Philly jails to spend $9 million on hepatitis C treatment
The Philadelphia Department of Prisons has quietly started testing all inmates with hep C and curing those who stay long enough to complete treatment.
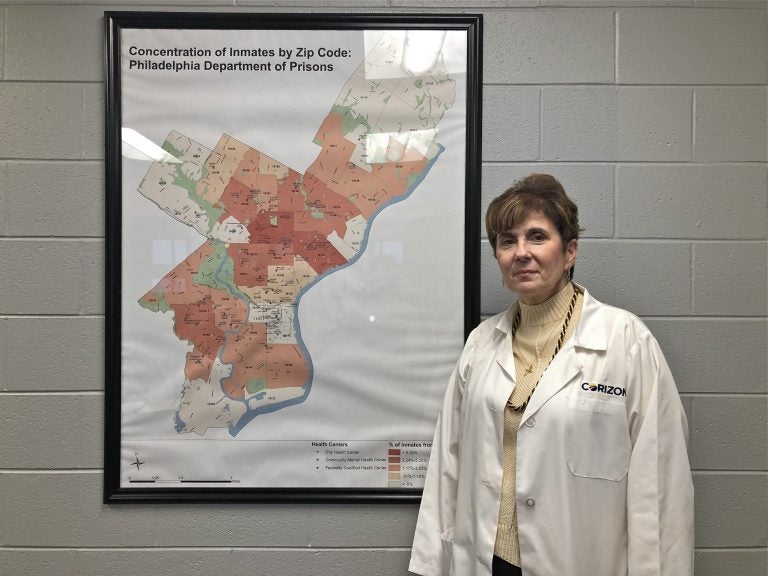
Debra D'Aquilante, an infectious disease specialist at Corizon Health, is heading the new hepatitis C treatment effort at the Philadelphia Department of Prisons. (Nina Feldman/WHYY)
The Philadelphia Department of Prisons has started testing all inmates for hepatitis C and treating those who will be incarcerated long enough to be cured. Officials at the jail estimate they will cure 700 people in the course of a year, costing $9 million in city funds.
The move comes on the heels of a settlement resulting from a 2018 class-action lawsuit in which the Pennsylvania Department of Corrections agreed to provide hepatitis C treatment to inmates. Philadelphia civil rights attorney David Rudovsky litigated the suit on behalf of the inmates and built a case that hepatitis C needed to be treated at all stages, not just the more advanced ones because it can cause difficult health issues even early on. Plus, the longer someone has the viral infection, the harder it is to treat.
The argument also centered on the opportunity to treat inmates from a public health standpoint: Hepatitis C can be cured, and if patients are treated while incarcerated, they can’t infect other people when released.
As a result of the settlement, the state Corrections Department started offering treatment to all inmates with hepatitis C last year. It is required to offer treatment to 1,500 inmates in the first year and 1,500 in the second, statewide.
The settlement set a precedent. Rudovsky approached the city and said if the jails didn’t do the same thing, legal action would be brought.
“From the beginning, they said, look, we understand that it’s worth it from a public health standpoint,” Rudovsky said of city officials. “The response early on was just, this is a significant cost.”
Not only is it expensive, but it’s also harder to treat hepatitis C at a jail than at a prison, because inmates stay in jail for a shorter and often unpredictable period, making the four months necessary to complete treatment tricky to guarantee. But jail officials were eager to comply with the new standard of care. They signed on to a legal agreement with the Pennsylvania Institutional Law Project, which set guidelines for the inmates’ treatment.
Rudovsky said Philadelphia’s jail system is the only one he knows of nationwide testing and treating hepatitis C on this scale.
What’s involved
Treatment for hepatitis C has improved substantially in recent years. Before the development of the direct-acting antiviral drugs used now, treatment took months, was unlikely to work, and came with a slew of unpleasant side effects including anxiety, depression and flu-like symptoms.
