Access to treatment for opioid addiction eased for those on Medicaid in N.J.
New Jersey is removing a barrier to medication-assisted treatment that should give Medicaid patients greater access.

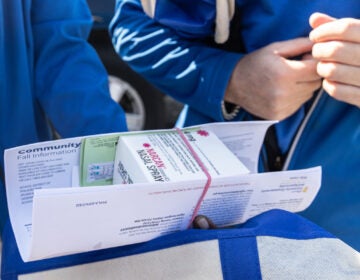
Suboxone, an oral film prescribed for the medication-assisted treatment of opioid addiction and dependency, is pictured in this Tuesday, Feb. 21, 2017 photo. (Charles Krupa/AP Photo)
This story originally appeared on NJ Spotlight.
—
New Jersey has continued to make small but critical changes in how it administers its Medicaid program to make it easier for low-income individuals to receive effective treatment for substance use disorders.
The state Department of Human Services, which oversees Medicaid, has announced that as of yesterday the program’s 1.7 million patients would no longer need the approval of a doctor in their health insurance company before starting medication-assisted treatment for opiate addiction.
Also known as MAT, the treatment involves the careful use of opioid-replacement medications to avoid withdrawal and addictive behavior and is now considered the gold standard of care. But experts have long complained about barriers that prevent patients from obtaining this treatment, including complications with insurance coverage.
In addition, in order to increase the available options, the DHS will require all addiction treatment facilities that accept Medicaid to offer MAT as an option, starting July 1. Tens of thousands of New Jersey residents now seek treatment for addiction issues each year, and many more are unable to access care.
“We’re never going to turn the tide on this epidemic unless we build a more accessible community” of treatment options, DHS commissioner Carole Johnson said earlier this year. “And we’re going all in on Medication Assisted Treatment to do it.”
All in on MAT
Johnson’s remarks came in January when Gov. Phil Murphy described his plans for spending more than $100 million in state and federal funds to address addiction. Among other things, Murphy called for the state to support two academic centers dedicated to combating opioid abuse, raising reimbursements for primary care providers who provide MAT, and funding for local addiction-response teams.
“Our goal is to remove barriers to opioid addiction treatment everywhere they exist and increase the pool of health care providers offering this critical treatment so that we can help individuals and families for whom this care is a matter of life or death,” Johnson said.
While policy changes and greater awareness have helped drive down the level of opioid prescriptions in New Jersey by some 40 percent over four years, addiction-related deaths continue to escalate. More than 3,000 residents died as a result of drugs in 2018, and the growing presence of fentanyl — a powerful opioid substitute that is increasingly being mixed with heroin — continues to drive up mortality.
Policymakers have struggled to find ways to expand the network of treatment options, something that can be a challenge when there are more glamorous, better-paying clinical specialties for doctors to choose. Another barrier has been convincing health insurance plans to pay for these treatments without erecting hurdles, such as prior authorization, requiring a medical expert at the patient’s health insurance company to approve the coverage for a treatment plan developed by a patient’s doctor.
At an NJ Spotlight panel on addiction last year, Johnson and others acknowledged that Medicaid members have faced particular difficulties finding providers who accept their plans and offer MAT for substance use issues. Many end up in hospital emergency rooms that are often ill-equipped to properly address addictions.
Prior authorization has been a roadblock
And even when individuals did find an available provider, Medicaid’s use of prior authorization often delayed patients’ access to treatment, participants in the panel noted. “When someone with an opioid addiction is ready for treatment, we shouldn’t be losing them to care while they wait for approval,” Johnson said Monday.
Under the new policy, Medicaid members in New Jersey can receive MAT as soon as a doctor prescribes the regime, the DHS said. Johnson praised the insurance companies that offer Medicaid plans — Aetna, Amerigroup, Horizon Blue Cross Blue Shield, UnitedHealthcare and WellCare — for working to implement these changes quickly, and said she hoped it would provide a “meaningful difference in terms of timely access to care.”
Prior authorization requirements have also proved frustrating for providers, some of whom said they had to dedicate specific staff to chasing down these approvals. The DHS is hoping that eliminating this requirement will also encourage more clinicians to get involved with MAT, which might now require less time and paperwork.
“New Jersey’s Medicaid program is a valuable tool in the fight against the opioid epidemic,” added DHS deputy commissioner Sarah Adelman. “With this change, we are easing burdens and removing barriers to care to help increase treatment and prevent overdose. Our goal is to save lives.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.