Cooper Health specialist: Time to treat opioid addiction like a disease — with medicine
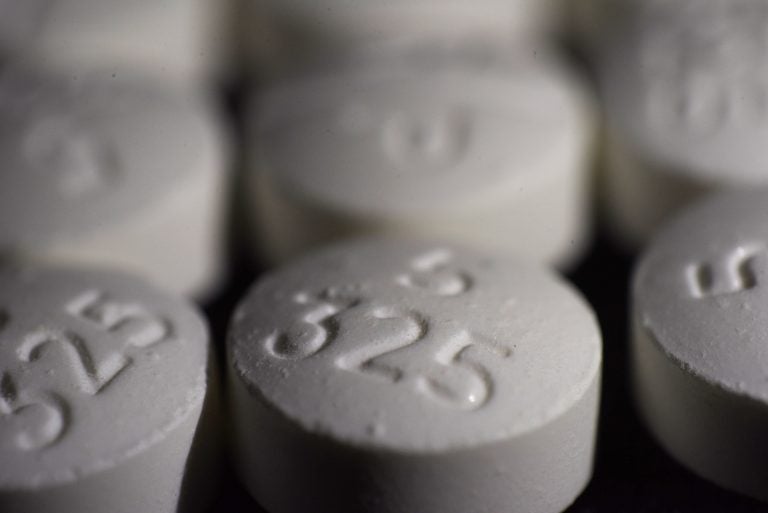
This photo shows an arrangement of pills of the opioid oxycodone-acetaminophen in New York. (Patrick Sison/AP Photo)
“Opioid epidemic.” The phrase has become ingrained in American public discourse, at candidate debates and community meetings, and in policy statements.
As it becomes clear that opioid-related overdoses have touched every level of society, the quest for a solution is drawing bipartisan support at the state and national level.
The most recent update from the National Center for Health Statistics estimates that 64,000 people died in the United States from drug overdoses in 2016. The vast majority, around 50,000 of those deaths, came from opioid related drugs.
- In Delaware 309 people died from drug overdoses, which was a staggering 71 percent increase over 2015.
- In Pennsylvania 4642 people died from overdoses.
- In New Jersey it’s estimated that 1900 people died from overdoses.
If we really want to help reverse this epidemic, said Dr. Kaitlan Baston at Cooper University Hospital in Camden says, we need to use opioid-based medicines to treat opioid-related addictions.
Methadone and buprenorphine-based treatments such as Suboxone are the best option for many fighting addiction, Baston said, but many see the approach as simply trading one drug for another — and that stigma is preventing its wider adoption.
As a result, programs based on total abstinence remain popular, although Baston said they are not always the best option for the patient. And methadone clinics remain deeply unpopular. Throughout the state, neighbors have fought to keep clinics out of their communities.
In November, for example, hundreds crowded a Camden City planning board meeting to express concerns about a proposal to bring an out-patient facility to the Waterfront South neighborhood.
Changing public perception
As part of a growing chorus, Baston wants to convince more people that, if handled correctly, opioid-based treatments are part of the solution, not the problem. In September, Food and Drug Administration Commissioner Scott Gottlieb called for wider adoption of medication-assisted treatment that includes opioid-based medicines.
Baston said the record is clear: If a patient who has overdosed on heroin starts a regular treatment program — including methadone or another opioid substitute — there is a much better chance that patient will be alive a year later.
Someone using methadone will not have withdrawal symptoms and, according to Baston, will not feel the effects of heroin or another opioid if they do ingest the drug, which helps in reducing the desire for a fix.
At Cooper’s emergency department, the staff sees five to 20 heroin overdoses a night. According to Baston, the best chance for each of those patients would be immediately starting treatment, including medications such as methadone, buprenorphine or naltrexone — drugs that flood the same dopamine receptors as heroin.
Barrier to treatment
Doctors can’t begin an opioid-replacement regimen unless the patient is in a program such as the one Baston has established at Cooper — and finding an opening in such a program takes time.
“I have nowhere near the number of slots available to get those medicines to the number of people that need them,” she said.
As with everything to do with addiction treatment, the need far outweighs available resources.
“That’s why I have a 300-patient waiting list right now,” she said. Patients on that list who might benefit from methadone-based treatment “are really likely to overdose and die.”
Where it begins
Most of Baston’s patients became hooked on opioids after receiving a prescription for pain medication. As the addiction takes hold, they need to increase their dosage. But as it becomes more difficult and expensive to obtain the prescriptions, in most cases, she said, they transitioned to heroin, which is far cheaper and easier to obtain. A single bag costs about $10.
“It’s a story I hear a hundred times a day,” Baston said. “There are very few patients who go out and just use heroin.”
Some patients will need to be admitted to the hospital, but she’s seen others make huge strides with regular outpatient visits. In an outpatient setting, she said, her patients can get a daily dose of methadone, buprenorphine or other medication.
Many patients want to keep coming back, Baston said, because that means another day they won’t slip. In the long term, they can begin to return to normal lives, get to work, repair relationships with loved ones, drive. They can live.
“Studies show that the longer people take these medicines, the more likely they are to stay in recovery,” she said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.