The Obamacare rollout continued: The varied fates of three enrollees
ListenNow that the clock has wound down for health care enrollment through the Affordable Care Act this year, The Pulse thought it a prime time to revisit several people who tried early on to navigate new options.
What happened?
Below are the stories of how three people navigated their way through the system and ended up with different fates.
Early payoffs for determined jazz singer
62-year-old Suzanne Cloud, a musician and adjunct professor living in Collingswood, N.J., wasted no time last fall, logging onto the federal website to try and find coverage. She has several chronic conditions “typical that a person my age would have,” but her age and health status previously priced her out of insurance.
For years, she had a routine when she needed to see a doctor. The receptionist would ask, do you have insurance?
“I’d say, no! I’m one of the 52 million Americans who don’t have insurance,” she recalls, laughing. She would do this loudly, so everyone in the waiting room could hear her. “Some would clap. Others would just look at me like I was insane,” she says with a smirk.
Cloud is blunt because so many of her musician friends are too embarrassed to talk about their health, she says, and they suffer. She has watched some die, prematurely, and she has postponed some of her own care, for diabetes and hypothyroidism, all due to cost.
But on a recent visit to the doctor, she started a new routine with the receptionist.
“I’ve got insurance!” she sings, while flashing her new, shiny insurance card across the check-in counter.
Cloud is one of at least three million people nationwide, and more than 100,000 in New Jersey, who enrolled in Medicaid since the fall, as part of the Affordable Care Act. She qualified because New Jersey expanded its eligibility guidelines, allowing low-income single adults to sign on.
Her eligibility and enrollment process was confusing for all those technical reasons plaguing the whole system’s roll out, but by mid-January, Cloud was finally set with coverage.
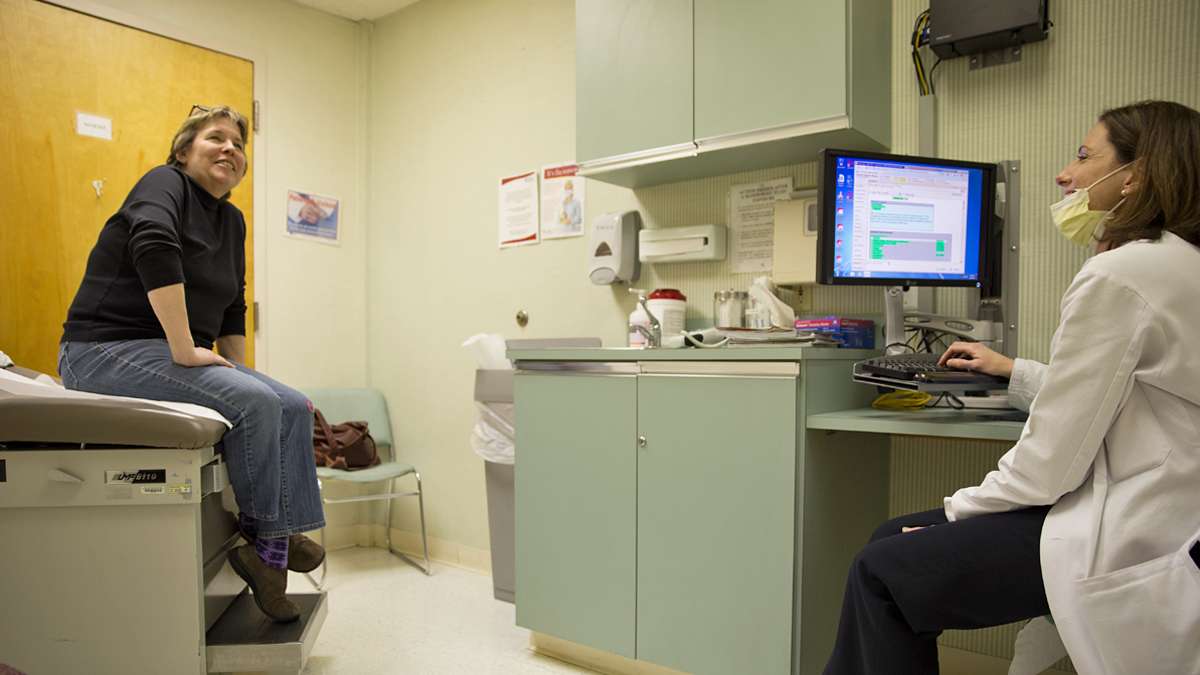
She put her new coverage to use for the first time in March, visiting her longtime doctor. Inside the exam room, the two were frank about how the change in insurance will positively affect Cloud’s care.
Dr. Mary Monari, affiliated with Cooper Hospital, admits caring for Cloud when she didn’t have coverage made her anxious. Her prescriptions were limited, specialists like endocrinologist – to help her better manage her diabetes, were too expensive.
“It’s nerve-racking,” she says. “You know there are certain risks of premature heart disease, strokes. You really want to make sure that you provide the best preventative care you can, especially for a diabetic and to know right off the bat that it’s limited. It’s nerve-racking.”
This time, however, Cloud leaves her visit with a thick stack of specialist referrals and prescriptions.
“I’m feeling very happy. I’m ecstatic!” she says. “This really lifts an entire weight off my shoulders.”
‘Feeling good’ but apprehensive about details
33-year-old Danielle Gatto, of Philadelphia, learned she had Crohn’s, an inflammatory bowel disease, after a painful, unanticipated trip to the emergency room in 2005.
She was uninsured.
“The very first time that I went to the hospital with a Crohn’s disease flair-up, before I knew what it was, I ended up racking up a $40,000 bill,” she says.
