American College of Physicians revises cancer screening guidelines
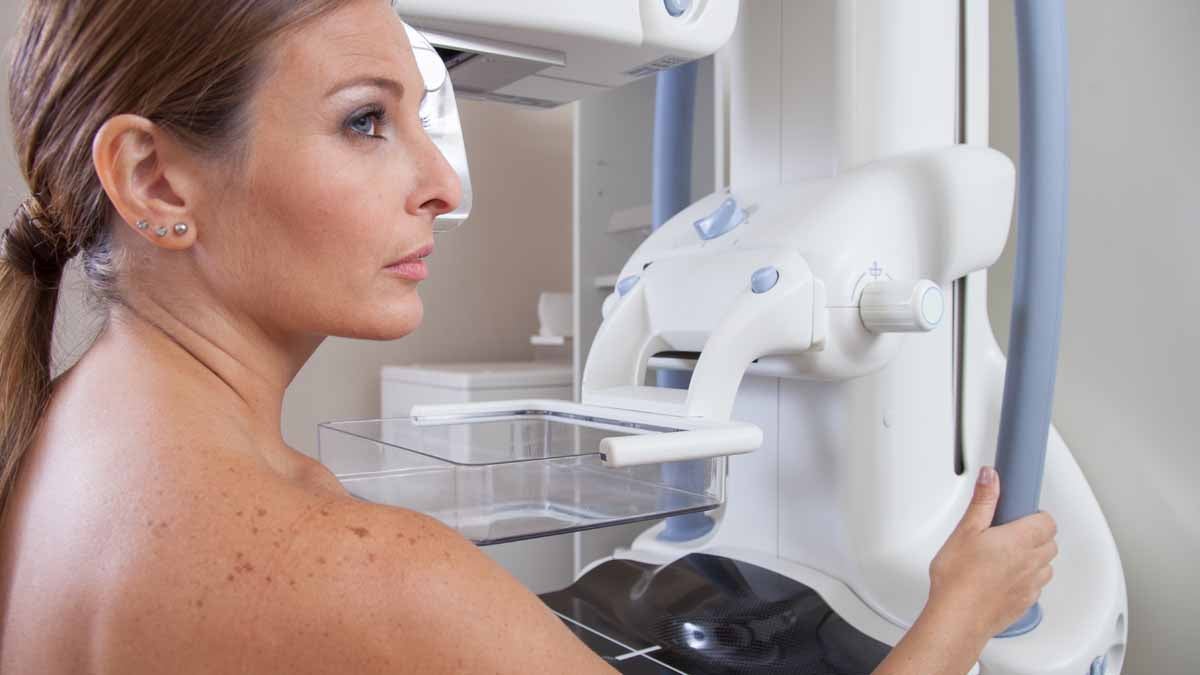 Photo via ShutterStock) " title="shutterstock_242555206" width="1" height="1" fetchpriority="high" />
Photo via ShutterStock) " title="shutterstock_242555206" width="1" height="1" fetchpriority="high" />
The American College of Physicians now recommends mammograms every other year only after the age of 40, and doing away with self-breast exams altogether.(<a href="http://www.shutterstock.com/s/mammogram/search.html?page=2&thumb_size=mosaic&inline=242555206">Photo</a> via ShutterStock)
The gains in cancer survival in the past 50 years are often attributed to better detection. But the American College of Physicians says, far too often, cancer screenings end up causing more harm than good, leading to inappropriate diagnosis and overtreatment of patients.
The doctors group has published new guidelines for how people of average risk for the five most common cancers — breast, cervical, colorectal, ovarian, and prostate — should be tested.
The recommendations may be shocking to some women, for example, who were taught to do self-breast exams and told to begin annual mammograms relatively early in adulthood. The ACP suggests considering mammograms every other year only after the age of 40, and doing away with self-breast exams altogether.
“When we start adding more tests or different modalities to it, the yield of the test may not go up,” said Tanveer Mir, a palliative care specialist at NYU and a member of the task force that analyzed the issue. “We may end up with more false-positive results.”
In addition to diagnosing someone with cancer who doesn’t actually have it, a large concern for oncologists is treating a fledgling tumor that will either not progress or never pose a risk to a patient.
According to the guidelines, men should regard PSA tests as purely optional, and only if they are between 50 and 69 years old. No one expected to live less than a decade should be screened for any of the cancers.
In reviewing specific methods, the group found that colonoscopies were useful in identifying problematic colorectal cancers, but did not need to be repeated more than every 10 years if the initial results were negative. No existing ovarian cancer screen was deemed worthwhile.
Thomas Jefferson University gynecologic oncologist Norman Rosenblum said he agreed with most of the recommendations, but not the idea that pelvic exams should go by the wayside.
“I think every woman should have a yearly pelvic examination and have a rectovaginal examination just as part of their normal health maintenance,” he said.
Mir said patients who feel strongly about getting a particular test still can — but they should talk through the pros and cons with their doctor.
“This is a discussion they can have with their physician in their office, and they can go ahead with it,” she said. “It’s not an absolute.”
The recommendations do not apply to people with family histories of these cancers, nor to those with genetic mutations that increase the chance of developing a tumor.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.

