Does enhanced HPV knowledge among teens and parents increase vaccination rates? Penn study says no
Listen-

-

-
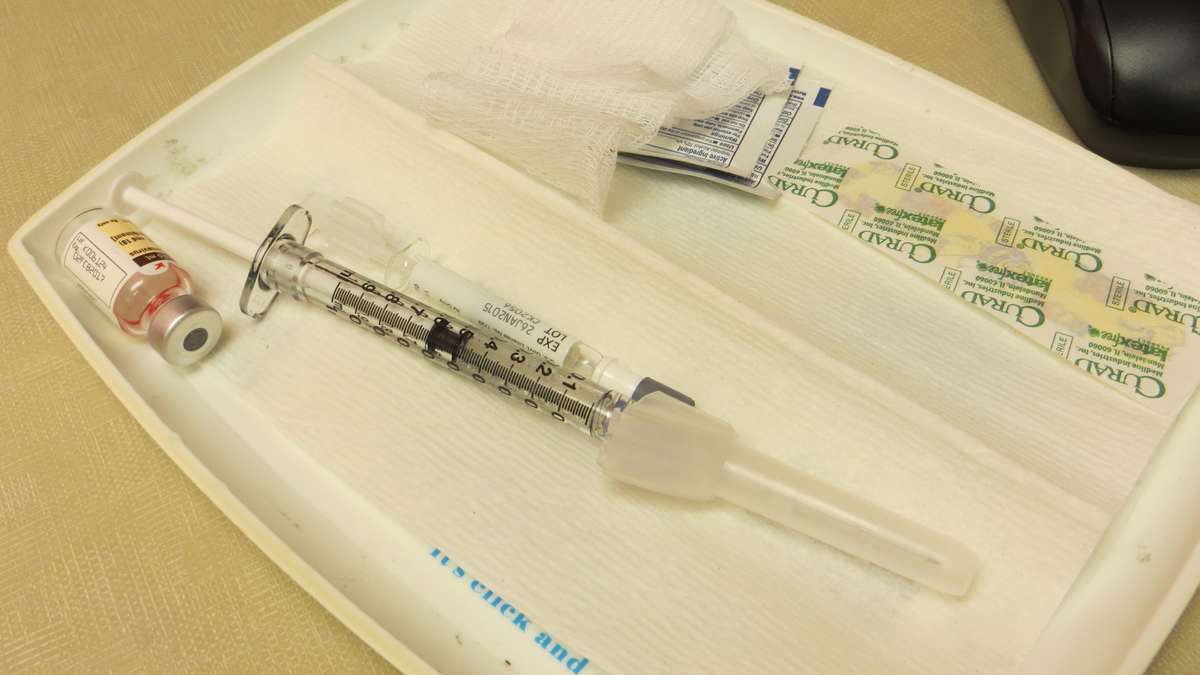
-
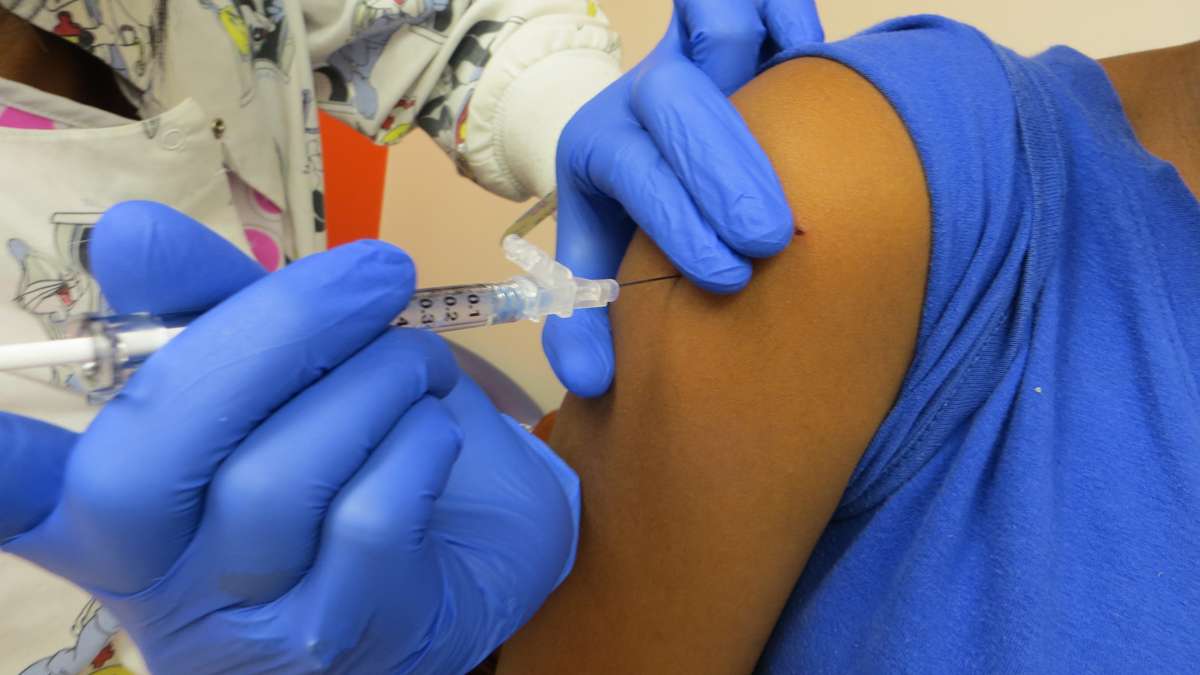
The Centers for Disease Control and Prevention recommends the vaccine against the Human papillomavirus for girls and boys age 10 or 26. (Taunya English/WHYY)
-

12-year-old Pearl Miller got her second HPV vaccine last month, and according to health officials that puts her ahead of lots of other young girls around the country.
The Centers for Disease Control and Prevention says not enough children are protected from the Human papillomavirus. The infection is spread during sex, and most often picked up by young people in their teens and 20s. It’s the virus that causes genital warts and can lead, later in life, to cervical cancer in women and certain throat cancers in men.
The CDC says girls and boys should get the HPV vaccine around age 11 or 12 to make sure they’re protected years before they start having sex.
The vaccine is a cancer-prevention tool, and that’s why so many public-health experts think it’s important.
The CDC has invested lots of dollars in vaccine-education campaigns and public service announcements on HPV, but despite efforts to get the word out, the percentage of kids who get the HPV vaccine is much lower than for the other shots recommended for pre-teens.
Encouraging a change in doctor behavior
A new study from the University of Pennsylvania questions whether improving knowledge among parents and kids actually works to improve vaccination rates. Maybe it’s doctors that need a bit more education and training.
