Delaware sees a drop in state’s high unplanned-pregnancy rate
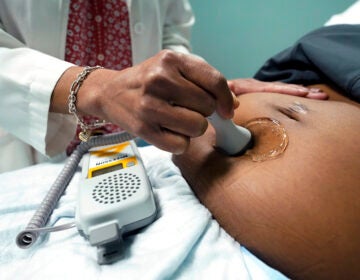
The state of Delaware is working with reproductive-health nonprofit Upstream USA to increase access to all kinds of birth control, including longer-term methods.

(Valeria_Aksakova/BigStock)
Brittany Vice said she wasn’t consistent with birth control, missing a pill about once a week.
Her demanding and fluctuating class schedule — she’s a recent college graduate — played a major role in that, she said.
“I would try to take it in the morning when I woke up, but I woke up at different times depending on when my classes were. I couldn’t find a time consistently every day I would be able to take it. The stress of college and having so many things to think about — it wasn’t something I prioritized as much as it should have been a priority,” Vice said.
“Other than the fact I could have gotten pregnant, my period was inconsistent, so I was getting it more often because of missing pills, so that obviously isn’t fun. So it was affecting my life in a lot of different ways, I would say.”
Vice visited a provider in Pennsylvania, where her parents live, to learn about alternative birth-control methods such as the IUD. But her parents’ insurance plan, through which she had coverage, would have charged $2,000 for insertion of an intrauterine device.
“Obviously, being a college student, money is definitely tight,” Vice said. “I had money at the time, but I was just using that for spending money. Being in school, it was hard to work any more than a few hours a week. So $2,000 would have been my whole savings at that point.”
Six months later, she heard about DelawareCan (Contraceptive Access Now), an initiative between reproductive-health nonprofit Upstream USA and the state of Delaware, during her maternity class at the University of Delaware, where she was a nursing student.
After doing some research, Vice was able to schedule an appointment with Planned Parenthood and get an IUD the same day at no cost.
“The main thing is I don’t have to think about it ever. Going from taking a pill every day, to not have to think about taking anything and still being protected and not worry about getting pregnant has really been beneficial,” she said. “It’s just one other thing off the checklist.”
Delaware had the highest rate of unplanned pregnancy in the nation in 2010: About 57% of Delaware’s 19,300 pregnancies were unintended, according to the Guttmacher Institute.
The highest percentages of unintended pregnancy occurred among women and girls under 20 — 83% between 2012 and 2015, according to state figures. In 2015 alone, state data showed that among Delaware women younger than 20 whose pregnancy resulted in a live birth, 76% indicated that the pregnancy was unintended. For comparison, 43% of women ages 25 to 34 whose pregnancy resulted in a live birth indicated the pregnancy was unintended.
“Why that matters is because there are health consequences to unplanned pregnancies,” said Karyl Rattay, director of the state’s Division of Public Health.
“Moms are less likely to get the prenatal care needed. Babies are more likely to be born early. We’re more likely to see issues with infant mortality. We’re more likely to see issues with substance disorder,” Rattay said. “Additionally, women who have children prior to being ready are less likely to achieve their educational and career goals, and often that leads to more economic challenges. A child is more likely to grow up in poverty if a mother is not ready to have a baby.”
She said Delaware has one of the highest infant mortality rates in the nation, 6.6 per 1,000 births in 2017, and while the state is improving those numbers, it still is a concern.
The DelawareCan campaign is showing promise, however, Rattay said. The Maryland-based research organization Child Trends estimates that since the campaign launched, unintended pregnancies in Delaware dropped from 106 per 1,000 in 2014 to 80 per 1,000 in 2017. The simulations are based on contraception use among Title X Family Planning patients aged 20 to 39.
The Guttmacher Institute, which analyzes data of all pregnancies, including those that are terminated or miscarried, estimated unintended pregnancies fell from 57% to 48% in 2014.
And Delaware’s Pregnancy Risk Assessment Monitoring System, which is limited to data on live births, saw unintended pregnancies fall to 43% in 2017.
Upstream USA co-CEO Mark Edwards became interested in the issue while running another nonprofit called Opportunity Nation, which focused on creating pathways between community colleges and employers.
“In those conversations, it was surprising how frequently their stories were, ‘I got my girlfriend pregnant, and I had to drop out of school,’ or ‘I got pregnant, and I had to leave the workforce,’” he said.
During that time, Edwards was working with then-Delaware Gov. Jack Markell, who asked him to develop a plan to work with health-care providers throughout the state to ensure that women have access to a full range of contraceptives. That’s when DelawareCan was born.
The campaign helps health-care providers offer all methods of birth control, and educates patients about their options. And while it does not focus solely on long-lasting methods, it has reduced barriers to obtaining an IUD, such as insurance companies requiring prior authorization or placing on the patient the burden of an out-of-pocket cost.
Edwards said many of the hurdles were in the health-care practices themselves.
“What we found too often was women were given a false choice … ‘You can get a pill right now, here’s a prescription, or it will take three or four visits to get other methods of birth control.’ And that’s not a reasonable choice. There’s no medical basis behind that,” he said.
“Women should be able to get access to any method of birth control, with terrific patient-center counseling, in one visit.”
Karen Antell, a physician with Christiana Care Health System, said that prior to DelawareCan, to get an IUD a patient first had a consultation and then was required to return at another date for the insertion. Sometimes, patients would not return.
There were other risks too.
“Unfortunately, some people come back for that insertion visit with that unwanted pregnancy test,” Antell said.
DelawareCan opened the doors, allowing doctors to offer IUD insertion at the first appointment. The campaign also has educated health-care practices on birth control options and debunked myths. Antell said some practices incorrectly believed that, to qualify for an IUD, the woman already had to be a mother, be monogamous, and have no history of disease spread through sex.
Rattay said some of the debunking also came down to educating administrative staff.
“We would hear stories about a person who answers phones in one clinic and says, ‘Those IUDs give you cancer.’ That’s not true,” she said.
IUDs do have a history of a higher risk of infection and other side effects, and there have been lawsuits against various IUD brands. But doctors say they have come a long way since their introduction in the 1960s. And they are more effective than the pill, which must be taken at the same time every day, and must be absorbed.
“They are effective and people are starting to come around. We’re seeing younger people using these methods. There has been an evolution of the devices to improve tolerance. The implant has improved over time, and I think people are tolerating that,” said Gordon Ostrum, an OB/GYN.
“Oral contraceptives work quite well if you take them quite well,” he said. “All of us tend to put things aside. You might not take your blood-pressure medicine as religiously as you should, so your pressure goes up and you fix that in a relatively short order. If you don’t take your oral contraceptive, that’s a longer-term solution if there’s a downstream effect from that.”
Edwards said the DelawareCan campaign also focuses on billing and coding so offices can get reimbursed. And it requires medical staff to ask the important question, “Do you plan to become pregnant in the next year?” so doctors can notify women of their birth control methods if they do not wish to get pregnant in that time frame.
Antell said she’s seen positive results since the campaign launched.
“Not too long ago, I had a young woman who was only 21 years old and has a child. She was planning to finish school, not become a mom at that time, but it didn’t happen that way,” Antell said.
“When she heard about our efforts, she came with her child to have an implant placed, and she was really happy to have a method she could control. She wants to be able to finish her degree.
And she brought her sister with her for moral support, and her sister is 18 and saw her sister having her implant, and asked for one too.”
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.