Dentists reassess their role amid growing opioid crisis
Listen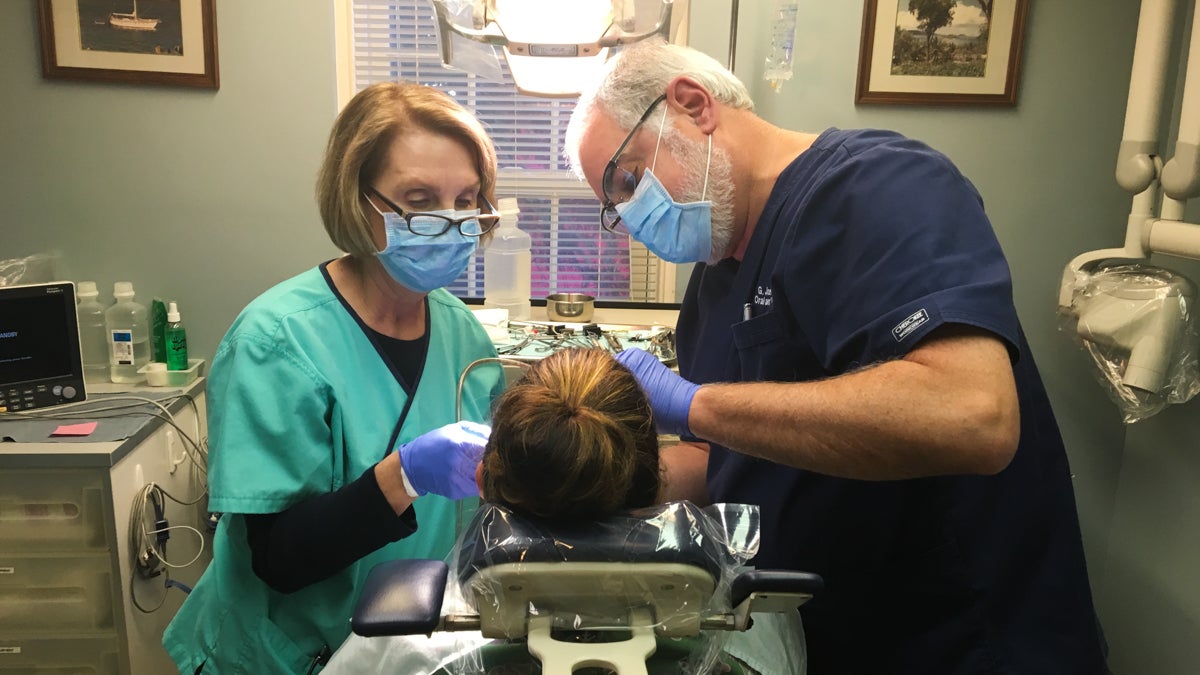
Dr. Joel Funari performs some 300 tooth extractions annually at his private practice in Devon
Firsts can be life changing. Think about your first kiss. Your first time behind the wheel of a car. But what about the first time you got a prescription for a narcotic?
James Hatzell didn’t realize it at the time, but that spring day of his junior year of high school was a pivotal moment for him.
“We’re in our 2001 Honda Odyssey minivan, driving to the dentist. And we get there, and I’m just pumped,” Hatzell recalled. “I was very excited to get my wisdom teeth out.”
This was almost seven years ago. Hatzell was 17, and he was about to join the ranks of the more than 3.5 million people annually, mainly young adults, who get their wisdom teeth extracted. But he distinctly remembered having those weirdly positive thoughts, while en route with mom, to what one would typically imagine to be a very, very terrible thing.
“I’m like, ‘alright, let’s do this thing!'” he said.
Hatzell’s excitement stemmed from his savvy teen knowledge that after the dentist cut out his third molars, not only would he get to sit around and eat ice cream, he’d get his very own bottle of pain pills.
Dentistry at a crossroads
Dentists, oral surgeons and endodontists have long occupied a rather overlooked position when it comes to addressing pain. While general practitioners and primary care doctors have taken the spotlight, especially in the last year, dentists are also frequent prescribers of immediate- release opioids like Vicodin and Percocet.
In some ways, who can blame them? They see patients experiencing some of the worst of it, from terrible tooth infections to the cruel phenomenon that is a dry socket (this is the condition when a nerve becomes exposed after a tooth extraction). They also provide post-operative pain management for procedures like the one Hatzell underwent.
But as the nation struggles with a major drug epidemic, one that has been linked to some 165,000 prescription drug overdose deaths in the last 15 years, and one that has in part been fueled by the misuse of prescription painkillers, dentistry is at a crossroads.
