Why does information about vaccines and COVID keep changing?
The messages shift and can be confusing. WHYY’s Health Desk Help Desk talked to public health communicators about, well, communication.

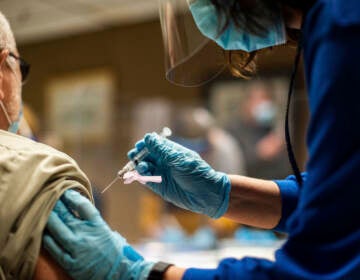
Zaliyah Dozier, an 11th grader at Lankenau high School, gets her first shot of the COVID-19 vaccine during a clinic at the Philadelphia Zoo. (Emma Lee/WHYY)
Ask us about COVID-19: What questions do you have about the coronavirus and vaccines?
This is one of a series of articles in which reporters from WHYY’s Health Desk Help Desk answer questions about vaccines and COVID-19 submitted by you, our audience.
If she had a time machine, Andrea Wojcik says, there’s one thing she would change about the beginning of the coronavirus pandemic: She would advise public health officials to explain clearly that much is unknown — and that information and recommendations will change.
“We eventually learned that, but I think that was a lesson that came a little too late, and unfortunately it led to additional confusion,” said Wojcik, section chief of the office of communications for the Delaware Department of Health and Social Services.
“I think that everybody kept saying, ‘This is new, this is new, this is new,’” she said. “But that doesn’t necessarily translate to the message of, ‘Things can change, and things can evolve, so we will provide that new information as soon as we have it.’”
If that simple message had been conveyed early on, perhaps it would have meant fewer people bewildered today, during the pandemic’s fourth wave, about coronavirus variants, and vaccine boosters, and breakthrough infections, among other things. WHYY’s Health Desk Help Desk often receives questions ranging from how the virus spreads to why anyone who’s been vaccinated should even have to worry about getting sick anymore. All of us have been inundated with evolving scientific data and shifting recommendations around masks and physical distancing, not to mention misinformation and disinformation on social media. So effective public health messaging is crucial, Wojcik said.
“People have lots of emotions and opinions, rightfully so, around their health. And sometimes, it can get easily confused when they see so many different forms of information or pieces of information coming from different sources. It can make it hard to know what is the correct piece of information,” Wojcik said. “So hopefully, the public health agency in whatever state or town that they are in provides that source of solid, reliable information for them to make those informed decisions about their own health.”
But on the national level, a lot of messaging mistakes were made in spring 2020, at the beginning of the pandemic, said Sarah Bass, associate professor of social and behavioral sciences at Temple University’s College of Public Health, and director of the Risk Communication Laboratory.
One of those mistakes, she said, was not using core crisis communication principles.
“If we don’t come out at the beginning and say, ‘Hey, we don’t know everything about this, our understanding is changing as the research is happening and as we see things,’ then the public takes everything that’s been said as verbatim,” Bass said.
“And then, if things start to change, the public looks at it and says, ‘Well, you don’t really know what you’re talking about, because you said this first, and then it was different.’”
One of the reasons some people won’t get vaccinated, according to Temple University surveys, is because they believe health officials don’t know what they’re doing, she said.
Another error on the federal level, Bass said, was that there was not one identifiable spokesperson with straightforward messaging. That confusion at the top hurt state and local governments by making them look less credible, she said.
“You had the politicians say one thing. You had public health being kind of buried a little bit, and you had Dr. Fauci up there trying to get the right information out. But sometimes, what you need is one coherent spokesperson who has that credibility,” Bass said.
“It was, ‘Well, this isn’t a big deal,’ or, ‘It is a big deal and you should quarantine in your house,’ or, ‘You don’t have to wear a mask,’ but then, ‘You do have to wear a mask,’ ‘Oh, you need to wipe every item that you have down with Clorox,’ or, ‘Never mind, you can’t get this virus that way,’” Bass said. “So there were a lot of those mixed messages at the beginning. And I think that just set us up for so much misinformation. And quite honestly, disinformation that’s done on purpose as a way to kind of sow discord and not having confidence in the messaging that’s coming out.”
‘We want certainty’
Tom Hipper is the associate director of the Center for Public Health Readiness and Communication, and an assistant professor at the Dornsife School of Public Health at Drexel University. A failure in communication early on set the precedent for the rest of the pandemic to date, he agreed.
“As is the case with pretty much any health emergency or crisis, we are dealing with a lot of uncertainty. And uncertainty is not something that anyone likes or is comfortable dealing with. We want certainty. We want clear answers. And we want them pretty quickly in the midst of a crisis,” Hipper said.
