What patients consider ‘worse than death’ can inform treatment choices
Listen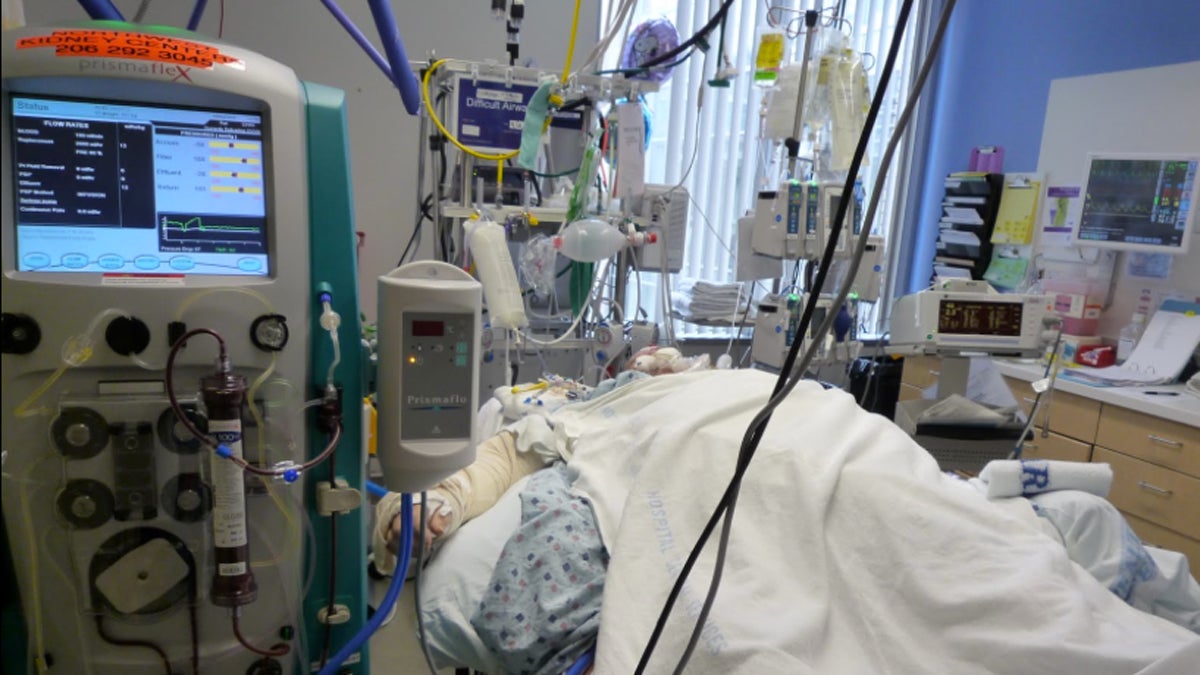 Photo via www.noelhastings.org)" title="hospital" width="1" height="1"/>
Photo via www.noelhastings.org)" title="hospital" width="1" height="1"/>
(Photo via www.noelhastings.org)
Humans go to great lengths to stay alive. Grueling chemo sessions. Huge, life-changing operations. Prolonged hospitalizations. And in dire situations, there’s always a difficult question that looms – how much suffering is too much? How do you weigh quality of life versus quantity of life? At what point would death become preferable?
Thinking about such things hypothetically, it’s difficult, if not impossible, to know what choices we’d really make.
But a new study dug into these questions in hopes of finding answers about what constitutes good care with gravely ill patients, and what patients fear the most.
Researchers at the University of Pennsylvania interviewed patients while they were in the hospital – and asked them about different states of health. It turned out that many patients in this study rated things like severe dementia, being confined to bed, using a breathing machine, having to rely on someone else for grooming and feeding, or being incontinent as equal to, or worse than, death.
“It’s obviously a very complicated issue,” said lead researcher Emily Rubin from the University of Pennsylvania, adding that evaluating the findings means putting them into context. “If you ask people about incontinence for example, I don’t believe if people had isolated incontinence and were otherwise able to take care of themselves, that they would prefer to die. I don’t take that at face value. But I think it does speak to people’s fear of losing control.”
Rubin said that non-death outcomes in patients are more difficult to study and to approach, because they are not as clear cut, and harder to measure.
“But I think we need to try to find ways to incorporate them into clinical practice, avoiding states that people would not want to live in.”
This could mean having conversations about options and outcomes with patients.
“Hopefully, these conversations are happening now,” said Rubin. “But often, they happen late.” She explained that exercising restraint was a difficult path to choose. “The path of least resistance is always to do the next test and the next treatment. It’s harder to take a step back and discuss ‘what is your life going to look like,’ and lay out different options.
In addition to meaningful conversations about choices and options, Rubin says finding ways to translate these conversations into action is key.
“Understanding where people are coming from is very important, but if we can’t find ways to take that information from patients and to translate into better practice, then we’re not making progress.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.