Behavior scientist Jessica Fishman studies why people make healthy choices. She says in public health the thinking goes like this: If people have the right information, they’ll take the right steps.
“There’s been a lot of emphasis on: ‘If only they knew, if only they knew,'” Fishman said.
Her team at the University of Pennsylvania surveyed low-income girls and their parents in Philadelphia to find out what those families know about the virus and the vaccine. The study is reported in the journal Pediatrics.
The researchers wondered: Does having better HPV information mean you’re more likely to get the shots?
“It didn’t really make a difference if you had the knowledge or not,” Fishman said.
That finding is a break from what many people in public health have believed for years. Fishman says colleagues warned her: “Don’t do the study. Don’t waste your time.”
“There’s sometimes a surprising amount of politics in science, so there are people who have argued for a long time that knowledge must be the key,” Fishman said. “We find something that doesn’t support that argument, and it can be troubling, or upsetting or surprising to people.”
Fishman is not troubled. She says it’s important to figure out what’s not working, so you can start searching for true solutions. Instead of focusing on what kids and parents know and do, she says, maybe there’s an opportunity to change the behavior of doctors or the health system.
One idea is to make sure there’s a ready, on-hand supply of the vaccine in doctor’s offices. Another system change is to program the electronic medical record so doctors get an alert when the child in front of them hasn’t had his or her HPV shot.
