ICUs give life-saving treatment to many patients with ‘do not resuscitate’ orders
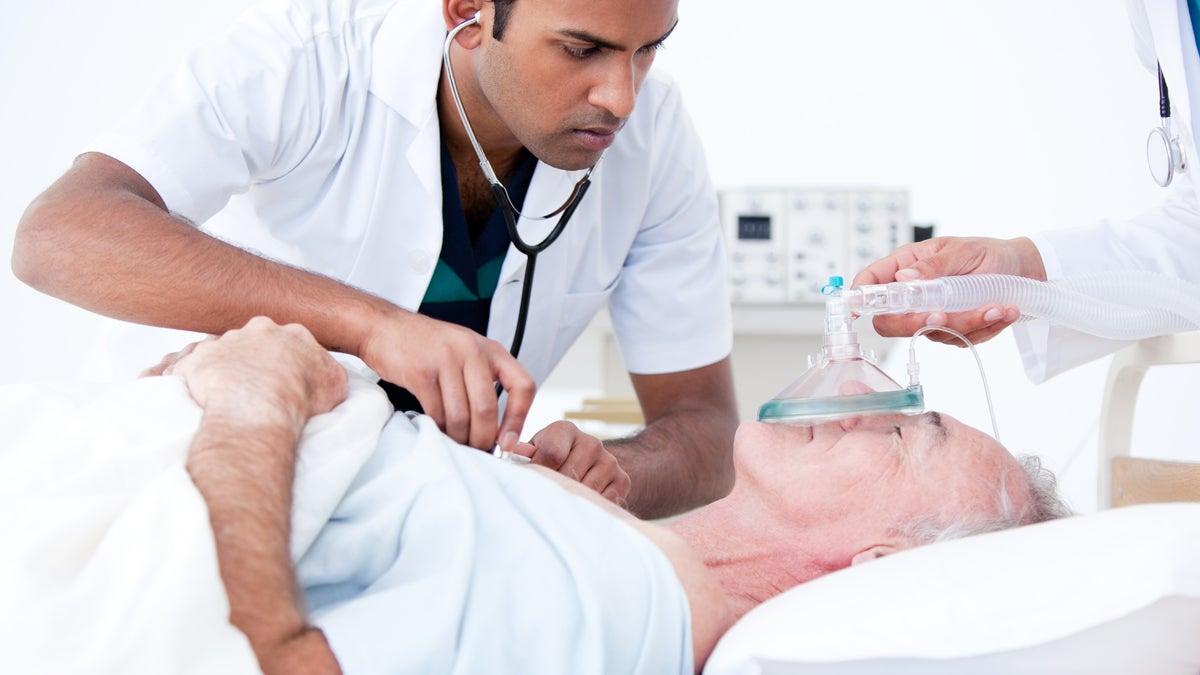 Photo via ShutterStock) " title="shutterstock_51877480" width="1" height="1"/>
Photo via ShutterStock) " title="shutterstock_51877480" width="1" height="1"/>
(Photo via ShutterStock)
Whether a sick patient with a “do not resuscitate” order still gets CPR might depend on where that patient is hospitalized.
Researchers from the University of Pennsylvania surveyed 141 intensive care units in hospitals across the country and found dramatic variation in how units treated patients who entered with requests for limited intervention. Some ICUs provided CPR to those patients in under 4 percent of cases. Others administered the lifesaving technique more than 90 percent of the time.
“It was very clear that some ICUs tended to be more aggressive in treating otherwise similar patients,” said Scott Halpern, a critical care physician and senior author of the study, which was published this week in the journal JAMA Internal Medicine.
Overall, nearly a quarter of patients entering with a DNR ended up receiving CPR. Survivors were also more likely to leave the ICU with their treatment limitations reversed rather than putting new restrictions in place.
The researchers did not have enough information to tell whether the more extreme care was ultimately requested or administered against a patient’s wishes. Some patients, for example, likely changed their mind about treatment while in the hospital.
“We don’t know what the right rate of providing CPR or other forms of life support for patients who have already expressed treatment limitations is,” said Halpern. “But presumably that rate shouldn’t vary across ICUs.”
The wide variation is disturbing, he said, and implicates the culture of particular ICUs.
“It strikes me that we can do a lot to improve on patient-centered decision making by better understanding how these cultures evolve and how they can be changed,” said Halpern.
For patients, Halpern advises discussing end-of-life care with family members, who can help make sure advance directives are followed in the hospital.
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.

