Sarah Murnaghan has better chance for new lungs, but transplant outcomes mixed
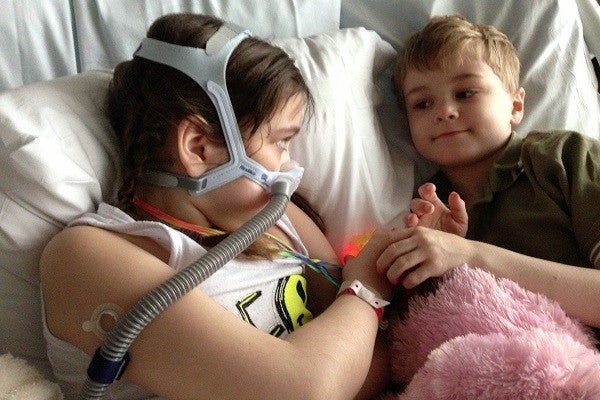
Suffering from cystic fibrosis, Sarah Murnaghan, 10, needs a lung transplant to survive.(Photo courtesy of the the Murnaghan family)
A 10-year-old girl waiting for a lung transplant at the Children’s Hospital of Philadelphia now has a top spot on the waiting list for adult lungs following a judge’s order that’s in effect until a court review next week.
Sarah Murnaghan has end-stage cystic fibrosis, a genetic lung disease. She’s been waiting for pediatric lungs for more than 18 months. Her parents successfully challenged a transplant policy requiring children 12 and younger to wait for pediatric lungs, and only be offered adult lungs after cases of adolescents and adults in need had been considered.
Experts say this gives her a much better chance of receiving donor lungs; still, transplant outcomes are mixed.
Transplant is the last resort, according to Thomas Scanlin, a pediatric pulmonologist at Robert Wood Johnson University Hospital in New Brunswick, N.J. It’s not done until the lungs of a cystic fibrosis patient are all but destroyed by the disease.
A successful transplant alleviates the disease’s symptoms, and patients no longer need oxygen or a machine to breathe, he said.
“After they heal from the surgery, their lung function is completely normal in most cases. They can take a deep breath, they have a new life,” he said.
But transplants come with problems of their own, he cautioned.
“Often, there’s a slow process of rejection of the lungs by the body,” he explained. “It can result in problems at approximately four to five years after the transplant for many patients. Not everybody — there are some who far exceed that and some who have the rejection earlier.”
Patients also are especially at risk for infections shortly after the transplant procedure.
Sarah’s case spurs review of organ allocation process
Scanlin says about 50 percent of lung transplant recipients, adults and kids, are still living five years after the transplant. He says lung transplants in kids are extremely rare — and outcomes vary slightly from transplant center to center.
Scanlin said Sarah’s case is bringing about a review of how donated organs are allocated, which he welcomed.
“It’s quite possible when a lot of transplant people get together, they will come up with a better system,” he said.
The girl’s family said that Sarah’s condition has deteriorated since the judge ruled in her favor to change the rules. A family representative said that they are still hopeful that she will receive a donor lung quickly.
Since Sarah’s wait-list status was changed by a judge, another family has filed for a similar appeal on behalf of their child, an 11-year-old boy in the intensive care unit at CHOP.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.

