Distribution and use of naloxone rise in N.J. and across nation
Various data sources make it clear that easy access to the overdose antidote is critical in preventing opioid deaths.
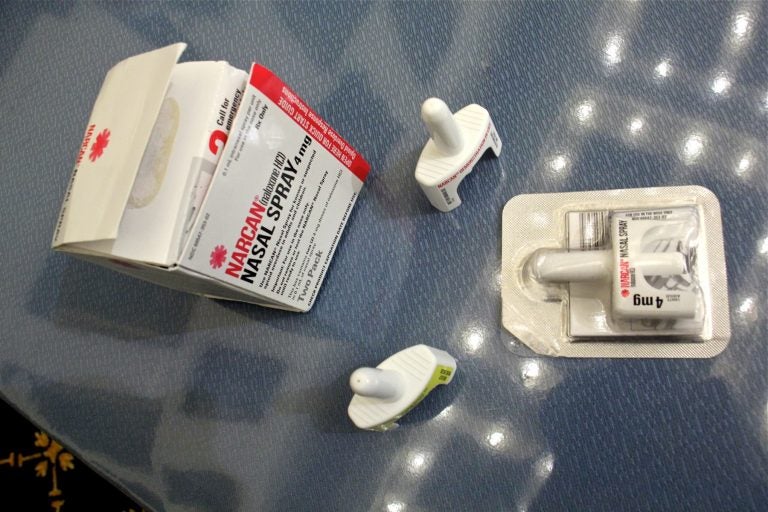
Naloxone, commonly known by its brand name, Narcan (Emma Lee/WHYY, file)
This article originally appeared on NJ Spotlight.
—
New Jersey has worked for years to expand access to naloxone, including holding in June what officials believe is the nation’s largest single-day give-away of the opioid-overdose reversal agent.
Through that initiative, drugstores armed 16,000 New Jerseyans with the life-saving antidote, each receiving a two-dose pack of a nasal spray version of the drug, according to the Department of Human Services, which oversaw the multi-agency effort. In the Garden State, naloxone is available without a prescription at pharmacies that have a blanket order to provide the medicine.
“Expanding access to naloxone is a key part of the Murphy Administration’s strategy to save lives and combat the opioid epidemic,” DHS Commissioner Carole Johnson said. “Parents, friends, and neighbors from across the state came out on our Free Naloxone Day to be part of the solution and are now better prepared to stop overdoses and save lives.”
Naxolone, also known by the brand name Narcan, is also clearly being used, according to the DHS and figures compiled by the Office of the Attorney General. Law-enforcement and emergency-medical responders alone have administered more than 58,700 doses in the past five-and-a-half years, with its use quickly ticking up from nearly 5,200 doses in 2014 to more than 16,000 last year.
The medication is easy to administer and it can usually reverse almost immediately the dangerously slow heart rate, breathing and other potentially deadly effects of heroin or other opiates, although some patients require multiple doses. State officials said it is available on an ongoing basis — although not for free — at many major-chain grocery stores and pharmacies, as well as the state’s harm-reduction centers, which include needle-exchange programs.
“Standing orders allow pharmacists to dispense naloxone to individuals at risk of an overdose or to an individual who wants to administer it to a loved one or someone in an emergency,” said Judith Persichilli, the acting commissioner of the state Department of Health.
NJ trend reflected in national numbers
New Jersey is clearly not alone, according to new federal figures that show distribution of naloxone more than doubled nationwide from 2017 to 2018, with more than half a million doses dispensed by pharmacies alone last year.
The findings, published Wednesday by the federal Centers for Disease Control and Prevention, also show, however, that significant disparities exist in access to naloxone. And with more than 48,000 overdose deaths recorded in this country in 2017, the researchers said more needs to be done to expand access to the antidote.
“Thousands of Americans are alive today thanks to the use of naloxone,” said Alex Azar, secretary of the U.S. Health and Human Services Administration, which oversees the CDC. “With help from Congress, the private sector, state and local governments, and communities, targeted access to naloxone has expanded dramatically over the last several years, but today’s CDC report is a reminder that there is much more all of us need to do to save lives.”
Among other things, the CDC findings showed naloxone is three times more readily available in urban counties than rural ones. In addition, across the nation, there were 25 times more prescriptions written for the drug in highest prescribing communities than the lowest. (Most states also make the medicine available to people without a prescription, the report notes.)
Garden State research shows a slightly different pattern. In May, Rutgers University’s New Jersey Medical School shared a study that showed the medicine was three times more likely to be stocked by drugstores in smaller, affluent communities than in urban areas of the state. This disparity reflects, in part, the lower number of chain drugstores — some of which embraced Narcan distribution early on — in cities.
The CDC study also showed both that, while opioid use has fallen significantly nationwide — from 48 million prescriptions in 2017 to 38 million last year — there is still only one naloxone dose dispensed for every 70 high-dose opioid prescriptions.
Impact of fentanyl
In the Garden State, opioid prescriptions have also declined by double digits in recent years, thanks to public-policy changes and multiple efforts by providers to change how they treat pain.
But drug-related deaths have continued to escalate, topping more than 3,000 last year — in part because of growing use of fentanyl, the even-more-powerful synthetic additive.
Numbers from the OAG suggest this could be turning around, however, as the death toll has declined somewhat when compared to last year: There were 1,387 drug related deaths in the first half of 2019, versus 1,494 over the first six months of 2018.
New Jersey officials have also sought to expand access to treatment in a variety of ways, including medication-assisted treatment (or MAT), which experts consider the best option for reducing relapse and supporting recovery.
The DHS has launched widespread training initiatives to increase the pool of providers and made it easier for Medicaid patients to qualify. And in another national first, in June the health department enabled trained emergency responders to dispense key MAT medications after administering naloxone to a patient.
The DOH is also hosting a free public event — Fighting Stigma to End the Overdose Epidemic: A Harm Reduction Workshop — at the Trenton War Memorial on Aug. 21, in which national and local experts will examine the role of harm-reduction programs in saving lives, curbing the spread of disease, promoting health, and reducing stigma around addiction.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.