CDC urges more teens to have HPV shots as N.J. lags national rate
Some parents think the vaccinations may encourage kids to have sex, doctor says.
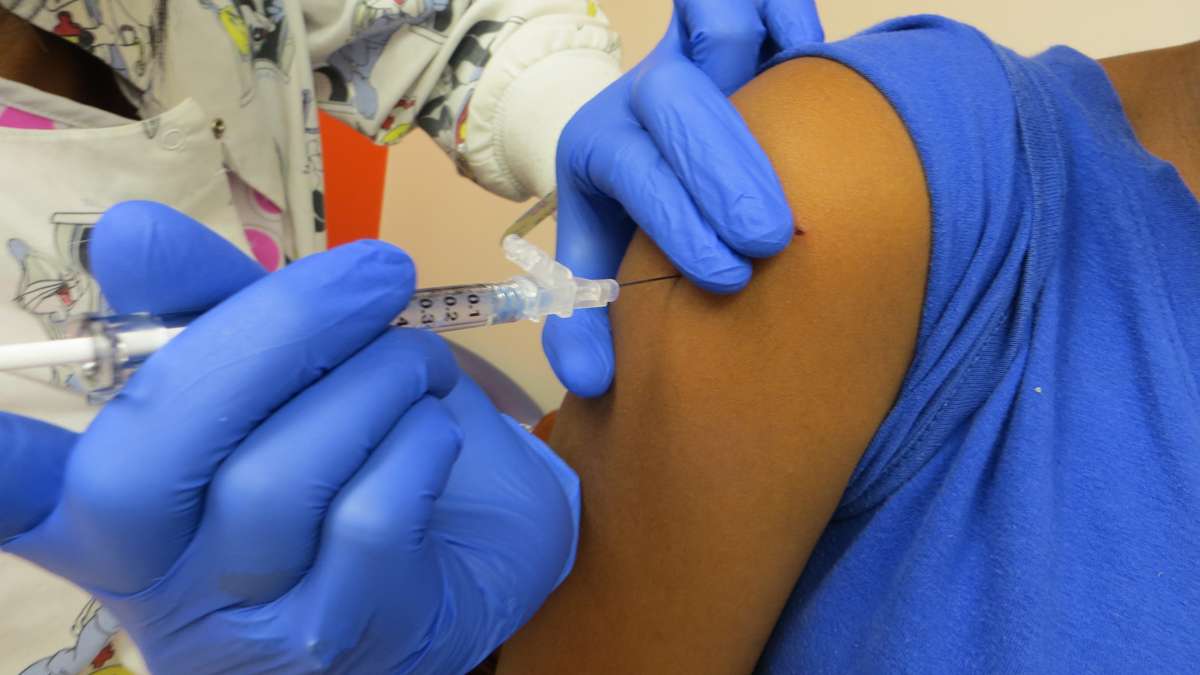
The Centers for Disease Control and Prevention recommends the vaccine against the Human papillomavirus for girls and boys age 10 or 26. (Taunya English/WHYY)
More than half of New Jersey 13- to 15-year-olds aren’t completing vaccinations for HPV, leaving them potentially exposed to the sexually transmitted infection (STI) that can cause cancer, according to data from state health officials who are stepping up their efforts to reverse the trend.
The Human Papilloma Virus is the most common STI, affecting 79 million Americans, mostly in their late teens and early 20s, according to the federal Centers for Disease Control and Prevention.
While most infections don’t develop symptoms, and go away on their own, some result in genital warts or cancer of the cervix or the throat, the CDC says.
Such health problems can be prevented with HPV vaccination but more than 60 percent of 13- to 15-year-olds in New Jersey aren’t fully protected, according to the Department of Health data.
How N.J. lags in vaccinations
The data show that only 39.1 percent of teens in that age bracket completed the multi-shot HPV vaccination process in 2017, the latest year for which data are available. That’s down from 42.7 percent in 2016, and below the most recent national rate of 46.0 percent.
