Campaign pushing Pa. to cover unauthorized children through state health insurance
Advocate says change can be accomplished simply: Remove 13 words in the current CHIP statute that exclude undocumented kids from eligibility.
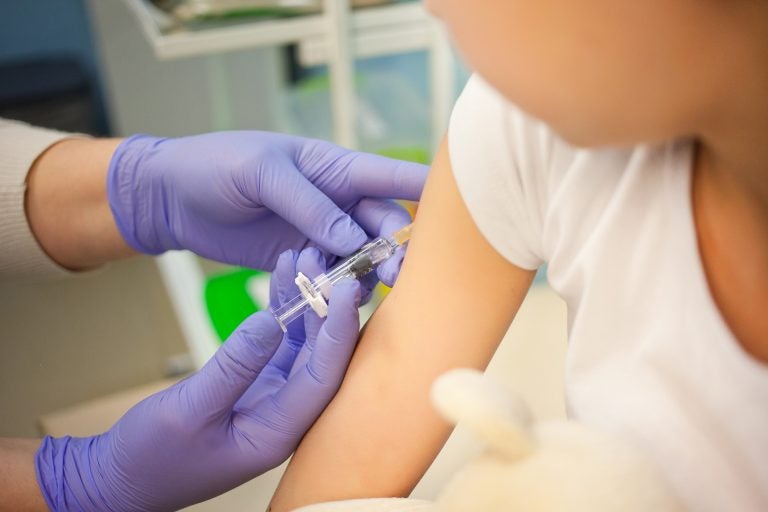
(AnnaVelfoto/BigStock)
In 2007, lawmakers significantly expanded Pennsylvania’s Children’s Health Insurance Program statute to reduce the number of uninsured children across the state.
Dubbed “Cover All Kids,” the initiative raised the income threshold to qualify for CHIP so that no family could make too much money to be eligible. Despite the name, however, the measure excluded a sizeable chunk of children from coverage — the thousands of kids across the state who don’t qualify because of their immigration status.
Now, another campaign, the Dream Care Initiative, is hoping to change that.
An estimated 24,000 children in Pennsylvania are undocumented and lack health insurance coverage — with about 7,000 uninsured Hispanic children in Southeastern Pennsylvania, according to Public Citizens for Children and Youth or PCCY, an advocacy group pushing the Dream Care Initiative. The rate of uninsured Hispanic children in Pennsylvania is 7.4 percent — higher than the national average — and may be due to their immigration status.
Urban clinics and federally qualified community health centers treat many undocumented children, regardless of immigration status, and clinicians there are able to refer patients to specialists in emergency situations. But the real issue comes for children with chronic conditions, such as epilepsy, broken bones, or heart conditions that wouldn’t classify as emergencies, but are serious and require ongoing care, said Dr. Kate Yun at the Children’s Hospital of Philadelphia.
“It’s not always easy if you don’t have health insurance to be able to afford the cost of specialty care,” said Yun. “Think about things like an MRI or a CAT scan — that can be out of reach for a lot of families.”
When undocumented children do visit an emergency room in Pennsylvania, the state foots the bill — and it’s high. PCCY found that it cost $4,600 for a pediatric hospital in Pennsylvania to treat an uninsured patient, while it would cost an average $2,500 to enroll that child in CHIP. (The average is calculated by looking at costs where undocumented children are covered by state-funded insurance: California, New York, Washington, Illinois, Oregon, and Washington, D.C. )
In addition to her CHOP practice, Yun works at Puentes de Salud, a community health clinic in Philadelphia that treats immigrant families, many of them undocumented. While most of her CHOP patients are insured or paying out of pocket, most of the children Yun sees at the clinic are not. The consequences, she said, can be devastating.
“A simple example is a child who hasn’t had health insurance and who’s had an injury to their ear drum,” Yun said. “Often that can be repaired surgically, but, if you don’t have health insurance, that surgery is out of reach.”
Yun said she has seen a patient who has lost hearing as a result.
In the case of her patients who start experiencing seizures, she said many parents can’t pay for a neurologist to prescribe the proper medications.
“You can imagine that’s really scary and also really dangerous for that child and that family,” said Yun.
Colleen McCauley from PCCY said the solution is easy: Just remove 13 words in the current CHIP statute that exclude undocumented children from eligibility. She said she and her group have been talking to legislators — including state Reps. Jamie Santora and Alex Charlton of Delaware County — to make a case for the Dream Care Initiative.
Despite political stalemates on a national level over the Deferred Action for Childhood Arrivals or DACA program — which temporarily allows young immigrants living in the country illegally who were brought here as children to live and work in the U.S. — McCauley said she’s found bipartisan support for the change on a local level based not only on its projected cost savings, but also on its appeal as a public health issue.
“All kids in the classroom need to stay healthy so they can help ensure that their classmates stay healthy,” said McCauley.
Changing the statute’s language can be done as part of the budget process, but time is running out. The legislature is required to pass a budget by July 1.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





