Region’s first double-hand transplant a success
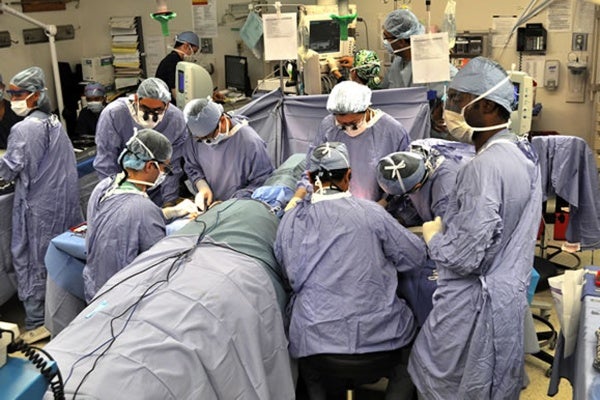
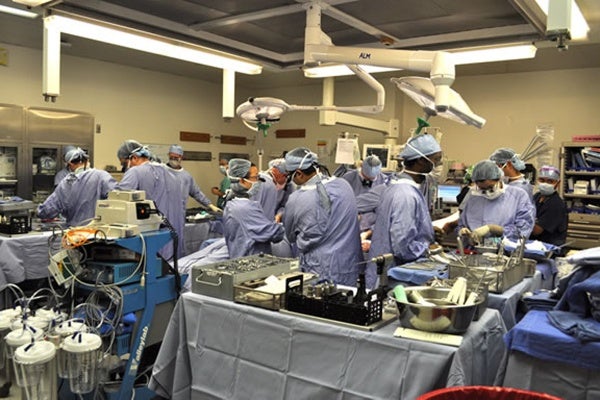
A team of Penn Medicine doctors and nurses successfully completed the region’s first bilateral hand transplant in September. Today, they offered the first update on the patient’s status.
Doctors say their patient, who was identified only as a woman in her 20s, is doing well and has not rejected the hands so far. She is wearing splints, and is able to gesture, wave, and feed herself.
The surgery took close to 12 hours and the efforts of a 30-member team. The patient’s arms were joined with the donor arms just below the elbow.
Dr. Scott Levin, who directs Penn’s hand-transplant program, said the hope is that the patient will gain fine motor skills as her own nerves merge with the transplanted arm.
“At this level, the nerves have to grow into the muscles, the muscles have to be activated by signals from the brain,” said Levin. “As the muscles get their nerves back, those muscles start to work, and then the tendons that are attached to muscles activate the fingers.”
The surgery was more than two years in the making, Levin said, and required intense planning. Its completion marks another achievement in the emerging field of vascularized composite allotransplantation or VCA. Multiple tissues such as muscle, bone, nerve and skin are transplanted as a functional unit.
So far, doctors have transplanted faces and hands. Penn Medicine doctors said this field holds a lot of promise, but involves ethical concerns that don’t come up with organ transplants.
Hand transplants are life-enhancing, not life saving–but still carry a lot of risks.
Dr. Abraham Shaked, who heads Penn’s transplant institute, said he was reluctant at first to get involved in such transplants. He said he changed his mind when he met the young patient who had lost her arms just below the elbows, and realized how difficult her life was.
“You start to think about life in a different way, and the life of this patient, and I looked at her and I said you know, one of these days, I would like to shake your hand,” recalled Shaked.
Shaked said it is essential to make sure patients understand the risks and benefits of the operation.
This emerging field of transplants also poses new questions and challenges for potential donors since hands and faces are visible, and are a recognizable part of a loved one.
Ethics experts at Penn said conversations are ongoing to make sure patients and donors feel comfortable that they are making informed decisions.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.