city’s Health Department, said the number of 975-dose vaccine shipments, nicknamed “pizza boxes” for their shape, that Philadelphia would receive was still in flux.
“Every time we ask the federal government, we get a different number,” Garrow said. “They keep telling us the number will not be final until the vaccines are put onto a truck.”
With emergency use authorization likely coming soon, that should be happening any minute.
Who gets it first
No hospital expects to receive enough doses to vaccinate its entire workforce in the first shipment, so it must create tiers to prioritize its staff.
Philadelphia’s Department of Public Health has recommended that hospitals give first dibs to health care workers who have the highest risk exposure to COVID-19-positive people — but how each institution defines that is up to the individual hospital.
Einstein Medical Center expects to receive a total of four “pizza boxes” in this first round — two for its Philadelphia campus and one each for Einstein Montgomery County in East Norriton and Einstein Elkins Park. Highest priority there will go to those working in the ICU and emergency departments, including those performing aerosolizing procedures such as intubating patients. The first tier at Einstein will also include supporting roles in those areas, like security and food service personnel, as well as pharmacy workers.
Penn Medicine will also include all workers — not just doctors and nurses — in high-exposure areas in the first tier.
In the following rounds, Einstein plans to offer the vaccine to anyone in the hospital caring for COVID-19 patients, and after that, those working in outpatient settings.
In a note to staff sent Thursday, Temple University Health System president and CEO Michael A. Young noted that 3,000 of its more than 10,000 employees meet one of two high-risk categories the hospital will prioritize for the first round of vaccines: those whose work assignment puts them at risk of close contact with confirmed COVID-positive patients for more than 15 minutes, and those who work in departments where the COVID-positivity rate has been higher than 10%.
Jefferson will offer the vaccine first to clinical employees at the highest risk of COVID-19, such as those in the emergency departments, ICUs and COVID units, according to an email sent to staff Tuesday. It anticipates receiving its first batch next week in Pennsylvania and the week of Dec. 21 in New Jersey.
Though none of these hospitals plan to mandate the vaccine, their administrations encourage workers to get it.
“We strongly believe that a protected frontline provider/staff workforce honors our highest professional obligation to the safety and well-being of our patients,” wrote Temple Health CEO Young, noting that even those who have recovered from the disease should get the vaccine.
Lingering doubt
Vaccine hesitancy is high among many Americans, and that does not exclude health care workers, even those who have regular exposure to the virus.
Many hospitals have distributed surveys to find out what type of COVID-19 exposure staff members have (roles for some may have shifted during the latest case surge) and whether they want the vaccine.
At Cooper University Health Care in Camden, nearly 500 physicians out of the health system’s nearly 750 doctors responded to the survey, in which 68% said they would take the vaccine now and nearly 29% said they would wait six months to take it. Of those who preferred to wait, 95% cited safety concerns as the reason why.
Among 181 advanced practice providers surveyed, which include nurse practitioners and physician assistants, just over half said they would take the vaccine now, with more than 90% of those who said they would rather wait citing safety concerns.
The surveys were sent before the final FDA evaluation of Pfizer’s vaccine was released; since then, the vaccine has been approved by health agencies in Canada and the United Kingdom, and the FDA already released preliminary evaluation of the vaccine based on data provided by the pharmaceutical company.
In its analysis, the FDA found that the safety profile of the vaccine included “no specific safety concerns identified that would preclude issuance of an EUA,” or emergency use authorization.
The most common adverse responses reported were reactions at the injection site, fatigue, headache, muscle pain, chills, joint pain and fever. Severe adverse reactions were recorded in 0 to 4.6% of participants, and were more common after the second dose.
Stirred, not shaken
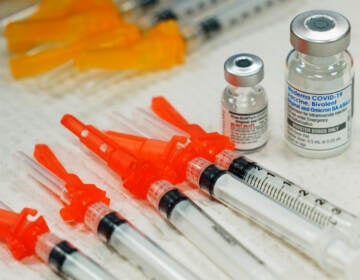
The Pfizer vaccine must be stored at -94 degrees Fahrenheit up until five days before it is administered, during which time it can be refrigerated. Hospitals have limited ultra-cold freezing capacity: Einstein has one such freezer in Montgomery County, and two in Philadelphia. Jefferson noted that it had acquired additional freezers to accommodate its expected shipments.
Each dose of the Pfizer vaccine will arrive at hospitals in two vials: a powder and a liquid. Not only does it need to be thawed before being administered, the two elements must also be reconstituted in a particular way — stirred, not shaken — before being drawn into the syringe and prepped for administration.
All that is a lot more complicated for the Pfizer vaccine than the Moderna vaccine, which requires cold storage but not ultra-cold. Moderna’s vaccine can be refrigerated for 30 days, and does not need to be reconstituted. The FDA hearing on the Moderna vaccine is scheduled for Dec. 17.
“Our pharmacists would really prefer the Moderna vaccine if we can get it, but we certainly want to get the first vaccine available and that will certainly be Pfizer,” said Steven Sivak, president of Einstein Physicians of Philadelphia and chair of the hospital’s COVID-19 vaccine task force.
Hospitals offer flu vaccines to their workers every year, so they are well-versed in the process of inoculating their staff. Einstein has a dedicated vaccine team that offers flu shots each year. At Jefferson, it’s the members of its Occupational Health Network team. Still, the logistics surrounding the COVID-19 vaccine are more cumbersome than the flu shot.
“For the flu, you just have to swipe your ID badge, roll your sleeve up and get vaccinated,” said Sivak. “This is a little more complicated.”
For the COVID-19 vaccine, employees must sign consent forms, enter their information into an electronic medical record and deliver that to the city or state health department within 24 hours to update the vaccine inventory, and wait several minutes on-site to ensure that no serious side effects ensue.
In anticipation of potential side effects, Sivak said, they plan to randomize the order of inoculations given within each tier at Einstein, so that not all the emergency department staff are vaccinated on the same day, for example. Jefferson, too, will avoid inoculating everyone from the same department on the same day.
In his letter to eligible Temple staff, Young encouraged workers to sign up to receive their vaccines on the day before a regularly scheduled day off in case of side effects.
Einstein also plans to stagger vaccinations so that when new rounds are shipped in the coming weeks, the limited number of staff administering the shots will have time to offer first doses to new workers, and not be forced on some days to only offer second doses to people who need to receive them three weeks from their first shots.
Sivak said they may even set up an every-other-day vaccination schedule from the jump. That way, he said, the already overburdened staff can have some time to catch its breath during what is bound to be a bumpy start.
“If it’s chaos on Day One, we’ll be able to recover on day two,” he said.

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)