Healthcare’s case for recruiting more men in nursing
Listen
Registered nurse Elikana Njeri came to the U.S. from Kenya in 2002 and planned to become an accountant. Today he works at Penn State Hershey Medical Center in Central Pennsylvania.(Dani Fresh/for WHYY)
Men are a growing minority in the nursing profession. They make up about 10 percent of registered nurses in the United States.
Registered nurse Frank Poliafico, who graduated from nursing school in 1971, says one of the first things to know about men in nursing is what to call them.
“I’m not a male nurse. I’m a nurse,” he said.
Poliafico is mostly retired these days but helped integrate the nursing ranks in Philadelphia when maybe two percent of registered nurses were men.
He’s stocky with thick black eyebrows, while his mustache and the rest of his hair have gone gray.
He says his patients never had a problem with him when he walked in a room.
“Even when I worked OB-GYN, I worked obstetrics, I never had a women say I don’t want him in here, he’s a man,” Poliafico said.
But in the 70s, some of his female co-workers didn’t take him seriously.
“I’ve had women attempt to embarrass me with off-color jokes that they wouldn’t tell in mixed company. But, it’s only Frank. I’d hear that statement a lot, ‘It’s only Frank,'” he said.
In the first years of his career, Poliafico was working in a big emergency room in Philadelphia, and part of his job was to care for victims of sexual violence.
“I did a little bit battle with a group called Women Organized Against Rape because they didn’t think a man should be in charge of the program, number one, and definitely shouldn’t be in there with a rape victim,” he said.
After an assault, the hospital collected each patient’s clothes for forensic evidence. That meant most women went home wearing paper underwear. It was one more, unnecessary indignity.
“So I went to the social worker, I said: Do you have budget. I said go buy a gross of women’s underwear, and there were women before me, they didn’t think of that,” he said.
Decades later, after Poliafico first entered nursing, the job is still a tough sell for some men.
Workforce researchers say low pay–relative to other professions—and image problems are still barriers.
In the traditional bedside jobs, the skill it takes to dress or bathe a patient—with as much privacy as is practical–is the same whether you are a man or a woman. But associate professor Brian Fasolka, who teaches at the college of nursing at Drexel University, says the perception can be different.
“When a male nurse goes to provide that same care to a female patient, there’s always this concern that the male will be accused of inappropriately approaching the patient or touching the patient,” Fasolka said.
As a result, many men choose nursing jobs that don’t require intimate contact. Those jobs—as nurse manager, ER nurse or nurse anesthetist–often pay a lot more.
In a big city with several medical centers, a nurse with two extra years of graduate school education, can make $150,000 to $200,000, Fasolka said.
But that’s not the norm in nursing.
“When you look at a profession like nursing, it’s 90 percent that’s really seen as women’s work, and it doesn’t get the professional status and recognition that it deserves,” he said.
The gender wage gap in America says a lot about how much we value so-called “women’s work,” he said. Across careers, women still earn just 80 cents for every dollar men earn. With so many nurses around the country getting ready to retire, Brian Fasolka says it just makes sense to use men to fill the need.
There’s been a steady increase over three decades, but only about 10 to 12 percent of nurses are men.
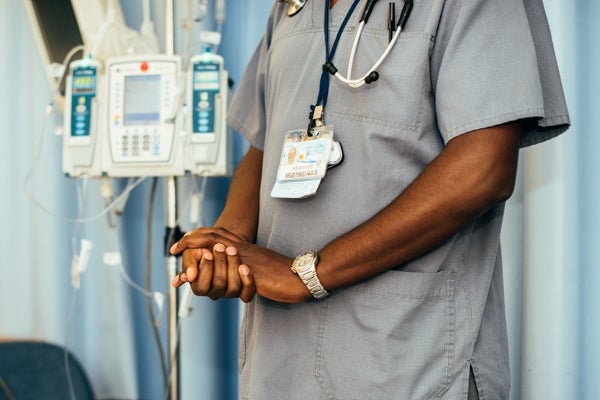
Registered nurse Elikana Njeri clasps his hands while he speaks to a patient. (Dani Fresh/for WHYY)
Misconceptions
Male nursing students at Drexel shared some of their experiences as they enter the profession.
“You can hear the stigma still, you hear ‘murse’ [male nurse] a lot,” said Glenn Burns, who’s from Long Island and used to be a Navy corpsman.
He’s brawny and says he knows how he’s perceived, so he compensates when he first interacts with patients.
“I have a shtick that I perform,” Burns said. “So I put on a light-hearted persona. I have a deep voice, so I try to raise it a little bit, I try to smile more.”
Nursing-school senior Hendrik Bilek from Connecticut says working as a nurse-intern had pushed him to think more deeply about his identity.