When prescriptions go unused, they may be diverted for non medical use. One report estimated that a fifth of opioid prescriptions are subject to medical misuse.
It all means that many in the field are now reassessing their role in ways they might not be used to. That has meant new approaches and an even more elemental realization about how to best treat the pain that’s rooted in the mouth.
Spoiler alert: it doesn’t involve opioids.
The significance of a prescription for one high schooler
Up until that dentist visit, narcotics seemed kind of scary to Hatzell. He’d actually tried Vicodin before, but with caution. Friends would find an extra pill in a medicine cabinet at home, they’d crush it, mix it with pot, and share it.
This was different.
For the first time, a health professional was going to say, ‘Here. This is OK to take. In fact, it will help you.'”
On the way home from the dental office that day, Hatzell was still high from the drugs given during the procedure. Still, he could not wait to pop that first pill.
His mom noticed.
“We got home, and my mom took the pills and was like, ‘you can’t have these.'”
End of story, right?
Wrong.
Being the trickster kid that he was, he knew exactly where that bottle was hidden. He had a plan for not getting caught. In a move that might be every parent’s worst nightmare, he snuck into mom’s room, emptied out the pills, and replaced them with Advil or some other over the counter drug.
Mom had no idea.
“And, you know, I start taking them,” he recalled.
Hatzell says he can joke about this now, but nothing about what happened to him or his family was funny then. That prescription would mark the start of a downward spiral, one that would include being arrested for dealing drugs in college in Pennsylvania. He nearly lost everything.
Up until that point, Hatzell had only dabbled with pills. For him, that dental visit somehow legitimized them. It took the fear away.
“I had never had a large quantity of them that I could just take as much as I wanted,” he said. “And it was sort of a defining moment in my addiction and my downfall, where I thought that that became OK.”
A ‘movement’ in the field
When Dr. Joel Funari started out as a dentist more than three decades ago, he recalled it was not that uncommon for people in his field to prescribe a bottle of 30 or more strong narcotics to someone after taking out their wisdom teeth.
“Dentists don’t like to see patients in pain, they want to get them out of pain,” he said. “You know, we tend to be compassionate people, and I think we were falling into a trap we were creating ourselves.”
It was a trap, he says, of excessive prescribing.
Dr. Funari, who specializes in oral and facial surgery, takes out a chart from the Substance Abuse and Mental Health Services Administration that lists the top prescribers of Hydrocodone combination drugs like Vicodin between the years 2007 and 2011. He points to dentists, which rank only below general practitioners and internal medicine doctors. A 2012 National Prescription Audit by IMS Health, meanwhile, ranked dentists as the fifth most frequent prescribers of opioid analgesics.
But the challenge is, it can be tough to figure out when these strong, potentially addictive pain meds are appropriate, and when they’re not.
Dr. Funari worked in the navy for two decades and these days, performs wisdom teeth extractions upwards of 300 times annually inside his practice in Devon, Pa. In 2014, he was part of a group tasked by the state department of health to come out with opioid prescribing guidelines for the field. None existed, he said.
In reviewing some of the latest research, he realized something he had long suspected and applied his own practice. There’s a better way to addresss standard dental pain that’s not opioids, even for standard wisdom tooth extractions.
“Non steroidal anti-inflammatory drugs (NSAIDs) – the Motrins, the Advils, the Aleves – when used in a certain way – are very effective, more effective, than the narcotics,” he said.
Those drugs keep the swelling and inflammation down, which is a main source of the pain, he said. “So look at the root cause to try to remove the stimulus and remove the after effect.”
And because wisdom tooth removal is done so often, it has actually been an ideal procedure to study the benefits from this approach (and the general effectiveness of nonsteroidal anti-inflammatory drugs).
“That has not filtered down to the level of the general dentist, the smaller practice and some of the subspecialties,” he said. “And that’s basically what we’re doing now.”
The 2014 guidelines are the state’s first on prescribing narcotics for dental patients, but discussions within the dental community about opioid prescribing practices appear to be growing.
Dr. Funari says depending on the situation after a wisdom tooth extraction, he’ll send a patient home with a dose of the non sterioidal anti-inflammatory drugs, and generally 10 narcotics, “which is enough to get them through three days or a weekend if they need it.”
Across the state, Dr. Paul Moore, a dentist and pharmacologist at the University of Pittsburgh’s School of Dental Medicine, has also been researching the use of ibuprofen and other NSAIDs in acute pain management. In the last year, he has worked at the national level, as part of the American Dental Association’s council on scientific affairs, to come up with new guidelines. They’ll be out next year, and Moore says it’s the first update in ten years.