“In times of great uncertainty, when people are stressed and concerned, I think the tendency is to calm people, to over-reassure them, to focus on the information that is known … but it’s equally important to acknowledge what isn’t known,” he said. “Doing so engenders trust and understanding, and not doing so can breed mistrust and confusion and cause people to look elsewhere for information.
“We need to … remind people that changing guidelines don’t mean that public health agencies are incompetent or health officials don’t know what they’re doing. Quite the contrary. Changing guidelines means that we are committed to learning more about this virus and to arm you with the latest information, to protect yourself and your family, even if that means changing our previous recommendations,” he said.
But it’s not too late to correct the wrongs, Hipper argued — he wishes public health officials were less scripted and tapped into people’s understanding that everyone is human.
“I’d love to see more health officials acknowledge the public’s frustration of the perception of these ever-changing guidelines … I’d like to see health officials acknowledge the sometimes frustratingly slow pace of science, and how difficult it is to deal with uncertainty when we’re 18 months into this and still desperate for answers, and do more to share the challenges behind making these kinds of policy decisions with incomplete information,” he said.
“I think more of that humility, coupled with reminders that we’re continuing to work relentlessly to get people the best information we can to keep them safe, would really go a long way in this space … give people a peek behind the curtain … and a reminder that people in public health are working as hard as they’ve ever worked to understand this virus and to help us figure out a way out of this,” Hipper said. “Seeing these folks work around the clock and all with the same odds of getting through this horrible stretch, it’s been really, really inspiring. And I would love to see that story get told a bit more.”
What public health officials are doing
Wojcik said she can’t think of another time in history that Delaware’s health department had a website dedicated to a single health crisis. It’s also the first time the health department has used multiple social media platforms. For instance, it’s using TikTok to reach 18- to 34-year-olds. On the video-sharing platform, people tell stories of their personal struggles with long COVID symptoms, or about missed life experiences and the importance of getting vaccinated to get back to normal.
Tapping into people’s emotions is much more likely to resonate than scientists providing statistics about mRNA vaccines, Wojcik and Bass said.
“When you’re talking to the average person who is very emotional because they didn’t get to go on their dream honeymoon because travel was restricted due to COVID, or they had to leave their dream job because sometimes they can barely get off the couch anymore, that feels very real. And these people are coming from a place of emotion and making it a lot easier to convey that, quite honestly, in a way that people relate to,” Wojcik said.
Delaware’s health department also is working to eliminate jargon-filled language in its messaging, because it can confuse people, she said.
“We were just discussing today internally with the communications staff about going through the website and starting to simplify some of the language. We hear this information from our community partners. So we’re updating some of our materials now to be more simplified and understandable,” she said.
Some of the most effective public health messaging campaigns have had a local theme, addressing what the community is looking forward to doing once the pandemic is over, Hipper said.
“Anything we can do to instill that community lens here — we are in this together, and really the only way we get out of it is together as well,” he said. “I know that’s really difficult to do when it seems like we’ve never been more at odds politically or value-wise. But I think it just makes it all the more imperative that we don’t give up on that front.”
Going directly to the community also has been effective, the experts agreed. Funded by the health department, Temple University experts meet Philadelphians one-on-one. Bass said it takes time for the public to build trust.
“Sometimes, the first time we talk to them is not going to convince them. So it’s really letting people vocalize how they’re feeling, what their worries are, talking to them about those worries,” she said. “And it’s, very honestly, very labor-intensive, because you may not get that person to say yes the first time you talk to them. But if they hear it again, you might get them to the point where they do, because they have talked to you enough that they trust you at a personal level.”
Listening, showing empathy, validating concerns, connecting people to trusted sources, and having access to vaccines are the best ways to promote the COVID-19 shot, Hipper said.
“Everyone, including me, wants there to be a magical, one-size-fits-all message that suddenly resonates with everyone and flicks that switch to widespread vaccination. In reality, this issue of vaccine hesitancy is multifaceted, and our strategy needs to account for this,” he said.
Part of that strategy is hearing people out and not talking down to them, Hipper said.
“It is frustrating for those working in public health and health care who, frankly, have never worked harder, who have witnessed so much suffering despite the availability of a safe and effective vaccine, who continue to be patient and listen. But it’s vital that we continue to do that, and recognize that not doing so is going to alienate those who have yet to get the vaccine,” he said.
“It’s very easy to lump anyone who hasn’t been vaccinated yet as an anti-vaxxer. And I think that’s inaccurate and also problematic with respect to our way forward,” Hipper added. “To this day, I continue to hear from friends and family who remain stressed about the conflicting information that they’re coming across on various platforms, and they seek clarity or reassurance. Others may be open to getting the vaccine, but find the prospect of having to take a day off from work or having to take a day off if they experience a day worth of side effects following a shot to be a very real challenge. The point is, not everyone is a conspiracy theorist — although they certainly do exist and get plenty of attention.”
