Access to primary care in Philly varies greatly by neighborhood
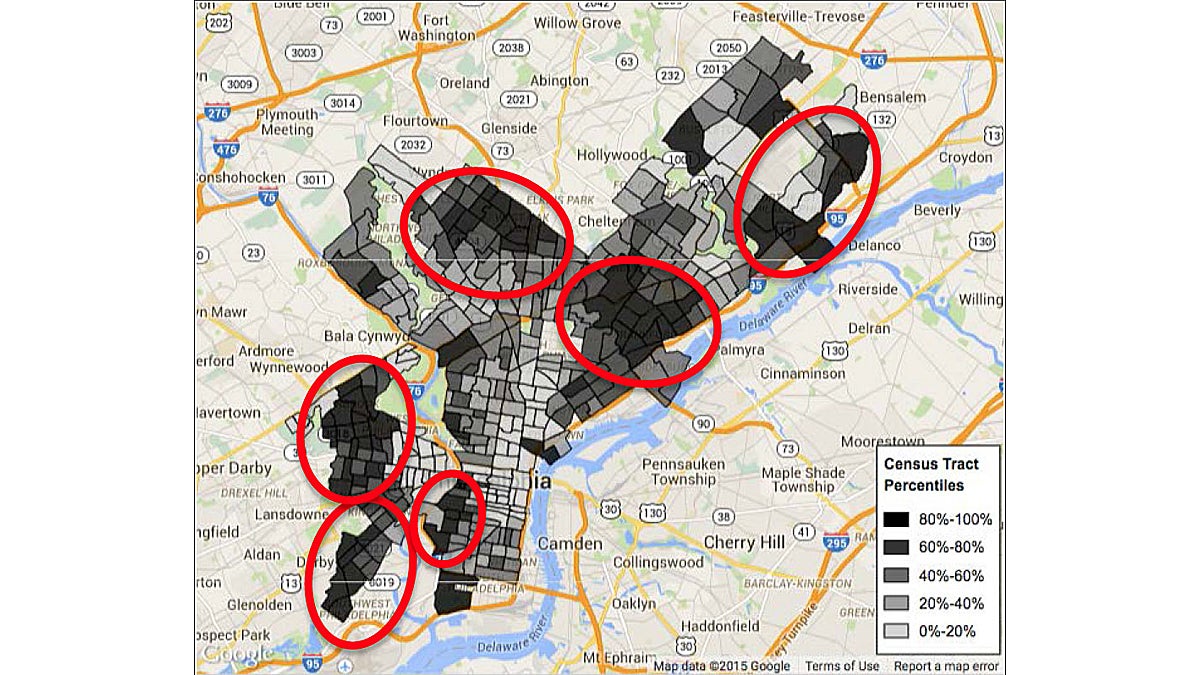
A new University of Pennsylvania study has identified the six areas of Philadelphia with the lowest levels of geographic access to primary care providers. The study focused only on geographic location data rather then outcomes and other health measures that are likely to be targeted in the future. The project was commissioned by the Philadelphia Department of Health and funded by the locally headquartered Independence Foundation. (Map image courtesy of the University of Pennsylvania)
In Philadelphia, ten times as many primary care physicians are within a short drive in the best-served neighborhoods when compared with underserved ones, according to a study released Thursday.
The report, commissioned by the Philadelphia Department of Public Health, found that the ratio of patients to primary care providers within a short drive is about 900-to-1 citywide. But in South Philly, the least-served area, it’s almost 3,000-to-1.
“What we’d like to do is use this report as a starting point for a broader conversation … for how this could inform the growth of new community health centers,” said Philadelphia Health Commissioner Dr. James Buehler, noting the results confirmed a need for expanded services in Northeast Philadelphia, where wait times at the city health clinic are often four or five months long.
Philadelphia census tracts with lower provider densities are clustered in the Northeast and Southwest parts of the city and tend to be more heavily African-American than the general city population.
“If someone lives in an area where there are fewer primary care doctors, they may face longer travel times to access primary care, they may face difficulty getting a new appointment,” said Dr. Elizabeth Brown, the study’s lead author and a Robert Wood Johnson Foundation Clinical Scholar at the University of Pennsylvania.
The report did not analyze travel times to appointments or wait times at clinics to determine how much of a deterrent they may be to residents seeking care, Brown said. “But it does point to areas of the city where we may be at risk for people not having sufficient access.”
Primary care supply overall is associated with improved population health. Decreasing densities of primary care providers have been linked to increased non-urgent emergency room visits.
No causal link has been proved, however, between physician density and overall health in small geographic areas.
“The hypothesis is that if you don’t live in an area where there are physicians around, that’s going to be bad for your health, and the hypothesized mechanism is that people are going to delay getting care that they really need,” said Brendan Saloner, assistant professor at the Johns Hopkins Bloomberg School of Public Health.
Brown said further research is needed to tie geographic primary care access patterns to health outcomes.
“Important next steps,” Brown said, “would include studies of primary care wait times and how different kinds of insurance or lack of insurance may affect the ability to get appointments in various areas.”
All but nine census tracts in Philadelphia have more primary care providers per resident than the federal threshold for a shortage area, suggesting the city has enough primary care providers overall even though access varies geographically.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.

