Living with a surprise diagnosis of ‘iron overload disorder’
Listen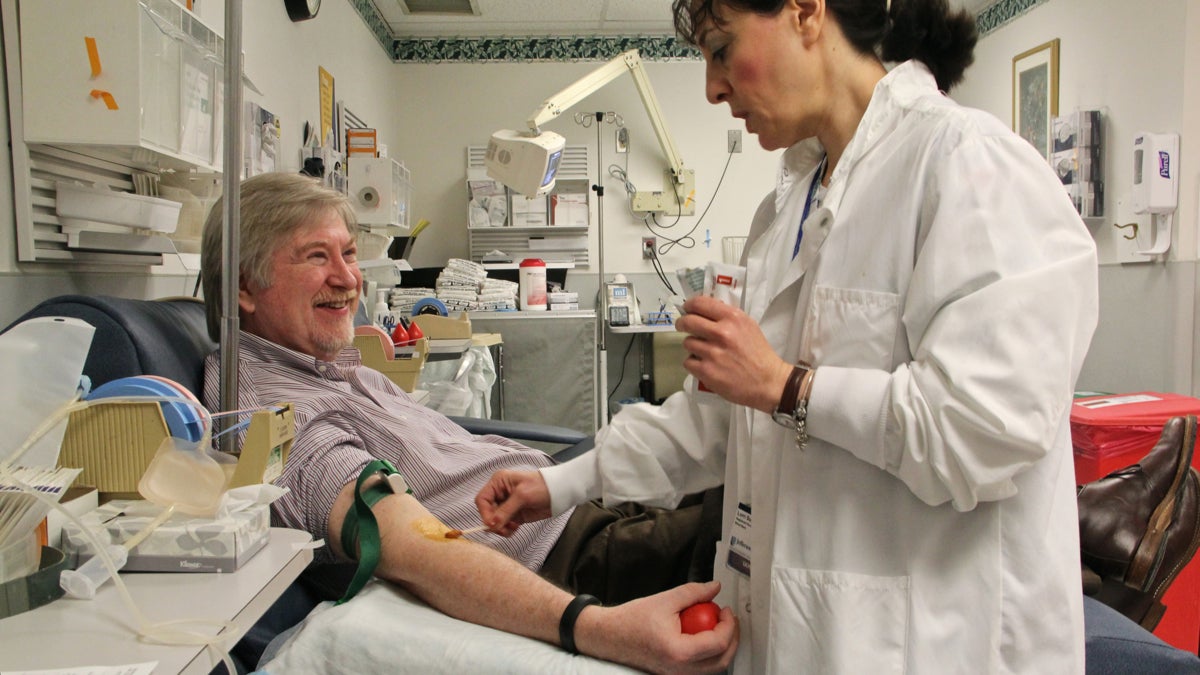
Charge nurse Lorri Summers prepares Dr. Craig Hooper for his weekly blood draw at Jefferson blood clinic. (Emma Lee/for NewsWorks)
Iron. Your body needs it to carry oxygen throughout the body in red blood cells. But too much of it can be toxic.
Craig Hooper, a professor at Thomas Jefferson University, was recently diagnosed with hereditary hemochromatosis.
“If it’s not diagnosed, you usually show up with congestive heart failure, cirrhosis, [or] type 2 diabetes,” said Hooper.
Hemochromatosis is a disease in which too much iron builds up in your body. While iron is essential in human bodies for carrying oxygen, too much can be poisonous. In the United States, more than one million people suffer from hereditary hemochromatosis, which is also known as “iron overload disorder.” It’s one of the most common genetic disorders but it’s likely that you’ve never heard of it.
Hooper first got a sign that something was wrong about three years ago.
“My liver enzymes were up a little bit in my annual physical and my primary care physician wasn’t too worried about it,” he said. But the trend continued each year.
Liver enzymes could indicate a number of possible diseases, including alcoholism, and Hooper credits an open-minded primary care physician for looking deeper into his symptoms.
“We sent out a panel to look at Hepatitis and they look for different parameters, one of which is ferritin.” Ferritin is a protein that binds to iron. Doctors use ferritin testing as a benchmark for how much iron is stored in the body.
The test confirmed that something was wrong. “My ferritin levels came back about 10 times normal,” Hooper said.
Genetic testing sealed the deal. Hooper had a hereditary disorder that caused his body to absorb iron from food more easily than normal. Since the body doesn’t have a way to flush out the iron, it builds up in organs and extremities over time, and can impede organ function when the iron reaches critical levels.
However, many people never know that they have this disorder.
“It’s been building up since I was born,” said Hooper. “More recently, I had some other little problems that I thought were aging and probably were not. It was probably iron accumulation.”
Weekly blood draws
The body has no natural mechanism for filtering iron, so the treatment is simple: bleed it out. Every week, Hooper gets a pint of blood taken with the goal of lowering his iron levels to a normal range in six months.
“It’s the old days of leaches and barbers as clinicians,” said Hooper, referencing earlier medical practices of blood-letting.
At the Jefferson Blood Donor Center, Nurse Sommers takes care of Hooper’s treatment while daytime television plays in the background. “He can be kind of a tricky stick,” said Sommers.
“Physiologically, it’s hard to get bled on a weekly basis,” said Hooper. He said losing blood dramatically changes blood pressure, and can make quick changes from sitting to standing, disorienting. It also impacts overall energy levels. “There are times when you absolutely run out of energy in a way that you’re not used to. It’s like a battery running out,” he said.
Hooper, who conducts research at Jefferson University, was not the only one knocked sideways by his diagnosis. “What has surprised me is that many of my colleagues, clinical colleagues, had never heard of it,” said Hooper. “This particular gene, that I have, is present in one copy in about one out of every 200 individuals that originated in northwestern Europe. Ireland, Scotland, England, France, also. In some areas of Ireland, one out of every five people have the gene.”
Adjusting to a new diet regimen
In addition to draining iron out of his body, Hooper now has to be careful about how much he puts in his body in the first place. “What has bothered me is it’s been very very difficult to find foods that are actually low in iron,” said Hooper. “The first thing you do is give up on red meat.”
Fortified foods, like bread and cereal, provide another challenge. “I found out I was eating a type of cereal that was 90 percent of the daily iron dose, and the daily dose on the packaging was based on what women need.” Women need to consume more iron to maintain healthy levels because they lose blood during menstruation.
And, Hooper says, his regimen of getting blood drawn and eating differently is working.
“I would say after the third phlebotomy [blood-letting] session, I started to actually feel different, feel better” he said, adding that since the iron accumulated so gradually, Hooper couldn’t tell how much it was affecting him. “I have more energy now and everybody notices it. My students notice it because I chase them around the lab. So the downhill slide was not as dramatic as the recovery.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



