How to prevent fatal overdoses: Surge in deaths sparks statewide trainings in Delaware
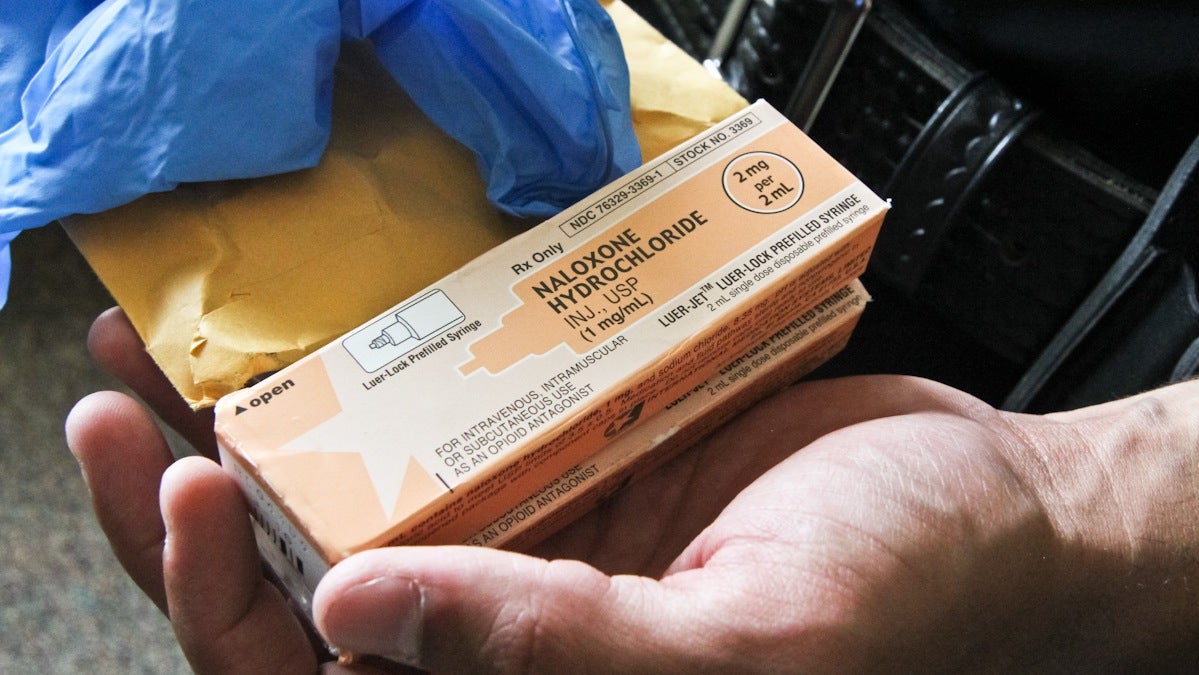
A police officer holds the drug Narcan, which can save the life of a person who has overdosed on opiates (Kimberly Paynter/WHYY)
Between November and June, Delaware experienced 124 suspected overdose deaths claiming victims from 17 to 87. That’s compared with 99 traffic deaths in all of 2013, according to the state health department, and 50 overdose deaths in all of 1999.
The surge has health advocates, public officials and even some members of law enforcement trying to get a better handle on the problem. The state recently enacted two laws aimed at equipping community members and first responders with information and tools that could help prevent future deaths.
Who’s most at risk of an overdose
When Domenica Personti, director of adolescent services and prevention at Brandywine Counseling, saw a spike in fatalities last fall, she started organizing trainings to educate the thousands of people connected to Brandywine, such as those in treatment, on how to best respond to an overdose and how to lower one’s risk or that of a loved one.
On a recent evening, she leads one such session, an hour in length, with a group of about a dozen women from a neighboring treatment program. All listen attentively as Personti goes over various prevention tips and debunks some commonly held myths.
Whether a person is a longtime user or new to drugs, she emphasizes, it only takes a little bit more than what the body is used to to overdose.
“One of the things we want to drive home, people are at higher risk in certain situations,” says Personti. “So an example of that is someone who has been sober for any period of time is at higher risk of an overdose, versus someone who’s not, because of their lack of tolerance.”
What that means, she stresses, is that those who are in treatment are often most at risk of overdosing and dying if they relapse.