Switching from conversations to strong recommendations
Fishman says doctors are pretty direct when they talk to parents about TDAP or the Meningococcal vaccine. TDAP is a booster shot that protects against tetanus, diphtheria and whooping cough. The meningococcal vaccine fights bacteria that cause meningitis.
The vaccine rate for those shots hovers around 80 or 85 percent. By contrast, depending on the year, only about 53 to 58 percent of girls nationwide have had their first dose of the HPV vaccine, and coverage is even lower for boys.
Fishman says doctor-parent chats can get confusing when it comes to HPV.
“A lot of physicians sometimes recommend the other two, and then when it comes to HPV, they’re like, ‘We’ll let’s start a conversation about this,'” Fishman said. “They’re sort of like: ‘This is something we can talk about and explore, and you don’t have to get it now.’ And it’s not clear to the patient or the parent that this is a recommended vaccine just like the other ones.”
One study found that when a doctor is faced with a “vaccine-hesitant” family, sometimes he or she will agree to delay the HPV shots as a “bargaining chip” to get parents to buy-in to the other vaccines first.
Hal Byke leads Nemours du Pont Pediatrics in Wilmington. He doesn’t offer teen vaccines as if they’re on a menu at a restaurant.
“Would you like this, or would you like this?” he said. “I say these are the things they are getting, and the parent can say: ‘I don’t want it.'”
Byke says he and other doctors at the Jessup Street health center present the HPV vaccine with the same emphasis and importance as the other recommended shots, which may contribute to the fact that the HPV vaccine rate at the Jessup Street center is higher than national averages.
According to health system data, among girls between the ages of 13 and 17, 68 percent have had at least one HPV immunization and 49 percent have had all three shots. Among boys aged 13 to 17, 64 percent have had at least one HPV immunization. Thirty-two percent have had all three.
Emphasizing life-long protection
When Nemours pediatrician Gina Amoroso speaks with 12-year-old Pearl Miller and her mom, her message is cancer prevention—and the reasons not to delay.
“There’s actually been some recent research that’s indicated that the sooner you get the three in, the better the protection you have life long,” she said.
Amoroso says it’s actually the first conversation about HPV that can be tricky. That’s when parents push back and have a few reservations, she said.
“The most common is: ‘My child’s not sexually active so it’s not something I need to do right now.”
Nemours pediatrician Colleen Witherell’s response is: Sure, we all hope kids don’t have sex early, but parents can never predict when a child will have his or her first sexual encounter.
“We want to catch them well before. If it’s 13 or 30, you want them to be protected,” she said.
Carla Miller did ask a few questions, but says she believed the doctor when she said the vaccine could protect Pearl later in life.
“My hope is that they have a trust in me from the day they bring me their child so that when they turn 11, they’re looking at me right direction and guidance,” Amoroso said. “It is extremely powerful to be able to prevent a cancer.”
Improving rates in Philadelphia
In Philadelphia, HPV vaccination rates are lower than health officials hope but are actually some of the best in the nation.
The city has a $600,00 grant from the CDC this year to help improve HPV vaccination rates.
The plan includes reminder postcards and phone messages sent to the parents of teenagers. Pediatricians also train other doctors to overcome barriers when they discuss the vaccine with moms and dads.
Claire Newbern manages the epidemiology unit at the Philadelphia Department of Public Health where she helps make sure the city’s immunization program hits its goals.
She says the city has done very well getting children the first dose in the three-shot HPV series. Getting healthy, busy teenagers to come back to the doctor for the second and third shots has been harder.
“We’ve heard from our providers that they see [teens] less,” Newbern said. “You are lucky to get ’em in once a year in the fall.”
While system changes and doctor education are both important, Newbern isn’t ready to stop the education outreach to parents and patients.
The media campaign helps dispel myths, she said.
“I think it’s important to improve health literacy, so parents know about vaccines, even if it doesn’t have a huge payoff immediately, maybe it helps the next child, or the neighbor,” Newbern said.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