Public health messaging needs to appeal to everyone, the experts said. So health departments are trying to reach people from all angles.
“I think it is multifaceted in that it has to be in a variety of different places that people hear it, but it has to be in places that people trust information coming from,” Bass said. “So for communities of color, for example, hearing it in a doctor’s office actually may not be the best place to hear it if they have mistrust of the medical system and research in general. And then it’s better to have this more community-based approach, where they’re actually talking to people either that they know or people that they see as part of their community.”
Yet confusion continues
We are bombarded with scientific information, but many people are still confused about how viruses behave and how vaccines work.
For example, people have unrealistic expectations about vaccine effectiveness, the health experts said.
No vaccine is 100% effective and breakthrough infections have always existed. But many people believe the COVID-19 shot does not work because of rare breakthrough cases that usually are mild.
The reality is that vaccines are meant to prevent hospitalizations and death — but that message wasn’t driven home enough, the experts said.
“COVID is around to stay, just like the flu is and the cold is … The vaccines help us control it, and that they aren’t 100% effective. But I think the message that most people got was that, ‘I’m going to get this vaccine and now I’m safe from ever getting it,’” Bass said.
“This idea that ‘Oh, well, you could get it’ is surprising to them, even though I think we tried to say, ‘It may not keep you from getting infected, but it will keep you from getting super sick, getting hospitalized and dying.’”
It’s a message that needs to be repeated more frequently, Hipper said.
“I think sometimes you get stuck in the weeds on the data and don’t make that very basic, but incredibly important point enough,” he said. “I think it’s important to normalize this idea of breakthrough cases, that people know that that’s not unique to the vaccine. And this occurs with every vaccination.”
Health officials should promote the fact that the Food and Drug Administration approved the Pfizer vaccine and that the Centers for Disease Control and Prevention recommends pregnant women get the shot to drive home the fact that the vaccines are safe, Hipper said.
Messaging surrounding the recent White House booster recommendation could have been clearer, Hipper said. The rationale behind boosters needs to be explained to the public with data-driven, clear information, especially when they’re also hearing messages that it’s important to get the unvaccinated vaccinated.
“To be clear, this doesn’t mean that offering boosters isn’t necessarily the right next step or that making boosters widely available will significantly hinder the need to get more people vaccinated,” Hipper explained. “But these are understandable concerns that folks have that need to be clearly addressed when policy announcements like that are made. And I would argue this recent announcement would have been strengthened with more clear evidence that walks people through what led to this significant decision.”
Misinformation and disinformation
Delaware’s Department of Health and Social Services has a team of people who read comments on social media and hide those with blatantly false information.
Studies show that when one piece of negative information is shared, it needs to be countered by at least three positive pieces of information, said Bass, from Temple’s College of Public Health. But at this point, she said, the false information has become so ingrained that countering it is difficult.
“I think at this point, the only way you get that group to get vaccinated is some of these, ‘You don’t have a job unless you get vaccinated,’ or, ‘You can’t get on an airplane unless you’re vaccinated,’ or, ‘You can’t go to this concert,’’ Bass said.
Still, Hipper argued, there are some strategies that can be successful in combating false information. That includes explaining to people how bad actors profit off promulgating conspiracy theories.
“We could be doing so much more to make this clear to people, so that they can better understand how and why they’re being misled and manipulated,” she said.
Public health experts also should “prebunk” false information, or as Hipper explained, “inoculate people against the bad information before they’re exposed to it.” That involves integrating health and science literacy into formal curriculum, so that people can be empowered to spot misinformation and disinformation.
Hipper adds that public health also needs to be better funded to prepare for health crises.
“Once COVID-19 is here and it’s affecting people, we dump a bunch of money at the problem, when putting money into this years ago to build up our personnel and our planning would have been much more cost-effective and much more effective overall,” he said.
“It was gut-wrenching, frankly, to hear at the very outset of this pandemic, ‘No one could have predicted this.’ And I can tell you that’s simply not true,” he said. “This idea of a novel virus and what it could mean and the extent to which we were prepared to deal with it is what kept a lot of folks in public health up at night. And yet, we’ve been dealing with fewer and fewer resources, cutting key personnel, and just not having the bandwidth to set up these systems for real-time surveillance data collection.”

Get daily updates from WHYY News!
WHYY is your source for fact-based, in-depth journalism and information. As a nonprofit organization, we rely on financial support from readers like you. Please give today.





![CoronavirusPandemic_1024x512[1]](https://whyy.org/wp-content/uploads/2020/03/CoronavirusPandemic_1024x5121-300x150.jpg)