“I think what we did with the revision of the statements were to provide more specific directions for practice, with regard to using non steroidals as your primary line of analgesics, using prescription drug monitoring programs, and some issues regarding education both in dental school and continuing dental education,” he said.
For him, the effort is also personal. Pennsylvania experienced more than 3,000 overdose deaths last year, and he too recently lost a family member to a drug overdose.
“I’m very sensitive to the issue,” he said.
State dental boards and associations are also developing additional opioid education materials for patients and trainings for dentists that echo these themes. Pennsylvania will soon require trainings for new dentists and for those renewing their license.
Moore and others are particularly concerned about adolescents. While opioids have their place when used appropriately, some worry that for a small portion of young adults, receiving legitimate prescriptions could be associated with an increased risk of future longterm use or misuse.
Young adults are “risk takers,” acknowledged Dr. Moore. “The wiring in their brain is not complete, so they’re certainly more willing to try out new things that are dangerous than adults.”
And that, he says, puts dentists in a unique position to counsel patients about what a narcotic prescription means and to be “thoughtful and responsible” when writing those scripts.
Challenges in changing practices
One challenge, though, is countering long-held perceptions.
“The opioids have a lot of hype,” said Dr. Elliot Hersh, a professor of pharmacology and oral surgery at the University of Pennsylvania School of Dental Medicine and a research collaborator with Dr. Moore.
Hersh is a leading researcher on post operative dental pain (some drug manufacturers have funded his research), and he says anti-inflammatory drugs like Ibuprofen just don’t have as much hype.
“Why? Because they’re available over the counter,” he said. “And what a lot of the lay public believe is if they’re available over the counter, they’re weak and they don’t work.”
It’s also taking a while, he says, to cut through the noise of widely marketed over-promises to the public and to doctors that opioids were the ideal option, that they weren’t as potentially addictive as we now know they are. He takes a self-described hardline approach in the classroom with future dentists, even bringing in a retired narcotics officer to be a regular presenter in his class.
“I’ve been teaching my students that you have to be really, really careful with these drugs,” he said. “That if you write too many of these drugs, for either good or bad intentions, either the state dental board and, or the DEA [Drug Enforcement Agency] is going to come down on you.”
Still, none of this is an exact science. Every patient’s response to pain is unique.
Hersh has found around one in five patients still need a combination of both anti-inflammatory medication and narcotics to control it.
And here’s the problem.
“The patients are still numb when we prescribe, so we don’t know who that 20 percent is going to be that also requires an opioid added on,” said Hersh.
A doctor may have a sense of what’s to come, depending on what happened during the surgery,but why some patients feel more pain than others is still a mystery. It all means that dentists may end up writing a prescription for at least some opioids to be on the safe side. If a patient has breakthrough pain in the middle of the night, a dentist can’t just call in a prescription because of the drug’s classification.
Even though about three quarters of some 560 clinicians surveyed by the American Dental Association a few years ago preferred ibuprofen in treating post operative pain for wisdom teeth extractions, even more – some 85 percent – reported that they still prescribed an opioid. The average was 20 tablets of a hydrocodone acetaminophen combination, to be taken “as needed.”
Still, it’s a tricky scenario, as the issue then becomes “they use one or two [pain pills] and there’s eight left over,” said Hersh.
And it was leftover drugs, remember, that became a problem for James Hatzell.
Lessons learned and looking ahead
Hatzell is 23 and has been in recovery for three years now. He’s involved in student recovery initiative, ones he credits as helping him when he hit his low as a student at Penn State. But along the way he has seen other peers take a darker turn.
“What it’s like graduating high school in the 2000s or the 2010s is your classmates die. They overdose on drugs and they die,” he said. “You’ll see in the obituary ‘died suddenly, died in their sleep’ or there’d some courageous family that would publicly state that they died of an overdose.”
For Hatzell, one of his most terrifying thoughts as he now navigates his own addiction is that one day, he might need surgery, that his ACL might rip, or that he might develop a bad tooth infection.
But it’s not the actual rip, or the procedure itself that frightens him. It’s the drugs.
“Because I don’t want to take any at all, but I might be put in a situation where it’s medically appropriate for me, and I don’t want to make that decision,” he said.
For that reason, Hatzell makes it a point whenever he goes to a dentist or doctor to say right up front that he cannot take narcotics.
Pennsylvania, New Jersey and most other states now have databases that will show dentists a patient’s prescription history. There’s a push for a national database, too.
But the next step, in how dentists will use that information and make referrals, is something that Dr. Funari and others are still working on.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