“I grew up in a community where being a white male, you are not a minority, and now to be in a minority setting, it is an eye-opening experience, and it’s really humbled me,” he said.
He was a 16-year-old EMT visiting a trauma center in Harford when the “organized symphony of chaos” in the emergency room hooked him. He leads his school’s chapter of the American Assembly of Men in Nursing and the members speak with high school students about nursing.
Alexander Fly from Grosse Pointe, Michigan says people he hardly knows try to convince him he’s chosen the wrong career.
“The thing I hear most often is when are you going to go to med school? Why not med school?” Fly said. “I still haven’t come up with a good answer for that one.”
Thomas Forney, 21, grew up in a small town in South Jersey. When people learn he’s going to be a nurse, there’s still plenty of misconceptions about why.
“They say, ‘oh, so you get all the ladies, huh?’ I never get like ‘you must be really compassionate,’ or anything like that.”
Compassionate Care
On a noisy medical-surgery floor at Hershey Medical Center in Central Pennsylvania, registered nurse Elikana Njeri said he can help prevent medical errors. Nurses do the safety checks that make sure the right medication goes to the right patient at the right time in the right dose, he said.
So, when Njeri needs to hang two IV medications for a patient, he pauses to look up the drugs.
“That’s my part,” he said. “The doctors don’t administer medication, they just order them. They don’t check compatibility of medications.”
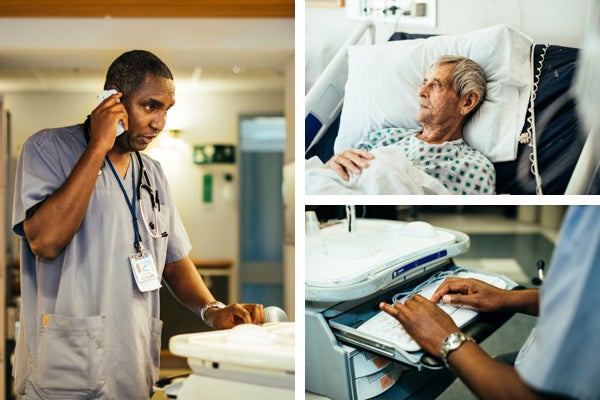
Registered nurse Elikana Njeri checks the medications for patients to try and prevent medical errors from happening. (Dani Fresh/for WHYY)
Njeri wears blue scrubs and he’s solidly built, and he’s never very far from a computer on a cart that rolls along with him from room to room. Each patient’s pain level or bowel movements have to be documented in the electronic medical record to help keep track of the hundreds of clinical decisions Njeri makes each day.
He’s from a small town in Kenya and he says growing up, the nurses he knew were all women.
When he came to America at age 24 in search of a career, he heard there was a nursing shortage. In 2002 hospitals were recruiting aggressively and giving out signing bonuses, but even then, Njeri says he couldn’t imagine being a nurse.
“Honestly speaking, it wasn’t a male job at all. So I thought that I wanted to become an accountant,” he said.
But at his core, he’s a caregiver, a husband, a dad. And at age seven, Njeri became a stand-in parent for his younger brother and sister.
“The main thing was I grew up without a mom. My mom passed on when I was very young,” he said. At the end of her life, nurses were there.
Later, somewhere along the way, he remembered the nurturing care she received and realized he could do that too.
“Maybe if I was in the medical profession I could help people get well and possibly avoid death and avoid suffering,” he said.
Even just finding the least hurtful place to give a patient an injection can make a difference, said Kathy Zimmerman.
Her 75-year-old father, Donald, was healing from a bowel obstruction at Hershey Medical Center, and after several surgeries, his stomach was covered in scars.
When it’s time for the next shot, Njeri takes a moment to ask Zimmerman if there’s another space on his body where he’d prefer to get the injection.
“He’s really experienced, and Dad feels a lot more secure with him,” Kathy Zimmerman said.
There’s a strength about Ngeri. Kathy Zimmerman said he’s a good nurse, but she doesn’t think it’s because he’s a man.
“It’s more about compassion, caring,” she said.
A national group—the American Assembly for Men in Nursing—wants men to represent 20 percent of U.S. registered nurses by the year 2020.
There are recruitment posters and YouTube videos and advocates say they’d like to take gender out of nursing, they call it an effort to “de-gender-ify.”
The association also offers college scholarships and gives awards to the best schools and workplaces for men.
Experts say–beyond political correctness—there’s a real value in having more healthcare workers with different backgrounds. Advocates argue that kind of diversity can lead to better care.
Nurses do health education, they urge patients to try new health habits – and that requires connection and communication. It’s all just part of the care nurses give, said Drexel associate professor Brian Fasolka.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



