Study says Philadelphia area a pocket of high charge-to-cost hospitals

Hahnemann University Hospital (Emma Lee/WHYY)
Beware of some especially big medical bills, at least if you’re paying the full price. A new analysis has identified the 50 American hospitals with the highest markups, and six cluster in the greater Philadelphia area.
According to the report, only Florida has more hospitals with outsize charges than Pennsylvania, which claims a seventh hospital in the Lehigh Valley.
Half of all hospitals to make the list are owned by Community Health Systems, including five of the Pennsylvania hospitals, and the one with the highest ratio of charges to costs in the state, Chestnut Hill. The group also includes Hahnemann University Hospital, which ranked 34th, and the sole non-profit hospital, Crozer-Chester Medical Center.
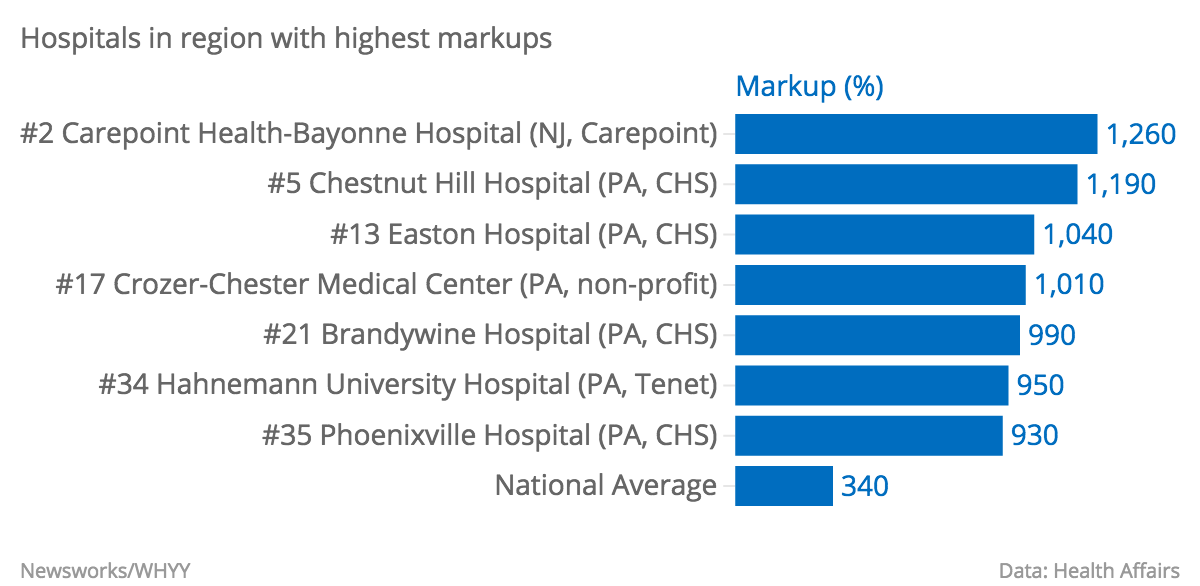
For nearly 4,500 hospitals in the United States, researchers compared total charges to a hospital’s Medicare-allowable cost using data submitted to the government. While charging more than Medicare is standard — the average American hospital bills 3.4 times the rate — in the most extreme cases, that billows to 10 or more times.
“We found that many hospitals are charging 1,000 percent of their costs,” said Ge Bai, a professor of accounting at Washington and Lee University, and lead author of the study, which was published in Health Affairs.
“This price gauging game trickles down to every single consumer,” she said, noting that it was worst for vulnerable populations such as the uninsured or those with workers’ compensation. “It really plays an important role in the rise of our overall healthcare spending.”
But Martin Ciccocioppo of the Hospital and Healthsystem Association of Pennsylvania said that focusing on the “list” price is deceiving because patients rarely pay that price, even if they are uninsured.
“The better thing to look at is what is payment to cost,” he said. “What that indicates is that hospitals are barely making enough money to provide the services that are needed in their communities.”
In statements, area hospitals said that high charges did not reflect the amounts paid, and charity care is available.
Dan Polsky of the University of Pennsylvania’s Leonard Davis Institute of Health Economics said the clustering of steep charges might be due to negotiation tactics hospitals take when trying to get the best reimbursements from an insurer when joining a network.
“If neighboring hospitals have high charges when they negotiate with insurers, it induces other hospitals nearby to use similar strategies,” he said.
In exchange for volume, insurers typically pay in-network hospitals less for each procedure.
Such a system, when concentrated in a geographic area, might lead to higher premiums for insured patients. But Polsky said this was unlikely to account for a sizable increase.
“I think the larger issue is we need to pay attention to the costs, and frankly there’s a real transparency problem,” he said. “Unless we address price transparency, people are going to get upset about charges because that’s all they really get to see in public.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.