Harvoni, the first single-tablet direct-acting antiviral, came out in 2014 and cost nearly $100,000 for a course of treatment. Now, if continued for the full 12-week course of treatment, drugs for hepatitis C are nearly 100% effective, with little to no side effects. Market competition has driven prices down, too — with a discount the jails get through the federal government, a full course of treatment costs $25,980 a person.
The city has allocated $14 million to the jails to treat hepatitis C patients this year — more than the amount earmarked for the state settlement last year. Jail officials said they think it will actually be less expensive because drug costs have gone down.
Hepatitis C is a blood-borne virus that infects the liver. It is most commonly spread through injection drug use. It can be acute or chronic, and in either case, people who have it rarely show symptoms. Left untreated, the virus can cause lasting liver damage, cirrhosis, liver cancer, and death. Roughly 50,000 people have hepatitis C in Philadelphia, and more than 3 million nationwide. Jail officials in Philadelphia estimate roughly 10% of the incarcerated population has hepatitis C.
At the Philly jails, a blood test for hepatitis C has been added to the standard panel of labs that inmates receive during intake. It takes a couple of days to get the results back, and because it’s common for people to be bailed out quickly, many never see the results.
Debra D’Aquilante, an infectious-disease doctor with Corizon Health, the jails’ health care provider, gets a list of those who test positive that do stay long enough. Assuming they want treatment, D’Aquilante will order more tests to determine how far along their disease is, and get a sense of how long they’ll be incarcerated to determine whether they’re eligible for treatment.
“It’s so different here than a state or federal prison, where every provider knows their patient will be there for that 12 weeks,” said D’Aquilante.
The jails started treating inmates at the beginning of September. D’Aquilante estimated that since then she’s treated 10 people a week, and twice that number have tested positive but left too early to be eligible for treatment.
If treatment is interrupted midway, the virus can return and become treatment-resistant.
That’s why the jails have partnered with community health nonprofit Philadelphia FIGHT. Case managers there have started visiting the jails each day to meet with inmates who test positive, talk to them about their illness, and make sure they know where to go to continue treatment if they get out unexpectedly early. Follow-up care is important: Even those who complete treatment have to be tested three months after they’re finished to make sure their viral load is zero. Those with advanced hepatitis C need to go for regular follow-up visits to screen for liver cancer.
D’Aquilante said the coordination between Philly Fight and the jails is going smoothly.
“I have a tight rein on my list,” she said. “I’ll see that someone got out, and I’ll say, oh boy, he’s on medicine, let me call.”
What happens after jail
Hep C treatment is covered by Pennsylvania’s Medical Assistance program, so when a patient switches from the jail to Philly FIGHT, the two split the cost.
Stacey Trooskin, director of viral hepatitis programs at Philadelphia FIGHT, said working with correctional facilities is essential in the effort to eliminate hepatitis C. Her organization is seeing a new wave of young people with hepatitis C, many of whom inject opioids but are otherwise healthy and don’t engage in medical care often.
“Because drug use is criminalized in our country, the correctional system is often one of the only places that individuals may have access to continuous health care,” she said.
Bruce Herdman, medical director for the Philadelphia Department of Prisons, sees it as his responsibility to treat the epidemic as the head of what amounts to the only public hospital in the city.
“From a public health standpoint, we can help prevent a lot of infection by getting people treated before they leave,” Herdman said. “If they leave and they’re cured, they’re not going to infect someone else.”
Though the price tag for treatment is high, studies have shown that treating hepatitis C can reduce costs in the long run — especially since a cure is now possible. Not only will curing people reduce the number of subsequent individuals who contract the disease and require treatment, it will reduce the cost of health care for those whose disease would worsen without treatment.
If hep C goes untreated, a certain percentage will go on to develop end-stage liver disease, require transplants, and multiple hospitalizations, said Trooskin.
“And those health care costs are extraordinary,” she said.
—
This article was updated to correct Stacey Trooskin’s job title.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