Although first-dose HPV vaccination increased for both boys and girls in 2017, the rates lagged significantly behind two other routine adolescent vaccinations — Tdap and meningococcal conjugate, the department said.
Among patients of all ages, it said New Jersey saw about 1,900 cases a year of HPV-related cancer in 2012-2016. The most common kinds of HPV-related cancer are of the cervix for women and of the mouth and throat for men, DOH data show.
While vaccination rates for 13- to 15-year-olds have risen since 2011, they are still well below the 80-percent level that the state aims to achieve by 2020.
Doctors and health officials are renewing their drive to get more young people vaccinated — as early as age 10, when scientists say the vaccine can be most effective, and as late as age 26.
Unfounded fears, misplaced beliefs
Dr. Ruth Schulze, a gynecologist who has been practicing in northern New Jersey since 1987, said the drive for more use of the HPV vaccine is hindered by unfounded fears of vaccinations in general.
“We seem to be in a bit of a cultural dilemma in that we are fearful of vaccinations,” Schulze said. “It’s problematic because they are a very safe vehicle in which to prevent subsequent disease.”
The relatively low rate of HPV vaccination for 13- to 15-year-olds may also reflect parents’ reluctance to agree to a shot that looks like it allows them to have sex with impunity, Schulze said.
“They are thinking, ‘We are going to give you something that will protect you from viruses that you may acquire during sexual activity,’” she said.
While many parents may wish to discourage young teenagers from becoming sexually active, it will happen regardless of whether the children are vaccinated or not, and so the parents should agree to their kids getting the HPV shots, Schulze said.
“Whether they are vaccinated or not vaccinated, it won’t stop them from being sexually active, regardless of what their parents may think,” she said.
What to tell teenagers
Parents should tell their kids that the vaccine is designed to prevent disease and not to encourage sexual activity, she said.
“Parents need to present to the child: ‘I’m giving you a vaccine, much like I gave you vaccines when you were younger to protect you from chicken pox, if and when you got exposed.’
“It isn’t, ‘You’re getting vaccinated so now you can go ahead and do something. This is getting a vaccine to get protection so that if and when you are exposed you already have antibodies on board to help you,’” she said.
Dr. Tina Tan, the state epidemiologist, also said some parents may resist giving permission for the shot because they think their children are not sexually active, or because they believe the vaccine is not safe.
Tan also cited a CDC study from 2013 indicating that not all doctors recommend the vaccination. “The provider recommendation is the best predictor of patients receiving the vaccine,” Tan said.
But Schulze rejected the suggestion that there was any reluctance by doctors to use the HPV vaccine. “I can’t really believe that currently practicing pediatricians who do vaccines all the time are not nailing this as part of their routine discussion,” she said.
Educating parents and teens
Although there is no guarantee that the vaccination will prevent infection in all individuals, there is good evidence that vaccinated people are much less likely to show symptoms of HPV-related illnesses than those who have not been vaccinated, Tan said.
She cited CDC data from 2003-2006 showing that for oral HPV infections, there were 88 percent fewer cases among people who were vaccinated than among those who were not.
To encourage more young people to get the shots, officials are focusing on educating them and their parents, especially through social media, Tan said.
One solution, she said, is to “bundle” HPV shots with other vaccinations such as Tdap and meningococcal conjugate, an approach fostered by “Protect Me With 3+,” an annual poster and video contest run by DOH and two health partners to raise awareness of the importance of adolescent immunizations.
And she urged parents to begin HPV shots as early as 10 because there is a better antibody response among younger children, and because they are unlikely to be sexually active at that age.
For her part, Schulze urged healthcare providers and officials to use all available media to promote the vaccine, and she called on doctors to help patients overcome their fears.
Physicians should be asking patients: ‘What is worrisome to you? Let me try to allay your fears,’” she said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.