Gatto, a bar/restaurant manager and freelance video producer, says thankfully, she got into a charity care program through the hospital. She didn’t want to be in that situation again, but found it nearly impossible to find private health coverage. Insurers kept rejecting her.
“Its been frustrating,” she says. “Basically there was a clause that people that needed the health care the most were not able to get it.”
That pre-existing condition clause went away on January 1, 2014, when the Affordable Care Act started barring insurers from rejecting people like Gatto or charging them more for coverage.
In Pennsylvania, Gatto did find a special “guaranteed issue” option. She describes it as a very bare-boned plan, only available to low-income residents regardless of their health status. It doesn’t cover her medicine and is limited to four doctor’s visits a year. Hospital care is only covered if she’s admitted.
So it didn’t bother Gatto when her insurer notified her the plan would be canceled this spring because it didn’t meet essential benefits standards under the Affordable Care Act. She figured she’d find a better plan through the Marketplace.
But all the new options made her “head spin,” and she wasn’t sure how to confidently pick a plan that would meet her needs.
“The idea of kind of gambling and saying, well I don’t’ think I’ll get sick, but if I get this amount of sick, it’ll cover that. I did a lot of math.”
The biggest blow, an expensive treatment she has put off for her Crohn’s didn’t appear to be covered under any plan. By December, she was still set on keeping her current insurance, the one that she disliked, as long as possible.
After a lot more contemplation, weighing premiums and deductibles, Gatto recently settled on a new Marketplace plan, in part because her other insurance will be cancelled this spring. She’s happy with the decision, though.
“In the end I kind of just closed my eyes and pointed at something, but I felt good about it,” she says.
Gatto qualified for federal discounts, making her plan’s premiums “amazing” at $33 a month. It has unlimited doctor’s visits, and hospital care appears covered regardless of whether she’s admitted. Gatto says the plan gives her more freedom to pursue video production gigs because her previous plan, a special program, required her staying below a certain income to be eligible.
Even so, Gatto worries a lot about the fine print of her new plan.
“Health care is one of those things they can sell to you without showing you exactly what you’re buying,” she says. “The information about each plan that was provided I felt was so basic. How is this actually going to work out?… Is it going to be covered?”
Gatto says it’s only a matter of time before she’ll likely have more answers. Her last hospital trip due to a painful Crohn’s flair-up occurred last fall, and she expects it could happen again this year under her new insurance.
Gatto says finding needed care when there are coverage gaps requires being savvy, clever and persistent. Can’t afford that inhaler? Perhaps there’s a coupon out there. That treatment isn’t covered? Try negotiating how doctors bill for the service.
Her new coverage kicks in later this spring. She says already, she’s initiating these kinds of conversations with providers.
Life changes complicate coverage, for better and for worse
24-year old Nathaniel Scott, of Philadelphia, is exactly the kind of guy insurers and health leaders want in the marketplace. He’s young and healthy. And while he doesn’t make a lot of money, he still sees value in having health insurance. What if the unexpected happens, and he needs emergency care?
“And then after I get out, I get a bill from the hospital for thousands and thousands of dollars,” says Scott. “And then my head’s spinning saying, ‘oh my goodness, how am I going to pay all this?!'”
Even with this enthusiasm, Scott faced several unanticipated challenges that nearly derailed his efforts to get covered.
Scott specializes in tech and computer support, but his employment situation has been tenuous. Promising full-time work with benefits fell through when the sequester hit last year, so in November he looked into health insurance on his own through the Marketplace.
Like many others, Scott fell into a technical labyrinth of lost applications and inaccurate account information. By December, he’d figured most of that out and decided on the cheapest option presented to him at just under $200 a month. It’s a catastrophic plan, available to young people, but he didn’t realize until several weeks later that he’d still have to pay a lot out of pocket – $6,000 – before any coverage would kick in.
Though he doesn’t feel any urgency, Scott says at some point he would like new glasses and a physical, so he can be eligible for a driver’s permit.
With such high out-of-pocket costs, however, he debated dropping the coverage. He weighed that against wanting to be prepared for the unexpected. Scott lives with his younger sister, and just over a year ago, their mother died.
“With everything falling on me now being head of the household, there’re other people I have to think of, not just myself.”
In a positive turn, Scott gained more steady contract work in January. But on a less positive note, his sister received notice that her Medicaid coverage was terminating.
Both of these factors further complicated Scott’s insurance situation.
On his own, Scott’s changing income may ultimately make him eligible for cheaper health coverage. That’s because the baseline to qualify for federal subsidies is 100 percent of the federal poverty level. If you make below that and depending on the state, a person is either eligible for Medicaid, like in New Jersey and Delaware, or not eligible for anything, like in Pennsylvania.
Scott also wanted to see about adding his now uninsured sister, a part-time student with no income, to his insurance plan. The process would require him to file her as a dependent on his taxes. Scott sought help from a navigator and learned their combined income wouldn’t be enough to make them eligible for subsidies. Without that, the insurance was too expensive for them both.
“To be honest, I’m still as confused today as I was when I first started enrollment back in early November,” Scott says.
Area navigators say many families have been reassessing their tax dependency status to find more affordable insurance. Assistor groups also anticipate more people turning to them for help even after the enrollment deadline, as people’s incomes and family dynamics change and require updates to their insurance.
For those who do experience a so-called life-changing event, like a new job, the government is granting them a special enrollment period.
As for Scott, he ultimately switched his catastrophic plan to one that’s a bit more expensive, about $200 a month, but covers more things. He wishes it were cheaper, but at this point, he says he’s tired of dealing with it.
“It’s nice to have it than to not have it,” he says.
In the meantime, he’s keeping his fingers crossed he’ll get more work, and trying to help out his sister, who recently incurred several medical bills, as much as he can.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.