Personti says the risk of dying also goes up when people use alone since there’s no chance of help if something goes wrong. People who are medically compromised, such as those with asthma, are at higher risk.
Another critical factor that elevates the risk of overdosing is mixing drugs, such as opiates with alcohol or benzodiazepines. Personti has seen that as a recurring theme in the overdose fatalities connected to Brandywine.
How to identify an overdose
An overdose occurs “when the body’s system is overloaded with a substance that’s not supposed to be there,” says Judy Cain, a registered nurse at Brandywine who’s assisting Personti at the training. Opiates act as a depressant, she explains. Take too much, and the body goes into respiratory distress.
The manner and speed at which a person responds to an overdose could mean the difference between life an death, Personti tells the group. An oxygen-deprived brain can suffer damage anywhere from 90 seconds to three minutes after the onset of an overdose.
And while it’s always best to err on the side of caution and call 911, some common signs may help identify an overdose.
The main sign is a lack of response.
One way to check this, Personti demonstrates, is to lift up a person’s arm. If it drops, that’s a sign he or she is unresponsive and may be overdosing.
Lips and fingertips may turn blue, and the chest may not be rising.
Personti says a user’s eyes could still be open amid an overdose, though he or she still wouldn’t be responding to any stimulus.
Cain goes over how to do a sternal rub — rubbing knuckles firmly on the sternum — to see if there is any reaction.
How to react (and how not to react) to an overdose
If someone is overdosing, the most important thing is to stay with him or her and to call for help, says Personti.
She acknowledges some may fear sticking around when police arrive, due to their own criminal records. She and others point to a “Good Samaritan” law enacted last year that aims to provide at least some degree of legal immunity to a bystander calling for help.
“Consider the person you’re with,” Personti tells the group. “Even if you are putting yourself in a risky position legally, your friend could still be alive.”
Cain says performing rescue breathing can be critical in those intermediary moments.
Common myths for combating overdoses include throwing a person in a cold shower, dropping ice in their pants, and putting warm milk up their nose. And some of these approaches may be more harmful than helpful, Cain and Personti caution.
Quick medical attention, including the use of nalaxone, can be a lifesaving treatment, they say.
Expanding access to nalaxone to community members, police
The recently enacted laws in Delaware will expand Brandywine’s prevention trainings to the community at large across the state. That way, friends and loved ones can also have access to more resources. But the law will also allow community members who go through the training to get a prescription for nalaxone.
So if someone is overdosing, instead of waiting critical minutes for help to arrive, a bystander can administer what could be a life saving, overdose-reversing drug, says supporters of the law.
“You can’t do anything to help a person person if they’re not alive,” says Rep. Mike Barbieri, D-Newark, a main sponsor of both laws. “So the first thing we have to do is keep them alive.”
Some critics worry that access to nalaxone might embolden users to not fear overdosing. Barbieri says the laws are first steps in a much broader effort to get a handle on a growing drug epidemic.
The other law would give police officers the option to carry nalaxone. At least 15 other states have similar programs.
The community trainings are still in the works, but the state health department hopes to launch them later this fall. Personti and Cain think the more people know about what to do in those critical moments when someone is overdosing will save lives.
“Just knowing what to do in the event when someone overdoses gives someone one more chance than they had,” says Personti. “Those minutes, even just doing rescue breathing, even calling 911, even the Good Samaritan law, those things will increase the likelihood of survival from an overdose.”
Austi Gilbert, who was at the Brandywine training, agrees, saying she found the presentation to be very useful, especially when it comes to recognizing signs of an overdose.
“I think if someone was overdosing around me, this would help a lot,” says Gilbert, 24. “I think I could definitely help save them now.”
The Rehoboth resident became addicted to heroin several years ago, after taking painkillers for a toothache. Like many at the training, she has lost someone close to her due to an overdose. It was about a year ago, she says, and while she did call 911, it wasn’t enough.
“It was very scary. It was very sad,” she says.
She thinks having nalaxone on hand in that situation could have helped.
This story was originally produced for the Sept. 19 episode of “First,” Delaware’s public media newsmagazine, which airs Friday evenings at 5:30 and 11 p.m. on WHYY-TV. Once archived online, the video version of this story can be accessed here.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.



